Blog & News
SHADAC Comments on Proposed 2025 American Community Survey Health Insurance Coverage Instrument Changes
January 07, 2024:The U.S. Census Bureau has released a request for comments regarding proposed revisions and changes for the 2025 American Community Survey. Based on information gained from the 2022 Content Test, proposed changes would affect a variety of topics and questions, including educational attainment, disability, household roster, and, most notably for the State Health Access Data Assistance Center (SHADAC), health insurance coverage.
See an excerpt regarding ACS health insurance coverage question changes below. You can find the full request for comments here in a notice from October 20, 2023.
| Health Insurance Coverage - Since implementation in 2008, research has found that Medicaid and other means-tested programs are underreported in the ACS and the PRCS and that direct-purchase coverage is overreported, in part due to misreporting of non-comprehensive health plans and reporting multiple coverage types for the same plan (Mach & O'Hara, 2011; Lynch et al., 2011; Boudreaux et al., 2014; O'Hara, 2010; Boudreaux et al., 2011; Boudreaux et al., 2013). Moreover, revisions to the health insurance question would help capture changes to the health insurance landscape that occurred with and since the passage of the Patient Protection and Affordable Care Act. Changes to the health insurance coverage question include a change in formatting of the question that adds an explicit response category for those who are uninsured, reordering some response options and rewording response options for direct purchase, Medicaid, employer, and veteran's health care. |
Researchers at SHADAC have reviewed the proposed changes regarding health insurance coverage data collection for the American Community Survey 2025 data year. We have crafted the following response letter discussing our opinion that the implementation of these changes be postponed in order to further investigate causes of Medicaid underreporting, and to allow for the ACS 2025 to adequately reflect effects of the Medicaid unwinding.
SHADAC’s Comments
We appreciate the opportunity to comment on Census’ proposed changes to the 2025 American Community Survey questionnaire. For more than twenty years, the State Health Access Data Assistance Center (SHADAC) has used the American Community Survey (ACS) to provide state officials and other stakeholders with data to inform health policy. Since the health insurance question was added in 2008, we have used the ACS to monitor changes in health insurance coverage.
As frequent and knowledgeable users of the survey, we have a particularly vested interest in the continued ability of the ACS to produce a high-quality measurement of health insurance coverage. With that in mind, we submit the following comments on the proposed changes to the health insurance coverage instrument. We strongly urge postponing the implementation of the proposed changes to the ACS’ health insurance coverage instrument with reasons provided below:
Medicaid Underreporting
While heartened by the commitment to improvements in the measurement of health insurance coverage, we are very concerned that the most recent content test showed significantly reduced reporting of Medicaid coverage in both versions of the test questions.
Given that this request for comment specifically mentions addressing the long-standing problem of Medicaid underreporting as a goal of the new instrument, we view this increase in Medicaid underreporting as disqualifying. In our view, Census needs to conduct further investigation to determine the cause for this demonstrated decrease in Medicaid reporting and use that information to revise the test questions to address this substantial problem.
Timing and Medicaid Unwinding Data
Though we understand that the timing for this change is driven by Census’ standard process for adding or changing survey content, we view the proposed timing of this change as inappropriate because of the ongoing, large-scale redetermination of Medicaid eligibility (“unwinding”) that began in April 2023 with the end of the pandemic-era continuous coverage requirement. This unwinding will continue into 2024.
The unwinding of the Medicaid continuous coverage requirement represents the largest nationwide coverage transition since the Affordable Care Act, and there is significant interest in monitoring the impacts. ACS data year 2025 will be the first full year of data after the completion of the unwinding.
If changes to health insurance coverage questions are implemented in 2025, we will never be able to reliably learn about the full impacts of the unwinding on health insurance coverage. Postponing revisions would allow us to better compare data and understand the impacts of the unwinding on key populations in the first full year post-unwinding completion. This is especially important for state-level populations of interest (including those relevant to furthering critical health equity goals) and for substate geographies, as the ACS is the only source of this information.
Thank you for your consideration. We know you face many important decisions and appreciate the chance to comment on this important and impactful data collection change.
See SHADAC’s comments on the newly proposed Sexual Orientation and Gender Identity (SOGI) questions on our blog here.
Blog & News
California Achieves Lowest Uninsured Rate Ever in 2022 (Cross-Post)
November 13, 2023:The following blog is cross-posted from The California Health Care Foundation.
Author: Lacey Hartman, Senior Research Fellow, SHADAC
Maintaining Gains Hinges on Transitioning People Who Lose Medi-Cal to Other Coverage in Coming Months
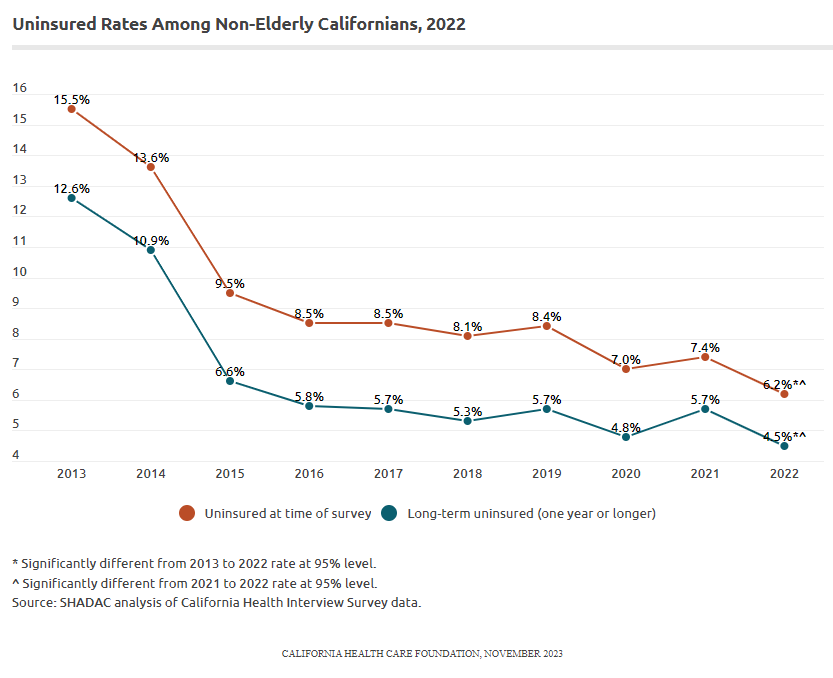
The share of Californians under age 65 (“nonelderly”) without health insurance reached a historic low in 2022. Based on the most recent California Health Interview Survey (CHIS), the percentage of nonelderly Californians without health insurance dropped to 6.2% in 2022, a statistically significant decline from 2021 (7.4%). The rate of nonelderly people without coverage for a year or more also reached a historic low in 2022. Commonly called the “long-term uninsured,” their rate dropped from 5.7% in 2021 to 4.5% in 2022, another statistically significant decline.
Disparities in Coverage by Race and Ethnicity Narrow, but Inequities Persist
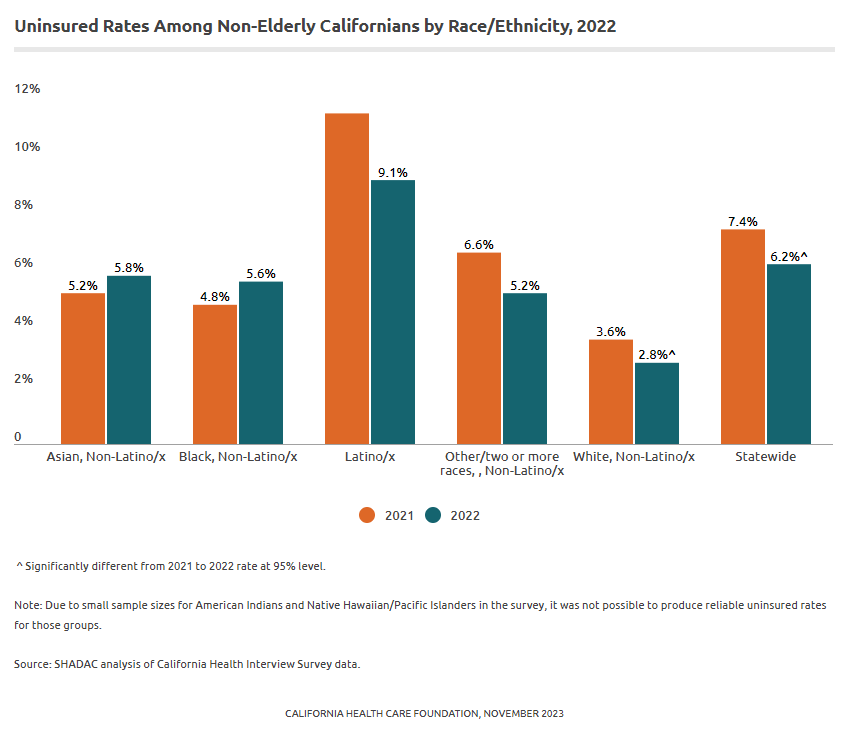
California’s Latino/x population experienced the largest improvement in coverage between 2021 and 2022; the share who reported being uninsured at the time of the survey dropped from 11.4% in 2021 to 9.1% in 2022, a change that was statistically significant. The Latino/x rate in 2022 also represents a historic low for this group.
The uninsured rate for White Californians also declined by a statistically significant but smaller amount, from 3.6% to 2.8%. There were no other statistically significant changes between 2021 and 2022 by race/ethnicity. Although there have been important gains in narrowing disparities in coverage by race and ethnicity in the state, Latino/x Californians continue to be uninsured at rates triple that of their White counterparts. Black and Asian Californians are uninsured at twice the rate of White Californians. Due to small sample sizes for American Indians and Native Hawaiian / Pacific Islanders in the survey, it was not possible to produce reliable uninsured rates for those groups.
Discussion
The fact that fewer nonelderly Californians were without coverage in 2022 than ever before is clearly good news. However, in 2023, the federal continuous coverage requirement for Medicaid came to an end. It’s estimated that as many as 2–3 million Californians may leave Medi-Cal as a result. How many Californians ultimately lose their Medi-Cal coverage and whether those leaving the program get connected to other coverage will have a huge impact on the state’s uninsured rate going forward.
These issues — as well as other challenges, such as inflation — may make holding onto California’s coverage gains difficult in the coming years. It will be vital to continue monitoring data from 2023 and future years to fully understand the impact of the pandemic — and the end of associated coverage protections, as well as other policy changes — on California’s health coverage landscape.
Blog & News
2022 ACS Tables: State and County Uninsured Rates, with Comparison Year 2021
November 17, 2023:Each year, SHADAC uses data released from the American Community Survey (ACS) via the U.S. Census Bureau's data.census.gov tool to produce estimates of uninsurance at the state and county level.*
Click on a state below in the interactive map to see a PDF table of uninsured rates by state and sub-state geographies, but also by demographic characteristics (e.g., age, race/ethnicity, and poverty level) for 2022 and comparison year 2021.
Click here to view uninsurance estimates for the United States.
Click here to view uninsurance estimates for Puerto Rico and its municipios.
Note: These tables present uninsured rates, which indicate the share of the population that is uninsured. For example, a 10 percent uninsured rate for adult women indicates that 10 percent of all adult women are uninsured.
Maps & Tables of Private, Public, & Uninsured Changes from 2021 to 2022
- Private Coverage Rates by State, Change from 2021 to 2022, for All People
- Public Coverage Rates by State, Change from 2021 to 2022, for All People
- Uninsurance Rates by State, Change from 2021 to 2022, for All People
About the ACS
The ACS is a household survey that began in 2005 and produces annually updated data on a variety of population characteristics, including health insurance coverage. In total, the ACS surveys approximately three million U.S. households each year. An important feature of the ACS is that it includes a large enough sample for state‐level and sub‐state estimates.
The ACS began asking survey respondents about health insurance coverage during the 2008 calendar year. Specifically, the survey asks respondents about current coverage for each person in the respondent’s household. A person is categorized as “insured” if he or she has coverage at the point in time at which the survey is administered.
*Why Aren’t Estimates Provided for All Counties?
Due to sample size constraints, single-year ACS estimates are available at the county level only for counties with a population greater than 65,000.
How Are These Estimates Different from the Estimates that SHADAC Publishes Using Census Bureau Micro-Data Files?
Two definitions used by the Census Bureau to generate the tabulations above differ from those that SHADAC uses to generate tabulations for State Health Compare. The definitional differences are as follows:
Family
The Census Bureau defines a family as “all related people in a household.”
SHADAC defines a family using a measure called the “Health Insurance Unit” (HIU), which includes all individuals who would likely be considered a family unit in determining eligibility for either private or public coverage.
To learn more about the 2020 update of SHADAC's Health Insurance Unit (HIU) see our HIU resource page, which houses two issue briefs: The first describes the SHADAC HIU, its purpose, the most recent update, and improvements to HIU data inputs; and the second outlines the impacts of using the SHADAC HIU in analysis so that researchers can assess whether the SHADAC HIU is suitable for their research and what the potential impacts of its use might be. The page also provides a link to STATA and SAS codes to aid in the use of the HIU variable.
Family Income
The Census Bureau determines family income as a percentage of the Federal Poverty Level (FPL), which is a definition of poverty used primarily for statistical purposes. For example, FPL is used to estimate the number of Americans living in poverty each year.
SHADAC determines family income as a percentage of the U.S. Department of Health and Human Services’ Federal Poverty Guidelines (FPG), which is a measure used for administrative purposes. For example, FPG is used to determine eligibility for federal programs such as Medicaid and the Supplemental Nutrition Assistance Program (SNAP).
To learn more about the difference between FPL and FPG, read our updated blog post from April 2023.
Related ACS Materials:
- An Annual Conversation with the U.S. Census Bureau: 2022 Health Insurance Coverage Estimates from the ACS and CPS
- 2022 ACS: Declining Uninsured Rates for the U.S. and States are Supported by Private and Public Coverage Increases
- CPS ASEC: 2022 National Health Insurance Coverage Estimates Show Falling Rates of Uninsurance and Direct-Purchase Coverage (Infographic)
Publication
An Annual Conversation with the U.S. Census Bureau: 2022 Health Insurance Coverage Estimates from the ACS and CPS
On Thursday, September 28th at 1:00 PM CST, SHADAC hosted a webinar covering the release of new 2022 health insurance coverage estimates from two key, large-scale federal data sources: The American Community Survey (ACS) and the Current Population Survey (CPS).
Estimates from both surveys were presented at: the national and state levels, as well as by coverage type, and a range of other demographic categories (age, geography, poverty level, and more), during the webinar. Technical and analytic insight was provided from experts at the U.S. Census Bureau, which administers both the ACS and CPS, and SHADAC researchers joined with our special guests from the Census Bureau to answer questions from attendees after the presentation.
Attendees were able to learn about:
- New 2022 health insurance coverage estimates
- When to use which estimates from the ACS vs the CPS
- How to access the estimates via Census reports and the data.census.gov website
- How to access state-level estimates from the ACS using SHADAC tables and State Health Compare web tool
Speakers
 Kathleen T. Call, Moderator Kathleen T. Call, Moderator
Principal Investigator
SHADAC Dr. Call has been an Investigator with SHADAC since its launch in 2001. She is also a Professor in the Division of Health Policy and Management at the University of Minnesota (UMN), School of Public Health (SPH). She demonstrates her commitment to community-engaged scholarship through her leadership in the Clinical and Translational Science Institute, and the Interdisciplinary Research Leaders (IRL) program, and by co-chairing the UMN, SPH Health Equity Work Group.
|
 Katherine Keisler-Starkey, Speaker Katherine Keisler-Starkey, SpeakerEconomist in Health and Disability Statistics Branch United States Census Bureau Katherine Keisler-Starkey is an economist in the Health and Disability Statistics Branch in the U.S. Census Bureau’s Social, Economic and Housing Statistics Division. In her position, Ms. Starkey provides subject matter expertise on health topics for the Current Population Survey Annual Social and Economic Supplement (CPS ASEC) and has authored the Census Bureau’s Health Insurance Coverage in the United States report for the last four years. Her research interests focus on Applied Microeconomics, including Health Economics, Public Finance, and Labor Economics, and she is the author of several topically focused Census working papers and blogs in these areas. |
 Robert Hest, Speaker Robert Hest, SpeakerSenior Research Fellow
SHADAC Robert Hest joined SHADAC in 2017 and was recently made Senior Research Fellow. Mr. Hest provides expertise in survey data, data analysis and processing, and project management. Mr. Hest also manages SHADAC’s State Health Compare website, coordinating data processing, quality assurance, dissemination, and documentation of data.
|
 Sharon Stern, Speaker Sharon Stern, SpeakerAssistant Division Chief
United States Census Bureau Sharon Stern is the Assistant Division Chief for employment characteristics in the U.S. Census Bureau’s Social, Economic and Housing Statistics Division. In her position, Ms. Stern oversees statistics on the labor force, health insurance and disability from several Census Bureau surveys. She has authored a wide variety of Census Bureau reports and papers on topics related to poverty, disability, and health insurance.
|
Related Resources
SHADAC
- Webinar slides from SHADAC
- CPS ASEC: 2022 National Health Insurance Coverage Estimates Show Falling Rates of Uninsurance and Direct-Purchase Coverage (Infographic) (Blog)
- 2022 ACS: Declining Uninsured Rates for the U.S. and States are Supported by Private and Public Coverage Increases (Blog)
U.S. Census Bureau
- Webinar slides from Census Bureau
- Health Insurance Coverage in the United States: 2022 (Report)
- Health Insurance Coverage of U.S. Workers Increased in 2022: Health Insurance Rates for Working-Age Adults Higher by Race, Hispanic Origin, Region (Blog)
- Uninsured Rates Decreased in Over Half of U.S. States in 2022: Changes in Types of Health Insurance Coverage Contributed to Declines in Uninsured Rates From 2021 to 2022 (Blog)
Blog & News
2022 ACS: Declining Uninsured Rates for the U.S. and States are Supported by Private and Public Coverage Increases
Setember 14, 2023:
Related Releases and Materials
|
The U.S. Census Bureau released 2022 health insurance coverage estimates from the American Community Survey (ACS) today, which included state-level information about health insurance coverage by type as well by certain demographic categories. The Census Bureau also released an accompanying report and blog post highlighting many of the changes seen from 2021 to 2022.
Overall, the data showed a drop in uninsured rates, with an 8.0% rate of uninsurance in 2022 as compared to 8.6% in 2021. This echoes similar year-over-year decreases in uninsurance shown in data from the Current Population Survey (CPS), for which estimates were released on Tuesday, and in recent survey data from the National Health Interview Survey (NHIS). Eight percent represents the lowest-ever national rate of uninsurance measured in the ACS.
The national decline in uninsurance was supported by decreases in 27 states, with Maine the only state to see an increase in its uninsured rate, from 5.7% in 2021 to 6.6% in 2022, reversing the previous trend from 2019 to 2021.* Overall, uninsured rates ranged across states from a low of 2.4% in Massachusetts to a high of 16.6% in Texas, a continuing trend from past years. The largest drop in uninsured rates was found in Oklahoma, which fell by 2.1 percentage points (PP) to 11.7% in 2022 from 13.8% in 2021.
The drop in uninsured rates coincided with small yet significant increases in 2022 for both private coverage — 67.2% from 67.0% in 2021 — and public coverage — 37.2% from 36.8%. Alaska saw the largest increase in private coverage, rising 2.2 PP to 66.4%. Nine states saw increases in private coverage, while nine states saw decreases in private coverage. And unsurprisingly, Oklahoma saw the largest increase in public coverage, rising 2.3 PP to 39.6%: Oklahoma was one of two states, along with Missouri to have expanded Medicaid in 2022.
The rest of this blog post highlights some of the national and state-level changes that took place between 2021 and 2022 in the broadest categories of insurance (uninsurance, public coverage, and private coverage) for two key age groups, nonelderly adults (age 19-64) and children (age 0-18). Accompanying interactive maps allow readers to view and sort the different coverage types for each age group.
Key Findings from the 2022 ACS: Nonelderly Adults (19-64)
Figure 1. Changes in state-level coverage rates among nonelderly adults, 2021-2022
State-Level Uninsurance
Nonelderly adults also saw falling uninsurance rates, dropping by 0.9 PP from 12.2% in 2021 to 11.3% in 2022. Additionally, 31 states saw decreases in their uninsured rates for nonelderly adults while only Maine saw an increase, rising 1.4 PP to 9.6%. The largest decline in uninsurance was seen in Oklahoma, whose rate of uninsured nonelderly adults dropped a notable 3.4 PP to 16.8% in 2022.
State-Level Private Coverage
Private coverage increased significantly for nonelderly adults, rising 0.7 PP to 73.4% in 2022 from 72.7% in 2021. This increase was echoed across 21 states, with Mississippi seeing the largest increase at 2.2 PP, rising to 69.7% in 2022. Private coverage levels fell across just three states — Maine, Minnesota, and Virginia — with Maine seeing the most significant drop, falling 1.8 PP to 74.1% in 2022.
State-Level Public Coverage
Overall, nonelderly adults also experienced a significant increase in public coverage from 2021 to 2022. Rates of public coverage rose to 19.4% from 19.1% in 2021, driven by similar increases across 14 states. Individually, Oklahoma once again saw the largest increase — 19.9%, up from 16.3% in 2021. Of the eight states that saw decreases in 2022, public coverage for nonelderly adults declined the most in Rhode Island, dropping 2.1 PP to 21.7
Key Findings from the 2022 ACS: Children (0-18)
Figure 2. Changes in state-level coverage rates among children, 2021-2022
State-Level Uninsurance
For children, uninsured rates fell to 5.1% in 2022 from 5.4% in 2021. Fourteen states also saw drops in children’s uninsurance, Wyoming being the largest - falling 3.5 PP to 7.9%, followed by New Mexico, which saw a 2.6 PP decrease from 6.4% in 2021 to 3.8% in 2022. Three states (Connecticut, Pennsylvania, and Wisconsin) saw increased children’s uninsured rates for 2022.
State-Level Private Coverage
Unlike nonelderly adults, children did not experience an overall increase in private coverage for 2022. Private coverage remained statistically unchanged for children nationally at 60.6%. However, 13 states did see rising private coverage rates, with Rhode Island leading the way, jumping 4.8 PP to 69.4% in 2022. Six states saw declines in private coverage, led by a drop of 2.3 PP in Missouri, whose rate of private coverage for children in 2022 was 63.2%.
State-Level Public Coverage
Like private coverage rates, public coverage remained statistically unchanged for children from 2021 to 2022, sitting at 39.6%. Just eight states saw increased public coverage for kids in 2022, led by a 2.6 PP jump in North Dakota, from 21.3% in 2021 to 23.9% in 2022. And seven states saw declining public coverage rates, with children in Rhode Island experiencing a precipitous fall of 5.9 PP to 34.4% in 2022.
Future Data Releases and Products
Supplemental tables for the 2022 ACS 1-Year Estimates will be released from the U.S. Census Bureau on October 19, 2023, and 2018-2022 ACS 5-Year Estimates will be available on December 7, 2023.
Stay tuned for more granular details about insurance coverage changes in the states from 2021 to 2022 via customized SHADAC tables examining coverage at the state and county level, and for an announcement of updated health insurance coverage measures available on State Health Compare.
Notes
All changes described in this document are significant at the 90% level. Private coverage includes individually purchased, employer-sponsored coverage, and TRICARE military health coverage Public coverage includes Medicare, Medicaid/CHIP, and VA health care. Public and private coverage types are not exclusive and include individuals with those types of coverage alone or in combination with other coverage. Estimates represent the civilian noninstitutionalized population.
Overarching estimates of uninsurance and public and private coverage are for all ages, except where noted for children (age 0-18) and nonelderly adults (19-64).
COVID-19 Public Health Emergency Impacts
Continuous Coverage Requirement
The continuous coverage requirement that prevented states from terminating individuals’ Medicaid coverage during the pandemic ended on March 31, 2023. The resumption of Medicaid eligibility redeterminations and renewals (and potential disenrollments), a process commonly referred to as the “unwinding,” began on April 1, 2023, and each state has a year to navigate a return to normal operations while also meeting reporting requirements set by CMS for publicly sharing coverage transitions and outcomes data during this time. While the health insurance estimates released by the US Census Bureau for 2022 precede the beginning of the unwinding process, the data provide an essential baseline for understanding how health insurance coverage is distributed across the U.S. and among the states prior to the unwinding, as well as marker to measure the impacts of this seismic coverage transition as potentially millions of individuals, both adults and children, are poised to lose Medicaid and must either find another form of coverage (e.g., state-based marketplace or employer-sponsored insurance [ESI]), or risk becoming uninsured.
Several resources have been compiled by SHADAC to track the unwinding process in a variety of avenues, falling under several broader categories:
Guidance for States
- Using Surveys to Monitor Coverage Transitions During the Unwinding of the Medicaid Continuous Coverage Requirement
- Best Practices for Publicly Reporting State Unwinding Data
Health Insurance Coverage Data Tracking
- State-Based Marketplace Transition Data During the Unwinding
- State Dashboards to Monitor the Unwinding of the Medicaid Continuous Coverage Requirement
- Tracking Health Insurance Coverage During the Unwinding: Monthly Data from the Household Pulse Survey
*Data Collection and Dissemination
As has been extensively documented by both SHADAC and the Census Bureau, disruptions to data collection and dissemination efforts—as well as the presence of significant nonresponse bias—due to the COVID-19 pandemic heavily impacted estimates for 2020. As such, the Census Bureau released 2020 ACS 1-year data in an “experimental-only” format and cautioned against their use. Similarly, the Census Bureau recommends that data users do not compare 2020 ACS 1-year experimental estimates with any other data. Researchers therefore have compared 2019 to 2021 data.













