Publication
Data to Inform Research on Integrated Care for Dual Eligibles
This report by SHADAC researchers Lacey Hartman and Elizabeth Lukanen, conducted with support from the Arnold Ventures Foundation, summarizes the findings of a systematic review of data sources that could be used to study the broad topic of integrated care for dual eligibles. The paper concludes with a set of recommendations aimed at addressing key data gaps and advancing the availability of comprehensive, high-quality data for research in this area. In addition to this report, SHADAC has produced a companion Excel table that contains the full abstraction details for each data source.
This work was supported by the Arnold Ventures Foundation.
Blog & News
New SHADAC Resource Explores and Evaluates Available Data Sources to Research Integrated Care for Dual Eligibles
April 1, 2021: The importance of improving care for individuals enrolled in both Medicare and Medicaid (dual eligibles) has received considerable attention in recent years.1,2,3 Extensive research has shown that dual eligibles account for a disproportionate share of spending within both programs, and the lack of integration between the two programs contributes not only to excess costs but also lower quality care.4,5,6 As a result, states and the federal government have developed a variety of models aimed at improving integration of care for dual eligibles.
The importance of improving care for individuals enrolled in both Medicare and Medicaid (dual eligibles) has received considerable attention in recent years.1,2,3 Extensive research has shown that dual eligibles account for a disproportionate share of spending within both programs, and the lack of integration between the two programs contributes not only to excess costs but also lower quality care.4,5,6 As a result, states and the federal government have developed a variety of models aimed at improving integration of care for dual eligibles.
A new report by SHADAC researchers Lacey Hartman and Elizabeth Lukanen, conducted with support from the Arnold Ventures Foundation, describes the strengths and limitations of existing data sources that could be used to study the broad topic of integrated care for dual eligibles. A primary focus is whether these data can address research questions aimed at improving care for dual eligibles. The paper summarizes findings by assessing the data sources across four focus areas that are critical to research aimed at dual eligibles: 1) enrollment in integrated care models; 2) analysis of priority subpopulations; 3) LTSS; and 4) enrollee social needs.
The report provides a systematic review of 34 data sources that can produce nationally representative estimates for dually eligible individuals (and/or estimates for all 50 states) and have the potential to inform research on integrated care models. Selections were made based on SHADAC’s extensive prior knowledge in working with a wide variety of data sources, our recent work developing an inventory of evaluations of integrated care models, and a scan of relevant and widely used data repositories such as the Research Data Assistance Center (ResDAC) and the Chronic Condition Data Warehouse (CCW).
The paper also provides an overview of important gaps and deficiencies within the data (and their implications for researchers seeking to evaluate the impact of integrated care for dual eligible) and concludes with a set of recommendations aimed at addressing these gaps and advancing the availability of comprehensive, high-quality data for research in this area.
In addition to this report, SHADAC has produced a companion Excel table that contains the full abstraction details for each data source.
References
1 Rizer, A. COVID-19: If ever there was a time to care about Medicare-Medicaid integration, it’s now. Arnold Ventures. https://www.arnoldventures.org/stories/covid-19-if-ever-there-was-a-time-to-care-about-medicare-medicaid-integration-its-now/
2 Center for Health Care Strategies (CHCS). (2021). Promoting integrated care for dual eligibles (PRIDE). https://www.chcs.org/project/promoting-integrated-care-for-dual-eligibles-pride/
3 Integrated Care Resource Center (ICRC). (2021). Home. https://www.integratedcareresourcecenter.com/
4 Medicaid and CHIP Payment and Access Commission (MACPAC). (2020). Integrating care for dually eligible beneficiaries: Background and context [Report to Congress on Medicaid and CHIP; Chapter 1]. MACPAC. https://www.macpac.gov/wp-content/uploads/2020/06/Chapter-1-Integrating-Care-for-Dually-Eligible-Beneficiaries-Background-and-Context.pdf
5 Medicare Payment Advisory Commission (MedPAC). (2020). Dual-eligible beneficiaries [Data book; Section 4]. MedPAC. http://www.medpac.gov/docs/default-source/data-book/july2020_databook_sec4_sec.pdf?sfvrsn=0
6 Medicare-Medicaid Coordination Office. (2015). Fiscal year 2015 report to Congress. Centers for Medicare & Medicaid Services (CMS). https://www.cms.gov/Medicare-Medicaid-Coordination/Medicare-and-Medicaid-Coordination/Medicare-Medicaid-Coordination-Office/Downloads/MMCO_2015_RTC.pdf
Blog & News
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey (Update: Jan 20 to Feb 1)
February 11th, 2021:Newly available COVID-19 vaccines promise to help protect individual Americans against infection and eventually provide population-level herd immunity. However, while the pace of COVID-19 vaccinations has picked up somewhat in recent weeks, the overall rollout thus far has remained somewhat slow and inconsistent. The initial groups prioritized for vaccination were health care workers on the front lines of the pandemic and nursing facility residents, many of whom are especially vulnerable to COVID-19 infection and severe outcomes.
While these groups continue to hold priority in vaccination slots, in response to reports of vaccines lingering unused and criticism from the public that limitations on vaccinations have too far slowed progress toward herd immunity many states have also recently begun expanding vaccine access to other (still high-priority) segments of the general population such as older adults, K-12 and child care workers, and those with high-risk medical conditions. However, there are concerns that these prioritization decisions and the existing mechanisms of the vaccine rollout—in addition to evidence that lower-income individuals, people of color, and individuals without strong connections to the health care system are less likely to get vaccinated—could worsen existing pandemic-related health inequities.
The available data have not assuaged these concerns, and show patterns of lower vaccination rates among people with lower incomes and levels of education, and marginalized racial and ethnic groups. The U.S. Census Bureau recently released updated data on take-up of COVID-19 vaccines from the most recent wave of its Household Pulse Survey (HPS), collected January 20-February 1, 2021.1 The HPS is an ongoing, weekly tracking survey designed to measure impacts of the COVID-19 pandemic. These data provide an updated snapshot of COVID-19 vaccination rates and are the only data source to do so at the state level by subpopulation. This blog post presents top-level findings from these new data, focusing on rates of vaccination (one or more doses) among U.S. adults (age 18 and older) living in households and comparing to results from the previous wave of the HPS, collected January 6-18.2
Roughly 13 percent of adults received a vaccination, but this varied by state
According to the new HPS data, 13.2% of U.S. adults had received one or more COVID-19 vaccinations during this two week period in January through February, though this varied by state from a low of 8.6% in Alabama to a high of 23.2% in Hawaii and Alaska. More than one in six adults had received a vaccine in eight states: Alaska, Hawaii, Indiana, Mississippi, New Mexico, Oklahoma, South Dakota, and West Virginia.
Vaccination rates increased substantially across nearly all states
Nationally, adult vaccination rates were up from the previous wave of the HPS, increasing from 7.7% in January 6-18 to 13.2% in January 20-February 1. Most states also experienced increases in their vaccination rates, though again the size of these increases varied across the states, from an increase of just 0.5 percentage points (PP) in Montana to an increase of 10.5 PP in Mississippi. Vaccination rates more than doubled in eight states: California, Florida, Indiana, Mississippi, Nevada, New York, South Carolina, and West Virginia.
Percent of Adults Who Had Received a COVID-19 Vaccine
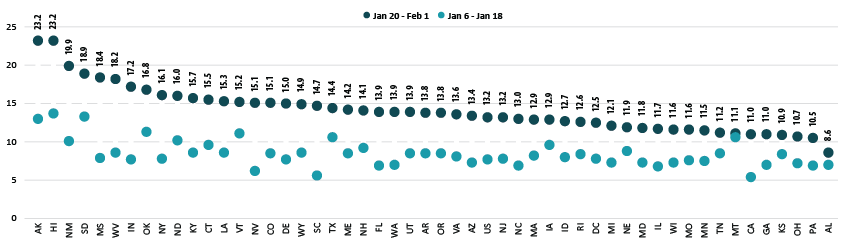
Disparities in vaccination rates remain, though some have narrowed
COVID vaccination rates continued to vary to a great degree by demographic and socioeconomic factors, though disparities narrowed slightly from previous weeks.
This narrowing could be due to the expansion of priority groups to include a broader share of the population over this period; however, progress has remained limited in getting vaccines to certain groups such as low-income and Hispanic adults, for instance, and new vaccination strategies may be needed to reach the hardest-to-reach groups such as these.
By race and ethnicity, non-Hispanic Asian and non-Hispanic White adults continued to have above-average vaccination rates at 19.5% and 14.0%, respectively. Vaccination rates among non-Hispanic adults identifying with multiple races or “some other” race increased relative to the average, rising to 13.1%, nearly in line with the national average of 13.2%. Rates among non-Hispanic Black adults (11.0%) and Hispanic/Latino adults of any race (9.4%) remained below the national average.
Percent of Adults Who Had Received a COVID-19 Vaccine by Race/Ethnicity
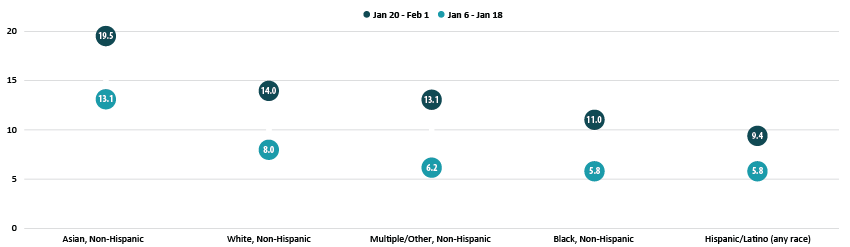
Disparities in vaccination rates by income narrowed somewhat, though those with the highest incomes continued to be much more likely to have received a vaccine compared with those with lower levels of income. Of adults with incomes of $100,000 or more, 18.0% had received a vaccination compared to just 6.6% of those with incomes less than $25,000. This pattern was broadly consistent across the states, and in nearly all states, adults with incomes of $100,000 or greater were more likely to have received a vaccine than the state overall.
Percent of Adults who Received a COVID-19 Vaccine by Income
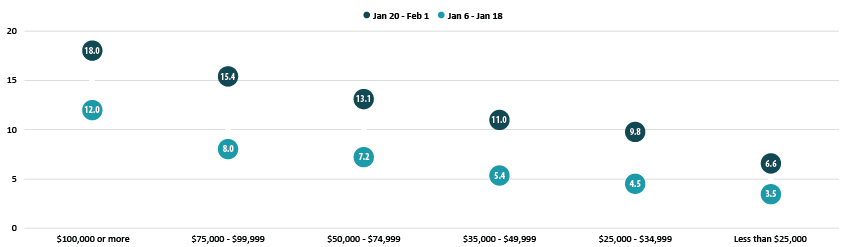
Disparities by level of education did not appreciably narrow, with adults holding a bachelor’s degree or higher having the highest vaccination rate at 20.2% and adults without a high school diploma having the lowest vaccination rates at 6.2%. These rates remained stable in relation to the national average compared with earlier in the month, and similar disparities were common across nearly all states.
At least 1 in 5 older adults received a COVID vaccine as the U.S. and many states made large progress in vaccinating older adults
Nationally, 20.4% of older adults (age 65 and older) had received at least one dose of the COVID-19 vaccine, which was more than seven percentage-points higher than among all adults (13.2%). Vaccination rates for older adults range from 8.5% in Minnesota to 56.0% in Alaska. Older adult vaccination rates were below 10% in three states (Kansas, Nebraska, and Minnesota) and above 30% in nine states (Alaska, Colorado, Florida, Georgia, Indiana, Louisiana, Mississippi, North Carolina, and Oklahoma) and the District of Columbia (D.C.).
The U.S. and nearly all states made large progress in vaccinating older adults compared with earlier in the month when older adults were no more likely to have received a vaccine than adults overall. This change was likely a reflection of many states’ recent expansion of vaccine prioritization for the general older-adult population and is heartening, considering that older adults are more likely to develop severe COVID-19 cases or die from the disease as compared to the general population.
Most states saw large increases in rates of vaccination among older adults, though from a relatively low baseline. Compared to earlier in January, 43 states and D.C. more than doubled their 65+ vaccination rates, with 26 of those at least tripling their rates. Only Minnesota failed to make substantial progress, increasing its older-adult vaccination rate to just 8.5% from 8.2% earlier in January, an increase of less than a percentage point.
Percent of Adults Age 65+ Who Had Received a COVID-19 Vaccine
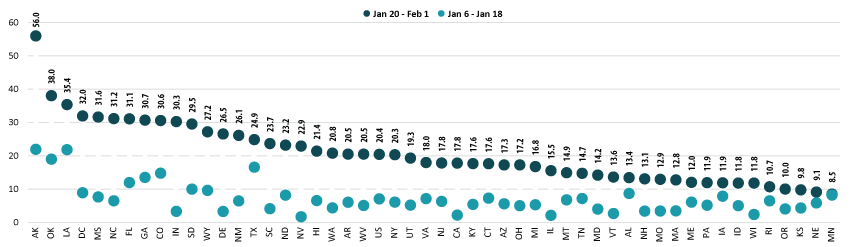
Notes about the Household Pulse Survey Data
The estimated rates presented in this post were calculated from the count estimates published by the Census Bureau. Though these counts are accompanied by standard errors, standard errors are not able to be accurately calculated for rate estimates. Therefore, we are not able to determine if the differences we found in our analysis are statistically significant or if the estimates themselves are statistically reliable. Estimates and differences should be assumed to have large confidence intervals around them—especially for subpopulations at the state level—and caution should be taken when drawing strong conclusions from this analysis. However, the fact that patterns of inequities in other vaccination rates are mirrored by these early indications of COVID-19 vaccination inequities demonstrates reason for concern.
Though produced by the U.S. Census Bureau, the HPS is considered an “experimental” survey and does not necessarily meet the Census’s high standards for data quality and statistical reliability. For example, the survey has relatively low response rates (7.5% for January 20-February 1), and sampled individuals are contacted via email and text message, asking them to complete an internet-based survey. These issues in particular could be potential sources of bias but come with the tradeoffs of increased speed and flexibility in data collection as well as lower costs. A future post will investigate differences between COVID vaccination rates estimated from survey data (such as the HPS) and administrative sources. The estimates presented in this post are based on responses from 80,567 adults. More information about the data and methods for the Household Pulse Survey can be found in a previous SHADAC blog post.
Related Reading
COVID-19 Vaccination Rates: New State-level and Subpopulation Evidence from the Household Pulse Survey (Jan 6 to Jan 18) (SHADAC Blog)
Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (SHADAC Brief)
New Brief Examines Flu Vaccine Patterns as a Proxy for COVID – Anticipating and Addressing Coronavirus Vaccination Campaign Challenges at the National and State Level (SHADAC Blog)
Ensuring Equity: State Strategies for Monitoring COVID-19 Vaccination Rates by Race and Other Priority Populations (Expert Perspective for State Health & Value Strategies)
SHADAC Webinar - Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (February 4th) (SHADAC Webinar)
Publication
Comparing Federal Government Surveys That Count the Uninsured: 2020
With the release of new insurance coverage estimates from surveys conducted by the U.S. Census Bureau, the Agency for Healthcare Research and Quality (AHRQ), and the Centers for Disease Control and Prevention (CDC), SHADAC has updated our annual “Comparing Federal Government Surveys that Count the Uninsured” brief.
The brief provides an annual update to comparisons of uninsurance estimates from four federal surveys:
- The American Community Survey (ACS)
- The Current Population Survey (CPS)
- The Medical Expenditure Panel Survey - Household Component (MEPS-HC)
- The National Health Interview Survey (NHIS)
In this brief, SHADAC presents current and historical national estimates of uninsurance along with the most recent available state-level estimates from these surveys. We also discuss the main reasons for variation in the estimates across the different surveys as well as possible reasons for incomparability of estimates across and within the surveys.
Download a PDF of the Comparing Federal Government Surveys Brief.
Last year’s brief with data from 2019, and certain 2018 data, can be accessed here.
Blog & News
Exploring Strategies to Fill Gaps in Medicaid Race, Ethnicity, and Language Data
October 1, 2020:The following content is cross-posted from State Health and Value Strategies. It was first published on October 1, 2020.
Authors: Elizabeth Lukanen and Emily Zylla, SHADAC
As states seek to address the social determinants of health and advance health equity, they face longstanding and persistent challenges in collecting complete, accurate, and consistent race, ethnicity and language (REL) data. This expert perspective provides an overview of current REL data collection standards; ideas for increasing completeness in data by engaging the enrollee and enrollment assisters, and modifying enrollment and renewal interface; and provides suggestions for how states could leverage alternative sources of data in order to improve REL data completeness.
Background
Collecting standardized patient demographic and language data across health care systems is an important first step toward improving population health, identifying areas of health disparities, and addressing health equity and social risk factors. As seen during the recent COVID-19 pandemic, for example, disaggregated demographic data is critical to identifying problems, implementing solutions, and evaluating impacts. To-date, the amount of unknown race data varies in Medicaid programs across the country. Recently the Centers for Medicaid and Medicaid Services (CMS) classified 14 states’ Medicaid race and ethnicity data as “high concern” because more than 20 percent of the data was missing. An additional five states with more than 50 percent of their data missing were classified as unusable.1 A review of the literature confirms that the deficiencies in REL data have changed over time from one of accuracy to one of completeness. The most commonly cited REL data collection challenges include:
- Lack of mandatory reporting standards
- Rapidly changing demographics
- Evolution in how people self-identify
- Voluntary reporting
- Lack of understanding on why the data are important
- Mistrust and enrollee concerns about how data will be used
Current Standards for Collecting Race and Ethnicity Data
There is a robust body of research, guidance, and tools related to the collection of REL data in health care settings. The Department of Health and Human Services (HHS) provides guidance (but does not mandate) to use the minimum standards developed by the US Office of Management and Budget (OMB), established in 1997 (Figure 1). These standards were updated after the passage of the ACA.
| Figure 1. OMB REL Standards |
Self-identification is the preferred means of obtaining information about an individual's race and ethnicity
- Allow respondent to select multiple responses (as opposed to a “multi-racial” category)
- Collect race and ethnicity data using two questions, starting with ethnicity
- At a minimum, Office of Management and Budget (OMB) categories include:
|
OMB CATEGORIES AND DEFINITIONS FOR DATA ON ETHNICITY
|
|
|
Hispanic or Latino
|
"A person of Cuban, Mexican, Puerto Rican, South or Central American, or other Spanish culture origin, regardless of race. The term 'Spanish origin' can be used in addition to 'Hispanic Latino'."
|
|
OMB CATEGORIES AND DEFINITIONS FOR DATA ON RACE
|
|
|
American Indian or Alaska Native
|
"A person having origins in any of the original peoples of North and South America (including Central America), and who maintains tribal affiliations or community attachment."
|
|
Asian
|
"A person having origins in any of the original peoples of the Far East, Southeast Asia, or the Indian subcontinent, including, for example, Cambodia, China, India, Jap an, Korea, Malaysia, Pakistan, the Philippine Islands, Thailand, and Vietnam."
|
|
Black or African American
|
"A person having origins in any of the black racial groups of Africa. Terms such as 'Haitian' or 'Negro' can be used in addition to 'Black or African American.'"
|
|
Native Hawaiian/Other Pacific Islander
|
"A person having origins in any of the original peoples of Hawaii, Guan Samoa, or other Pacific Islands."
|
|
White
|
"A person having origins in any of the original peoples of Europe, the Middle East, or North Africa."
|
- Optional questions are recommended for collecting data on specific language spoken
- Do you speak a language other than English at home?
- Yes
- No
- What is this language?
- Spanish
- Other Language (Identify)
- Do you speak a language other than English at home?
HHS also recommends collecting more granular data that reflects the population of interest/locally relevant choices, with the following considerations:
- Make sure the categories can be aggregated back to the minimum categories above (see Figure 2.)
- Consider conducting analysis of Census data to select these options
- Rely on established coding systems such as the CDC code set for race and ethnicity
- Although “Other” is not an official OMB designation, the US Census and OMB also recommend including a “some other race” option.
| Figure 2. HHS Race and Ethnicity Collection Guidance |
|
Ethnicity Data Standard
|
Categories
|
|
Are you Hispanic, Latino/a, or Spanish Origin?
(One or more categories may be selected) a. ____ No, not of Hispanic, Latino/a, or Spanish origin b. ____ Yes, Mexican, Mexican American, Chicano/a c. ____ Yes, Puerto Rican d. ____ Yes, Cuban e. ____ Yes, Another Hispanic, Latino/a or Spanish origin |
These categories roll-up to the Hispanic or Latino category of the OMB standard
|
|
Race Data Standard
|
Categories
|
|
What is your race?
(One or more categories may be selected) a. ____ White
b. ____ Black or African American c. ____ American Indian or Alaska Native |
These categories are part of the current OMB standard
|
|
d. ____ Asian Indian
e. ____ Chinese f. ____ Filipino g. ____ Japanese h. ____ Korean i. ____ Vietnamese j. ____ Other Asian |
These categories roll-up to the Asian category of the OMB standard
|
|
k. ____ Native Hawaiian
l. ____ Guamanian or Chamorro m. ____ Samoan n. ____ Other Pacific Islander |
These categories roll-up to the Native Hawaiian or Other Pacific Islander category of the OMB standard
|
The number of response categories a state offers often will depend on format and space available (e.g., web vs paper) and whether or not a state has the staffing capacity to recode write-in responses. States are encouraged to report additional granularity where it is supported by sample size and as long as the additional detail can be aggregated back to the minimum standard set of race and ethnicity categories.
Race and Ethnicity: New Census Research
In preparation for the 2020 census, the agency conducted research to improve race/ethnicity collection.[2] The goals of the project were to increase the accuracy and reliability of reporting in the major OMB racial and ethnic categories; collect detailed data for myriad groups; and obtain lower item nonresponse rates. The research had several major findings, including:
- Reinforcing the importance of allowing multiple responses
- Suggesting that “Mark all that apply” or “Select all that apply” is better than “Select one or more”
- Using race/ethnicity terminology is less confusing than using terms like “category,” which can suggest a hierarchy
- Data collection is improved when there is a dedicated “Middle Eastern or North African” response category for race (currently classified as “White”)
- Data collection is improved when a “write-in line” is used to collect detailed American Indian/Alaskan Native (AIAN) responses, however including a limited number of conceptual checkboxes (i.e., American Indian, Alaska Native, and Central/South American Indian) decreased detailed reporting for the AIAN category. According to Census Bureau research there are hundreds of very small detailed AIAN tribes, villages, and indigenous groups. Listing the six largest American Indian groups and Alaska Native groups as checkboxes, for example, would represent only about 10 percent of the entire AIAN population. Therefore, providing a distinct write-in area was determined to be the best overall approach for eliciting detailed responses across AIAN communities and identities.
Overall, the research found evidence that a providing a combined race/ethnicity question with detailed checkboxes resulted in increased use of OMB standard categories, decreased nonresponse, and improved accuracy.
Strategies for Improving and Revising Collection Standards
Research continues to inform REL data collection efforts, and practices continue to evolve. Data collection standards change in response to research, but also in response to the rapidly changing demographics and fluidity of racial and ethnic self-identification. States should review data collection practices periodically, as well as the overall demographics of the state’s population to assure REL response options are appropriate, but only modify collection practices if needed. If modifications are needed, make sure changes do not impact the ability to compare/link your data to other sources (e.g., other state agency data, data from providers, etc.). If possible, engage enrollees and their advocates in decision-making related to how REL data are collected and get feedback on any changes that are made.
The following suggestions are strategies that states could employ to help increase REL data completeness in their Medicaid programs.
Engage Enrollees
Some Medicaid enrollees may be sensitive about answering questions about their race/ethnicity or preferred language because of concerns about discrimination. Consider the following steps to help enrollees overcome that concern:
- Conduct outreach to ask the enrollee community, and community leaders, for their input about how to best collect this information
- Proactively seek advice on why data are not being provided and how the state can improve data collection
- Collect input from stakeholders into how data are collected, defined, and used (e.g., A/B user testing, testing what educational messages work, etc.)
- Report findings back to stakeholders when data are available
- Develop a communication strategy focused on the importance of REL data collection, addressing concerns about collecting this data, and providing enrollees information specifically on:
- How are REL data used and NOT used? (e.g., can the information be used to enforce immigration laws)
- The state’s privacy policy
- Who has access to these data and how these data are protected
- Where results are reported
Engage Enrollment Assisters
Enrollment assisters (term used broadly) play a large roll in application submission and renewal. In many cases, assisters serve as trusted source of information and are well positioned to talk to enrollees about providing REL data. Like the enrollees, however, assisters may not know why REL data are being collected, how data are used and might skip questions to save time. Assisters pride themselves on being neutral and may not be comfortable making recommendations to clients about providing data. Consider the following steps to help enrollment assisters collect complete and accurate REL data:
- Develop trainings, role playing, talking points, and fact sheets that address key questions about REL data collection broadly, but also provide specific tips regarding client engagement. (Training and tools should be framed as information to educate their clients, not coerce them.) Trainings can address:
- Where in the application/renewal form or online process are REL questions asked and how can discussions about the importance of these questions be incorporated into assister workflows?
- Where can the assister send people if the client has questions or complaints about response options
- For assisters where Medicaid has a direct or contractual relationship (call center employees, contractors, grantees):
- Require training on the topic
- Make enrollee discussions about REL data part of the formalized work flow
- For the broader assister community
- Communicate with umbrella organizations that support smaller community based organizations as a way to build trust and spread the message
Modify the Enrollment/Renewal Interface
Since the implementation of the ACA, states have made significant progress in streamlining and simplifying their enrollment processes and systems. As required by the ACA, all states now have to accept Medicaid applications via multiple modes including in person, mail, telephone, and online. The following strategies could help states increase the collection of REL data through their online enrollment and renewal platforms.
- Include text, or links to text, explaining the importance of collecting REL data and how the information will be used in online forms
- Utilize hover text with links
- Provide reminder prompts: “Are you sure you want to skip this question?”
- Use research-tested messages to explain the value of collecting race, ethnicity, and language data (Figure 3)
| Figure 3. How to Message REL Data Collection |
A research study tested four messages related to the collection of race/ethnicity data and measured individual’s comfort in providing that information:
 Quality Monitoring: “…review the treatment that all patients receive and make sure everyone gets the highest quality of care”
Quality Monitoring: “…review the treatment that all patients receive and make sure everyone gets the highest quality of care”- Government Recommendation: “Several government agencies recommend we collect information…as part of a national effort to make sure all patients have access to quality health care”
- Needs Assessment: “…this will help us decide who to hire, how to train our staff better, and what health information is most helpful for our patients”
- Personal Gain: “…help us make sure you get the best care possible…”
Telling patients that this information would be used for monitoring quality provided the most comfort![]()
Source: Baker, D.W., et al. (2005). Patients’ attitudes toward health care providers collecting information about their race and ethnicity. J Gen Intern Med, 20(10), 895-900.
- Increase opportunities for enrollees to provide REL data for collection if data is missing
- Prompt near the end of the application
- Prompt when the enrollee logs in to account (e.g., when they log in to re-enroll or report changes)
- Send special email reminder to complete this information a short time after enrollment or renewal
Leverage Alternative Data Sources
Another potential strategy is to use other data sources to fill gaps or validate Medicaid data. This is a particularly successful strategy if the data source in question is more complete (e.g., Minnesota has robust provider quality reporting standards that include REL data collection). States could compare Medicaid data against other data sources to look for systematic gaps (e.g., implausibly low rates of certain races/ethnicities). In some cases, states are collecting data at several points in time – e.g., eligibility determination, enrollment into a health plan, and at the time of treatment. These data can be used together and to validate the strongest and most complete data source. Potential data sources might include:
- Encounter data collected directly or from managed care organizations
- Data from health and social needs assessments
- Vital records data
- Data from other state agencies
Leveraging other data is not without challenges and might be best approached initially as a pilot initiative. For example, data use agreements take time to execute and data linking can face technical challenges and take up scarce analyst time. Also, data from other sources often has similar issues related to quality and completeness or different issues.
1 Medicaid.gov. (n.d.). DQ Atlas: Race and Ethnicity [2016 data set]. Available from https://www.medicaid.gov/dq-atlas/landing/topics/single/map?topic=g3m16












