Blog & News
Drug overdose deaths grew by almost 30 percent in 2020
July 15, 2021:Fentanyl- and methamphetamine-type drugs surged roughly 50 percent in 2020
Drug overdose deaths surged in the United States during the first year of the COVID-19 pandemic, increasing nearly 30 percent in just 12 months. Provisional data recently published by the U.S. Centers for Disease Control and Prevention (CDC) show that more than 92,000 people died of drug overdoses in 2020—surpassing records yet again.1
The growth was widespread throughout the country, with only two states (New Hampshire and South Dakota) spared from the jump in drug overdose deaths. Conversely, some states saw their death rates increase more than 50 percent, including Kentucky, South Carolina, Vermont, and West Virginia.
Much of the growth in drug overdose deaths was driven by synthetic opioids such as fentanyl, which increased more than 50 percent from 2019 to 2020 (see Figure 1). Fentanyl has become a key product for international drug traffickers, often finding its way as an adulterant in other drugs like heroin and cocaine, and even as an ingredient in counterfeits of common opioid prescription pills such as Oxycontin. The emergence of fentanyl in the U.S. illicit drug trade is a newer phenomenon beginning in the past decade, and it has recently spread from eastern states to increasingly affect states in the western half of the country as well.
Figure 1. Changes in drug overdose deaths in the U.S., 2019 to 2020
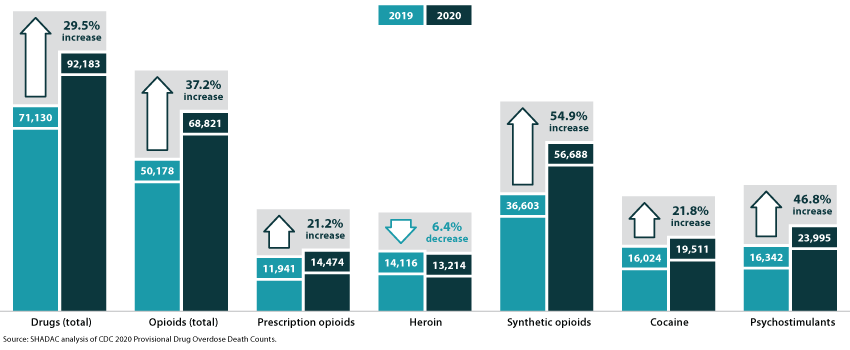
A family of drugs called “psychostimulants”—mostly methamphetamine—also drove a large increase in deaths in 2020, up nearly 50 percent since 2019. Deaths involving methamphetamine and other psychostimulants have grown dramatically in the past few years. The increased death toll involving psychostimulants is likely caused by two factors: First, the methamphetamine trafficked in the U.S. today is generally much more potent than methamphetamine sold in the past, raising the potential risk of overdoses caused by methamphetamine. Second, methamphetamine today is often contaminated with, or used alongside, synthetic opioids, raising the risk of an overdose involving the use of multiple drugs simultaneously.
Of the main drugs involved in overdoses2, only heroin was associated with a decline in deaths during 2020—falling by less than 10 percent since 2019. Meanwhile, overdose deaths involving prescription opioids increased more than 20 percent, reversing a trend of relatively stable or even declining death rates over several years. Cocaine overdose deaths similarly increased by more than 20 percent in 2020.
1 National Center for Health Statistics (NCHS). (2021, July 14). Vital Statistics Rapid Release: Provisional Drug Overdose Death Counts [Data set]. Centers for Disease Control and Prevention (CDC). https://www.cdc.gov/nchs/nvss/vsrr/drug-overdose-data.htm
2 The drug overdose death categories presented in the CDC data include: heroin, natural opioid analgesics (e.g., morphine and codeine) and semisynthetic opioids (e.g., oxycodone and hydrocodone), synthetic opioids such as methadone and synthetic opioids other than methadone (e.g., fentanyl and tramadol), cocaine, and psychostimulants.
Blog & News
New Study Shows Heightened Mental Health Burdens for Young Adults, Adults with Lower Incomes or Lower Education Levels, and Adults who Experienced Income Loss during the COVID Pandemic
July 1, 2021:As rates of COVID vaccination increase around the world and the nation, attention is beginning to turn toward addressing more of the non-physical impacts and effects of the virus, such as the mental health burdens borne by large segments of the population.1
 In a new issue brief released this week, SHADAC researchers used the U.S. Census Bureau’s Household Pulse Survey to study the relationship between the COVID-19 pandemic and mental health burdens for the United States’ adult population. Based on data gathered in April/May through December of 2020, the brief’s authors found that reported rates of combined and individual symptoms of anxiety and depression in the first part of the year were more than triple when compared with data from a similar time period in a related survey, the Center for Disease Control and Prevention’s (CDC) National Health Interview Survey (NHIS). The HPS found a rate of 35.9 percent of adults reporting anxiety or depression symptoms in April/May 2020, versus 11.0 percent from the NHIS in January-June 2019.2 And rates only continued to grow significantly throughout the remainder of 2020, reaching a peak of 41.9 percent in December.
In a new issue brief released this week, SHADAC researchers used the U.S. Census Bureau’s Household Pulse Survey to study the relationship between the COVID-19 pandemic and mental health burdens for the United States’ adult population. Based on data gathered in April/May through December of 2020, the brief’s authors found that reported rates of combined and individual symptoms of anxiety and depression in the first part of the year were more than triple when compared with data from a similar time period in a related survey, the Center for Disease Control and Prevention’s (CDC) National Health Interview Survey (NHIS). The HPS found a rate of 35.9 percent of adults reporting anxiety or depression symptoms in April/May 2020, versus 11.0 percent from the NHIS in January-June 2019.2 And rates only continued to grow significantly throughout the remainder of 2020, reaching a peak of 41.9 percent in December.
In particular, the analysis found that the highest rates of these mental health burdens were borne by younger adults, adults with less than a high school education, adults with lower incomes, and adults who experienced or anticipated job-related income loss. In each case, reported rates of anxiety or depression symptoms were significantly higher than those for the total population (41.9 percent).
In December 2020…
…younger people consistently reported the highest rates of anxiety or depression, with more than half (56.4 percent) of 18-29 year-olds reporting symptoms of anxiety or depression, a significantly higher rate than this same group reported in April/May 2020.
…roughly one-half (51.2%) of adults with less than a high school education reported anxiety or depression symptoms.
…more than half (58.2 percent) of adults with household incomes of less than $25,000 reported anxiety or depressions symptoms, a statistically significant increase over their April/May 2020 rate.
The HPS also collected data on anxiety and depression symptoms from adults who had either experienced or anticipated a job-related income loss during the 2020 year. Just over one-half of individuals (53.2 percent) who had experienced an employment income loss reported symptoms of anxiety or depression, which was significantly higher than the roughly one-third (31.5 percent) rate among people who hadn’t experienced such a loss. An even greater number of people who anticipated an employment income loss (58.0 percent) reported anxiety or depression symptoms, which was again significantly higher than the approximately one-third (35.0 percent) rate among people who didn’t anticipate such a loss.
The pandemic's toll on mental health, especially for younger adults, has become increasingly worrisome in recent months.3 Mental health burdens, such as suicide deaths, were already an area of concern prior to COVID, with rates trending upward in the years before 2020.4
It is important for policymakers, as they consider directing resources toward addressing the impacts of COVID-19 on their individual populations, to understand which groups (i.e., younger adults, adults with lower incomes and education levels, and adults who experienced income losses) might benefit most from outreach to connect them with or increase their access to mental health care services.
Explore Additional COVID-related SHADAC Work Using the HPS
SHADAC previously wrote a blog post that provided an overview of the Household Pulse Survey (HPS) methodology as well as survey and questionnaire updates.
SHADAC has also used HPS data to track vaccination rates for a range of demographic groups, producing our own state-level estimates of vaccination rates for a biweekly blog series.
Additionally, SHADAC produced a blog studying vaccine hesitancy rates among adults during the first part of 2021.
1 Tully, T. (Updated 2021, June 11). Covid-19: U.S. Vaccine Production and Supply Increase After Snowstorms Caused Delays. The New York Times. https://www.nytimes.com/live/2021/02/23/world/covid-19-coronavirus
Soucheray, S. (2021, May 28). COVID-19 vaccinations increase in US, but unevenly. Center for Infectious Disease Research and Policy (CIDRAP). https://www.cidrap.umn.edu/news-perspective/2021/05/covid-19-vaccinations-increase-us-unevenly
Abbot, A. (February 2021). COVID’s mental-health toll: how scientists are tracking a surge in depression. Nature. https://www.nature.com/articles/d41586-021-00175-z
2 The pandemic-era rates from the CDC study and the HPS are not perfectly comparable to the pre-pandemic rates from the NHIS because they come from different surveys with different methodologies. However, since they ask essentially the same questions on anxiety and depression, the rates should presumably be similar, so the substantially higher estimates in the pandemic-era surveys provide reason for concern.
3 Fernandez, M.E. (2021, March 8). AHA News: COVID-19 Mental Health Crisis Is Hitting Young Adults. U.S. News & World Report. https://www.usnews.com/news/health-news/articles/2021-03-08/aha-news-covid-19-mental-health-crisis-is-hitting-young-adults
4 Planalp, C., Hest, R., & Au-Yeung, C. (June 2020). Suicide Rates on the Rise: National Trends and Demographics in Suicide Deaths from 2000 to 2018. State Health Access Data Assistance Center (SHADAC). https://www.shadac.org/sites/default/files/publications/2020_NATIONAL-Suicide-brief.pdf
Hill, R.M., Rufino, K., Kurian, S., Saxena, J., Saxena, K., & Williams, L. (March 2021). Suicide Ideation and Attempts in a Pediatric Emergency Department Before and During COVID-19. Pediatrics, 147(3), e2020029280; DOI: https://doi.org/10.1542/peds.2020-029280
Publication
COVID-19 Pandemic Coincided with Elevated and Increasing Anxiety and Depression Symptoms
 SHADAC Director Dr. Lynn Blewett and SHADAC Researchers Colin Planalp and Robert Hest used data from the U.S. Census Bureau’s Household Pulse Survey (HPS) to study rates of anxiety and depression in the U.S. adult population for the months of April to December 2020.
SHADAC Director Dr. Lynn Blewett and SHADAC Researchers Colin Planalp and Robert Hest used data from the U.S. Census Bureau’s Household Pulse Survey (HPS) to study rates of anxiety and depression in the U.S. adult population for the months of April to December 2020.
The brief looks at both combined and individual rates of reported anxiety and depression symptoms for the total adult population as well as by specific breakdowns, including age, gender, race/ethnicity, income and education levels, and employment status.
Designed to provide near-real-time estimates of the economic, financial, and health impacts of the pandemic, the HPS asks questions covering topics such as health insurance coverage, medical treatment, employment status, and job loss, food security, and transportation access, among others. The HPS questions used in the analysis of this brief were adapted by the Census Bureau from a four-item screening tool commonly used by health care providers to identify symptoms of anxiety and depression.
Though the United States is beginning to emerge from the darkest days of the pandemic, it is important to remember that this crisis affected not only physical health, but mental health as well, and these burdens must be continued to be monitored and addressed at the local, state, and national levels. This brief provides an overview of mental health impacts on different portions of the populations, and highlights which groups may benefit from particular outreach to connect them with needed mental health care.
Explore Additional COVID-related SHADAC Work Using the HPS
SHADAC previously wrote a blog post that provided an overview of the Household Pulse Survey (HPS) methodology as well as survey and questionnaire updates.
SHADAC has also used HPS data to track vaccination rates for a range of demographic groups, producing our own state-level estimates of vaccination rates for a biweekly blog series.
Additionally, SHADAC produced a blog studying vaccine hesitancy rates among adults during the first part of 2021.
Publication
Escalating Alcohol-Involved Death Rates: Trends and Variation across the Nation and in the States from 2006 to 2019 (Infographics)
April 19, 2021
In the midst of the opioid epidemic, the United States has been quietly experiencing another mounting public health crisis as deaths involving alcohol have grown to historic highs. After years of stability, the rate of alcohol-related deaths began to increase in 2007 and has increased significantly almost every year since, growing by 49 percent to 10.4 deaths per 100,000 people in 2019. Of the 414,000 alcohol-involved deaths that occurred nationwide during the 2006 to 2019 time period, 88,000 would not have occurred if alcohol-involved deaths had held steady at 2006 rates.
 In an effort to shed light on the growing issue of alcohol-involved deaths, SHADAC researchers have produced an issue brief that describes trends and variation in alcohol-involved death rates at the state and national levels, and among demographic subgroups, using vital statistics data from the Centers for Disease Control and Prevention for 2006 to 2019.
In an effort to shed light on the growing issue of alcohol-involved deaths, SHADAC researchers have produced an issue brief that describes trends and variation in alcohol-involved death rates at the state and national levels, and among demographic subgroups, using vital statistics data from the Centers for Disease Control and Prevention for 2006 to 2019.
To accompany the issue brief, SHADAC also developed infographics for all 50 states and the District of Columbia. These infographics present trends in state-level alcohol-involved death rates from 2000-2019, show how each state's 2019 rate compares to the national average, and provide a glimpse into how 2019 alcohol-involved death rates and opioid overdose death rates compare in each state.
State alcohol-involved deaths per 100,000 people, 2019
Click on a state below view its infographic.
Quick infographic links: the United States, the District of Columbia, and All States.
Related Reading:
U.S. Alcohol-Related Deaths Grew Nearly 50% in Two Decades: SHADAC Briefs Examine the Numbers among Subgroups and States (SHADAC Blog)
Overdose Crisis in Transition: Changing National and State Trends in a Widening Drug Death Epidemic (SHADAC Briefs)
50-State Analysis of Drug Overdose Trends: The Evolving Opioid Crisis Across the States (Infographics)
Blog & News
COVID-19 Vaccination Rates: State-level and Subpopulation Analysis of the Household Pulse Survey
April 14, 2021:Update 5: March 17 to March 29
Newly available COVID-19 vaccines promise to help protect individual Americans against infection and eventually provide population-level herd immunity. The pace of COVID-19 vaccination rollout in the United States has picked up after an unsteady start earlier in the year. The country is on track to meet the current administration’s new goal of immunizing 200 million in Biden’s first 100 days in office, despite hiccups in the rollout of the Johnson & Johnson vaccine.
The initial groups prioritized for vaccination were healthcare workers on the front lines of the pandemic and nursing facility residents, many of whom are especially vulnerable to COVID-19 infection and severe outcomes. While these and other high-priority groups continue to be first in line for vaccination slots, many states have since expanded vaccine access to the general adult population. However, there are concerns that these early prioritization decisions and the existing mechanisms of the vaccine rollout—in addition to evidence that lower-income individuals, people of color, and individuals without strong connections to the health care system are less likely to get vaccinated—have created challenges in equitably distributing the COVID-19 vaccine and could worsen existing pandemic-related health inequities.
The available data have not assuaged these concerns and show patterns of lower vaccination rates among people with lower incomes and levels of education and marginalized racial and ethnic groups. The U.S. Census Bureau recently released updated data on take-up of COVID-19 vaccines from the latest wave of its Household Pulse Survey (HPS), collected March 17 - 29, 2021.1 The HPS is an ongoing, weekly tracking survey designed to measure impacts of the COVID-19 pandemic. These data provide an updated snapshot of COVID-19 vaccination rates and are the only data source to do so at the state level by subpopulation.
This blog post presents top-level findings from the new data, focusing on rates of vaccination (one or more doses) among U.S. adults (age 18 and older) living in households and comparing the results to the most recent wave of the HPS, collected March 3 - 15, 2021.2
These data represent the last release from Phase 3 of the HPS. Data collection for Phase 3.1 will begin April 14 after a two-week break to make tweaks to questionnaire content. It is anticipated that the first results from Phase 3.1 will be released on May 5, 2021. Census has indicated that it plans to continue administering the survey through December 2021.
Almost half of U.S. adults had received one or more COVID-19 vaccinations by the end of March.
According to the new HPS data, 47.0% of U.S. adults had received one or more vaccinations by March 29th, though this varied by state from a low of 4.12% in Maryland to a high of 59.6% in Alaska. At least one in two adults had received a vaccine in ten states: Alaska, Connecticut, Hawaii, Nevada, New Mexico, New York, North Dakota, Oklahoma, South Dakota, and West Virginia.
Vaccination rates increased dramatically across nearly all states; states with lower rates catching up
Nationally, adult vaccination rates were up from the previous wave of the HPS, increasing from 34.2% during March 3 - 15, 2021, to 47.0% during March 17 - 29, 2021. Many states experienced a large increase in their vaccination rates. The size of these increases varied from a 5.7 percentage point (PP) increase in Vermont to a 20.0 PP increase in New Mexico. Twelve states saw increases of 15.0 PP or larger.
Percent of Adults Who Had Received a COVID-19 Vaccine
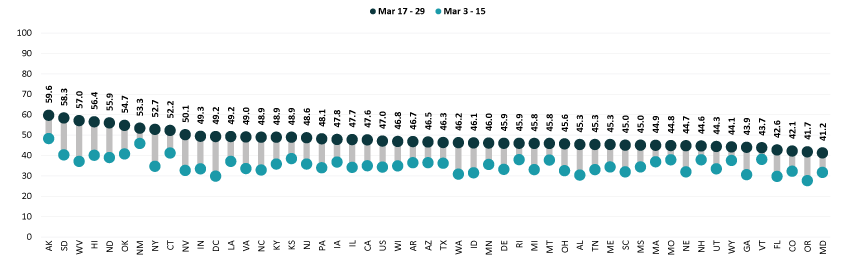
Disparities in vaccination rates improved, but slowly and unevenly
COVID-19 vaccination rates continued to vary to a great degree by demographic and socioeconomic factors. Gaps in vaccination compared to the national average narrowed slightly for most groups, though some groups saw larger improvements. As with prior weeks, vaccination rates were lower for certain subpopulations such as Hispanic/Latino adults, Black adults, and Other/Multiracial adults, and these rates were particularly low for very-low-income adults and for adults without a high school education. More resources, increased attention, or new strategies may be needed to close the gaps for the hardest-to-reach groups.
By race and ethnicity, Asian and white adults continued to have above-average vaccination rates at 51.4% and 50.1%, respectively. Rates among Black adults (42.0%), adults identifying with “Multiple” or “Some Other” race (40.0%), and Hispanic/Latino adults (37.7%) continued to be below the national average. However, vaccination rates among Black adults, “Multiple” or “Some Other” race adults, and Hispanic/Latino adults all improved somewhat relative to the national average.
Hispanic/Latino adults had the largest relative improvement, going from 26 percent below the national average in the first half of March (25.4% vs. 34.2%) to 20 percent below the national average in the second half of March (37.7% vs. 47.0%). This was a marked improvement after consistently being 25 to 30 percent below the national average with every bi-weekly release since the beginning of January.
Percent of Adults Who Had Received a COVID-19 Vaccine by Race/Ethnicity
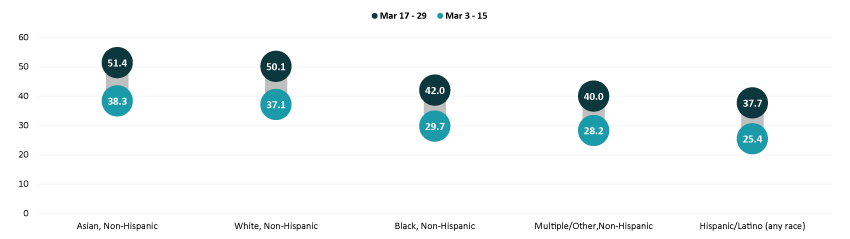
Gaps in vaccination rates among income levels have continued to narrow, however, Adults with household incomes below $50,000 are still falling below the national average, whereas adults with household incomes above $50,000 remain higher than the national average. Vaccination rates among adults with incomes less than $35,000 continued to improve compared to the national average. This improvement was especially large among adults with incomes between $25,000 and $34,999, going from 22 percent below the national average in the first half of March (26.7% vs. 34.2%) to just 6 percent below the national average in the second half of March (46.6% vs. 47.0%).
Percent of Adults Who Had Received a COVID-19 Vaccine by Income
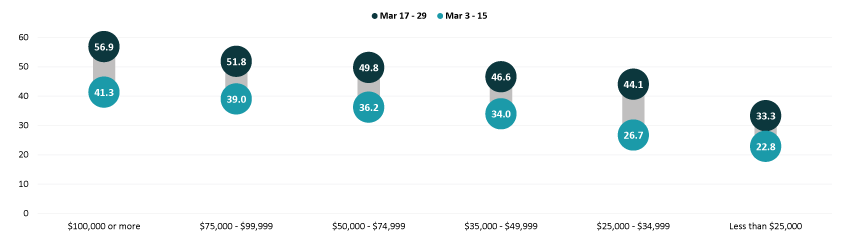
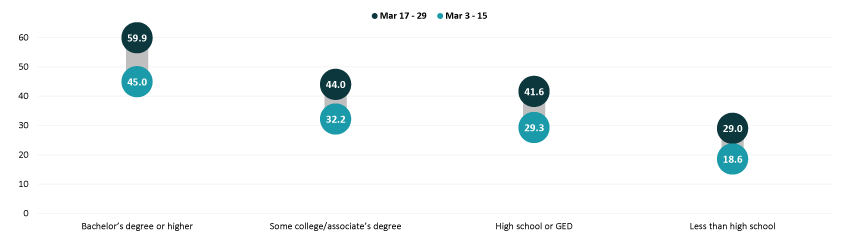
Disparities by level of education remained, with adults that hold a bachelor’s degree or higher continuing to have the highest vaccination rate at 59.9% and adults without a high school diploma having the lowest vaccination rates at 29.0%. Disparities by education did narrow somewhat relative to the national average, especially for adults with a high school education or equivalent and adults with less than a high school level of education. However, adults with less than a high school level of education continued to have the lowest rates of vaccination of any of the groups analyzed here.
Percent of Adults Who Had Received a COVID-19 Vaccine by Education
Nationally, More than four in five older adults had received a COVID-19 vaccine
Nationally, 80.1% of older adults (age 65 and older) had received at least one dose of the COVID-19 vaccine, which was 33.1 PP higher than the rate among all adults (47.0%). Vaccination rates for older adults ranged from a low of 67.4% in Hawaii to a high of 90.1% in Connecticut. Hawaii was the only state to have a 65+ vaccination rate of below 70 percent.
As may be expected given the high rates of vaccination in the older adult population, rates of increase in vaccination in this group slowed somewhat in the last half of March. No state increased its 65+ vaccination rate by more than 0.43x (Oregon), whereas ten states were able to increase vaccination rates by 0.5x or more in the first half of the month. Though the 65+ vaccination rates in Alaska appeared to have fallen in the second half of March, this was more than likely a statistical artifact rather than an actual decrease.
Percent of Adults Age 65+ Who Had Received a COVID-19 Vaccine

Notes about the Household Pulse Survey Data
The estimated rates presented in this post were calculated from the count estimates published by the Census Bureau. Though these counts are accompanied by standard errors, standard errors are not able to be accurately calculated for rate estimates. Therefore, we are not able to determine if the differences we found in our analysis are statistically significant or if the estimates themselves are statistically reliable. Estimates and differences for subpopulations at the state level should be assumed to have large confidence intervals around them and caution should be taken when drawing strong conclusions from this analysis. However, the fact that these early indications of COVID-19 inequities mirror patterns of other vaccinations inequities demonstrate reason for concern.
Though produced by the U.S. Census Bureau, the HPS is considered an “experimental” survey and does not necessarily meet the Census’ high standards for data quality and statistical reliability. For example, the survey has relatively low response rates (7.2% for March 17 - 29), and sampled individuals are contacted via email and text message, asking them to complete an internet-based survey. These issues in particular could be potential sources of bias but come with the tradeoffs of increased speed and flexibility in data collection as well as lower costs. A future post will investigate differences between COVID-19 vaccination rates estimated from survey data (such as the HPS) and administrative sources. The estimates presented in this post are based on responses from 77,104 adults. More information about the data and methods for the Household Pulse Survey can be found in a previous SHADAC blog post.
Previous Blogs in this Series
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey (Update 4: 3/3 - 3/15) (SHADAC Blog)
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey (Update 3: 2/17 - 3/1) (SHADAC Blog)
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey (Update 2: 2/3 - 2/15) (SHADAC Blog)
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey (Update: 1/10 - 2/1) (SHADAC Blog)
COVID-19 Vaccination Rates: New State-level and Subpopulation Evidence from the Household Pulse Survey (1/6 - 1/18) (SHADAC Blog)
Related Reading
State-level Flu Vaccination Rates among Key Population Subgroups (50-state profiles) (SHADAC Infographics)
50-State Infographics: A State-level Look at Flu Vaccination Rates among Key Population Subgroups (SHADAC Blog)
Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (SHADAC Brief)
New Brief Examines Flu Vaccine Patterns as a Proxy for COVID – Anticipating and Addressing Coronavirus Vaccination Campaign Challenges at the National and State Level (SHADAC Blog)
Ensuring Equity: State Strategies for Monitoring COVID-19 Vaccination Rates by Race and Other Priority Populations (Expert Perspective for State Health & Value Strategies)
SHADAC Webinar - Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (February 4th) (SHADAC Webinar)












