Blog & News
Spotlight on Health Behaviors: Adult Who Forgo Needed Medical Care and Adults Who Have No Personal Doctor
December 21, 2020:Prior to the arrival of the novel coronavirus, much of American consumer health care concerns surrounded rising costs of care. With health care spending rising a reported 4.6 percent in 2018 and the Centers for Medicare and Medicaid Services (CMS) Office of the Actuary projecting an average annual increase of 5.4 percent for 2019 to hit a record $3.82 trillion or around $11,559 per person—this issue will remain at the forefront of concern for the foreseeable future.1
Compounding these trends in spending, the continued rise in the share of Americans without health insurance coverage has left more individuals without a means of protecting themselves or their families from the financial burden of illness or injury and without strong ties to health care providers and the health care system to access care.
The effects of rising health care spending and rising rates of uninsurance can be seen in direct measures of actual dollars, such as Medical Out-of-Pocket Spending and Percent of Individuals with High Medical Care Cost Burden, but also in more indirect avenues, such as changes in health behaviors and access to care.
Two measures of such behaviors, Adults Who Forgo Needed Medical Care and Adults with No Personal Doctor, are housed on SHADAC’s State Health Compare and have been recently updated with 2019 data from the Center for Disease Control's Behavioral Risk Factor Surveillance System (BRFSS). This blog provides an analysis of these indirect costs of rising health care spending and uninsurance in the year prior to the COVID-19 pandemic and examines overall national and state-level trends as well as comparisons across race/ethnicity and educational attainment.
Adults Who Forgo Needed Care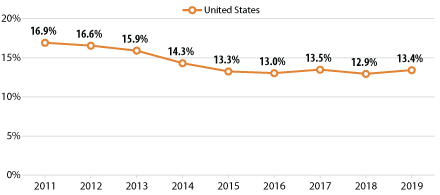
Across the nation, progress was made in reducing the percentage of adults who forgo needed medical care in the years following the passage of the Affordable Care Act (ACA). However, that progress began to flatten out by 2016 and has now begun to reverse course and display a trend of smaller but significant increases in recent years, such as the growth from 12.9% in 2018 to 13.4% in 2019 at the national level.
Trends by Education and Race/Ethnicity
Examining forgone care by individual breakdowns showed that disparities by education level and race/ethnicity, found in a previous SHADAC analysis, have persisted from the year before.
Across the U.S., adults with less than a high school degree saw their rates of forgone care hit 22.2% in 2019 from 21.1% in 2018;i a figure nearly triple the rate among adults with a bachelor’s degree, who saw their rate of forgone care rise to 7.9% in 2019 (up from 7.4% in 2018).
Nationally, Hispanic/Latino adults experienced the largest increase in rates of forgone care, rising to 21.4% in 2019 from 20.2% in 2018. African-American/Black and Hispanic/Latino adults were also significantly more likely to report going without needed medical care than White adults, with the former being 1.5 times more likely (15.7% vs. 10.9%) and the latter nearly twice as likely (21.4% vs. 10.9%).
State Trends
At the state level, the trends in forgone care are varied. Despite increasing national trends, some states, such as Florida and Michigan, have continued to make steady progress in reducing forgone care. Florida saw their overall rates drop by 5.9 percentage points,ii from 22.0% in 2011 to 16.0% in 2019, and Michigan saw a similarly steady drop in rates of forgone care from 16.5% in 2011 to 11.7% in 2019.
Unfortunately, progress in reducing the number of adults who report going without needed medical care has stalled in many states—California and Kentucky being two such examples. The former state has seen relatively unchanged rates of forgone care since 2016 (11.4%, 11.8% in 2017, and 11.9% in 2018 and 2019). The percentage of adults who have gone without needed medical care in Kentucky has likewise remained nearly unchanged from 2015 to 2019 (12.3% and 12.1%, respectively).
In other states, such as Kansas and Maine, rates of forgone care have followed the national trend and in 2015 begun reversing course on previous gains. The state of Kansas saw a 2.1 percentage-point increase from 2015 to 2019 (11.0% to 13.1%) and Maine saw a concerning increase of 2.9 percentage points during the same time period (9.4% in 2015 to 12.3% in 2019).
It is important to remember that these increases in forgone care occurred in the context of an economy that was growing steadily before the COVID recession. Though the release of 2020 data is at least another year away, early studies and surveys have given some indications as to the impact of the COVID-19 pandemic on health behaviors. SHADAC conducted a survey in April 2020 in which over half of U.S. adults (51.1 percent) said they had delayed or canceled health care appointments due to the pandemic.2
Adults With No Personal Doctor
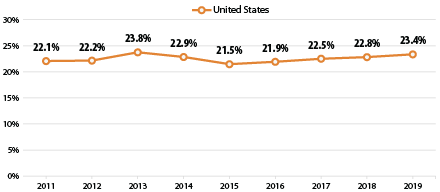 As with the measure of forgone medical care, more adults reported having a usual source of care after the passage of the ACA. However, once again this promising trend reversed itself in 2015, after which the percent of adults with no personal doctor or health care provider has increased each year, nearly reaching its pre-ACA peak in 2019 at 23.4% (23.8% in 2013). Both of these increasing trends have paralleled an increase in the rate of the uninsured across the nation, from 8.6% in 2016 to 9.2% in 2019.3
As with the measure of forgone medical care, more adults reported having a usual source of care after the passage of the ACA. However, once again this promising trend reversed itself in 2015, after which the percent of adults with no personal doctor or health care provider has increased each year, nearly reaching its pre-ACA peak in 2019 at 23.4% (23.8% in 2013). Both of these increasing trends have paralleled an increase in the rate of the uninsured across the nation, from 8.6% in 2016 to 9.2% in 2019.3
Trends by Education and Race/Ethnicity
Significant disparities by education level and race/ethnicity were again present for this measure in 2019.
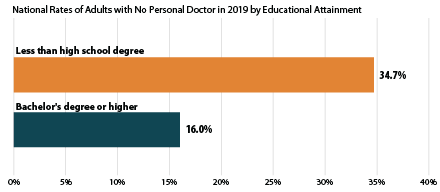 At the national level, adults with less than a high school education were more than twice as likely as adults with a bachelor’s degree to report not having a regular doctor (34.7% versus 16.0%). This pattern was consistent across more than half of states, as adults with less than a high school degree were more than twice as likely to report having no doctor as those with a bachelor’s degree in 26 states, and more than three times as likely in 5 states (Connecticut, Delaware, Maryland, Nebraska, and New Hampshire). There was no statistical difference between these educational groups in D.C. and 6 states (Kentucky, Mississippi, North Dakota, Tennessee, Vermont and West Virginia).
At the national level, adults with less than a high school education were more than twice as likely as adults with a bachelor’s degree to report not having a regular doctor (34.7% versus 16.0%). This pattern was consistent across more than half of states, as adults with less than a high school degree were more than twice as likely to report having no doctor as those with a bachelor’s degree in 26 states, and more than three times as likely in 5 states (Connecticut, Delaware, Maryland, Nebraska, and New Hampshire). There was no statistical difference between these educational groups in D.C. and 6 states (Kentucky, Mississippi, North Dakota, Tennessee, Vermont and West Virginia).
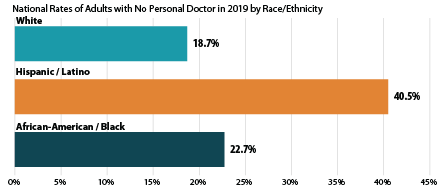 Nationally, Hispanic/Latino and Black adults were both significantly more likely to report not having a regular doctor as compared to White adults. Hispanic/Latino adults were more than twice as likely as White adults to report not having a personal doctor (40.5% vs. 18.7%), and African-American/Black adults were more than 1.2 times as likely as White adults to report not having a personal doctor (22.7% vs. 18.7%). Again this pattern persisted among over half of the nation, as Hispanic/Latino adults were more than twice as likely to report not having a regular doctor as White adults in 28 states, and more than three times as likely to report the same in 3 states (Delaware, Maryland, and Nebraska). African-American/Black adults were at least 1.2 times as likely to report not having a regular doctor as White adults in 17 states, and this gap measured 1.5 times or larger in 6 states (Nebraska, Iowa, Kansas, Massachusetts, Michigan and Utah).
Nationally, Hispanic/Latino and Black adults were both significantly more likely to report not having a regular doctor as compared to White adults. Hispanic/Latino adults were more than twice as likely as White adults to report not having a personal doctor (40.5% vs. 18.7%), and African-American/Black adults were more than 1.2 times as likely as White adults to report not having a personal doctor (22.7% vs. 18.7%). Again this pattern persisted among over half of the nation, as Hispanic/Latino adults were more than twice as likely to report not having a regular doctor as White adults in 28 states, and more than three times as likely to report the same in 3 states (Delaware, Maryland, and Nebraska). African-American/Black adults were at least 1.2 times as likely to report not having a regular doctor as White adults in 17 states, and this gap measured 1.5 times or larger in 6 states (Nebraska, Iowa, Kansas, Massachusetts, Michigan and Utah).
Related Reading
Affordability and Access to Care in 2018: Examining Racial and Educational Inequities across the United States (Infographic)
Most U.S. Adults Report Reduced Access to Health Care due to Coronavirus Pandemic
Eleven Updated Measures are Now Available on State Health Compare
1 Hartman, M., Martin, A.B., Benson, J., & Catlin, A. (2019, December 5). National Health Care Spending in 2018: Growth Driven by Accelerations in Medicare and Private Insurance Spending. HealthAffairs, 39(1). https://doi.org/10.1377/hlthaff.2019.01451
Keehan, S.P., Cuckler, G.A., Poisal, J.A., Sisko, A.M., Smith, S.D., Madison, A.J., Rennie, K.E., Fiore, J.A., & Hardesty, J.C. (2020, March 24). National Health Expenditure Projections, 2019–28: Expected Rebound in Prices Drives Rising Spending Growth. HealthAffairs, 39(4). https://doi.org/10.1377/hlthaff.2020.00094
California Health Care Foundation (CHCF). (2019). Health Care Costs 101: Spending Keeps Growing. California Health Care Almanac. https://www.chcf.org/wp-content/uploads/2019/05/HealthCareCostsAlmanac2019.pdf
2 Planalp, C., Alarcon, G., & Blewett, L.A. (2020). Coronavirus pandemic caused more than 10 million U.S. adults to lose health insurance. https://shadac.org/news/SHADAC_COVID19_AmeriSpeak-Survey
3 State Health Access Data Assistance Center (SHADAC). (2020). 2019 ACS: Rising National Uninsured Rate Echoed Across 19 States; Virginia Only State to See Decrease (Infographics). https://www.shadac.org/sites/default/files/ACS_Estimates-2019-Infographic.pdf
Blog & News
State Health Compare Users Can Now Explore Unemployment by Race/Ethnicity
November 18th, 2020:SHADAC has updated our State Health Compare online data tool to provide estimates of unemployment according to race and ethnicity. Previously, State Health Compare users could analyze unemployment nationwide and at the state level for years 2000 to 2019, but subgroup analyses were not possible. Now, users can explore State Health Compare’s unemployment estimates, which come from the federal Bureau of Labor Statistics, by four racial/ethnic breakdowns: Hispanic/Latino, African-American/Black, Asian and White.
Why This Change Matters
Racial/ethnic breakdowns provide an important lens for analyzing unemployment as a social determinant of health, with unemployment often varying widely across racial/ethnic categories in a way that can be masked by a consideration of population-wide unemployment numbers. We see this scenario at the national level, where the overall unemployment rate in 2019 was 3.7%, but an examination of unemployment for racial/ethnic subgroups reveals 2.7% unemployment among Asian Americans, 3.3% unemployment among Whites, 4.3% unemployment among Hispanics/Latinos, and 6.1% unemployment among African-Americans/Blacks.
Minnesota provides a state case that parallels the national picture on this point. If we look at statewide unemployment in 2019, we find that Minnesota’s unemployment rate was 3.2%, which is 0.5 percentage points below the national rate of 3.7%. However, if we look at the numbers sorted by race/ethnicity, a different picture emerges: The rate for Asians in Minnesota is 2.4%, Whites are at 3.0%, Hispanics/Latinos are at 5.0%, and African-Americans/Blacks are at 5.5%. Not only do Hispanics/Latinos and African-Americans/Blacks have higher unemployment rates than Whites and Hispanics/Latinos, but their rates are also above the broader Minnesota state average, as well as the national average. Thus, what looks at first glance like a state doing well on unemployment turns out to be a state with major disparities in unemployment for certain racial/ethnic subgroups.
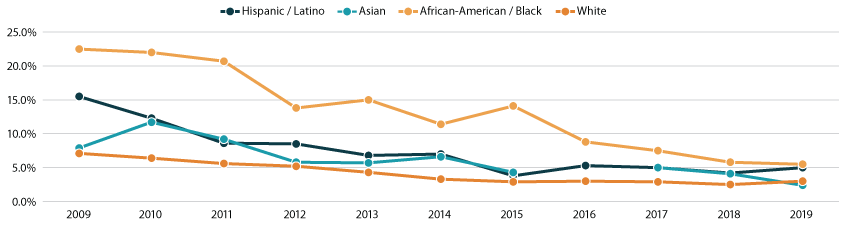
An examination of trends in unemployment over time confirms that the 2019 data for Minnesota are not an anomaly. Though unemployment numbers for Asians in Minnesota were less stable from year to year, White Minnesotans consistently had unemployment rates below those of Hispanic/Latino Minnesotans each year during the 10-year period from 2009 to 2019, and African-American and Black Minnesotans consistently had the highest unemployment rates of any analyzed racial/ethnic group during this time (Figure 1.)
Figure 1. Unemployment in Minnesota by Race/Ethnicity, 2009-2019
The Importance of Considering Individual States
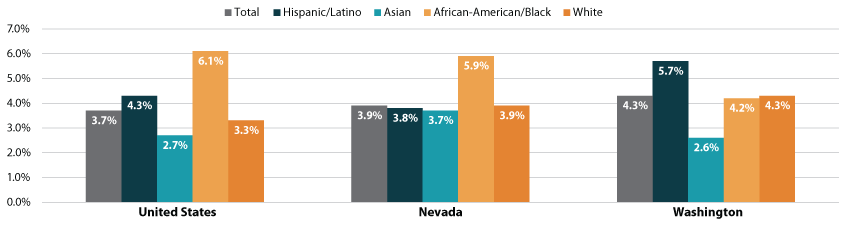
Additionally, it is worth exploring both overall and racial/ethnic subgroup numbers within each individual state, as there is considerable variation both across states and between states and the nation. Washington state, for example, saw an overall unemployment rate of 4.3%, or 0.6 percentage points above the national rate. And among racial/ethnic subgroups, Washington’s numbers followed a different pattern than that seen nationally, with African-Americans/Blacks having the second lowest unemployment rate (4.2%), Whites having the third lowest rate (4.3%), and Hispanics/Latinos having the highest rate (5.7%).
Nevada is another state that had 2019 unemployment numbers that differed from the national story when looking at racial/ethnic breakdowns. Like Washington, Nevada’s state’s overall unemployment rate of 3.9% was above the national rate. However, unemployment in Nevada was second lowest among Hispanics/Latinos (3.8%), third lowest among Whites (3.9%), and highest among African-Americans/Blacks (5.9%).
Figure 2. Unemployment in by Race/Ethnicity, 2019: United States, Nevada, Washington
Taking these state variations into consideration, it’s clear that efforts to analyze and/or address disparities in unemployment by race/ethnicity would potentially look different in Washington and Nevada, or even going to back our example in Minnesota, based on their respective divergences in overall and subgroup numbers.
Discussion: Unemployment as a Social Determinant of Health
Unemployment has important implications for health and health care, as employment affects access to stable housing, food, and health insurance coverage and care. At the same time, unemployment can also have a number of direct negative health consequences, including depression, anxiety, and stress-related illness such as high blood pressure, stroke, heart attack, heart disease, and arthritis.1-7
An examination of unemployment that takes into consideration important nuances in unemployment numbers among subgroups reveals the need for critical, targeted attention to unemployment, even in states where unemployment appears to be trending well overall. Consideration of interstate variation of unemployment by race/ethnicity reveals that policy levers to address unemployment that take race/ethnicity into consideration will require state-specific modifications as well.
Explore the Data
Visit State Health Compare to learn more about unemployment by race/ethnicity within and across the states.
About the Estimates
State Health Compare’s estimates of unemployment are produced using data from the federal Bureau of Labor Statistics and represent the percent of the civilian labor force (age 16 and older) that was unemployed. State refers to place of residence.
1 Avendano, M., Berkman, L. F. (2014). Labor markets, employment policies, and health. In L. F. Berkman, I. Kawachi, & M. Glymour (Eds.), Social Epidemiology (2nd ed., pp. 182-233). Open University Press.
2 Murray, L. R. (2003). Sick and tired of being sick and tired: scientific evidence, methods, and research implications for racial and ethnic disparities in occupational health. Am J Public Health, 93(2), 221-226.
3 Kasl, S. V., Cobb, S. (1970). Blood pressure changes in men undergoing job loss: a preliminary report. Psychosom Med, 32(1), 19-38.
4 Frumkin, H. E., Walker, D., Friedman-Jiménez, G. (1999). Minority workers and communities. Occup Med, 14(3), 495-517.
5 James, S. A., LaCroix, A. Z., Kleinbau, D. G., Strogatz, D. S. (1984). John Henryism and blood pressure differences among black men. II. The role of occupational stressors. J Behav Med, 7(3), 259-275.
6 Robert Wood Johnson Foundation. (2013). How does employment—or unemployment—affect health? Health policy snapshot. Available from http://www.rwjf.org/content/dam/farm/reports/issue_briefs/2013/rwjf403360
7 U.S. Department of Labor, Bureau of Labor Statistics. (2012). A profile of the working poor, 2010. News release. Available from https://www.bls.gov/opub/reports/working-poor/archive/workingpoor_2010.pdf
Blog & News
November 10th Webinar - "Overdose Crisis in Transition: Changing Trends in a Widening Drug Death Epidemic"
November 24, 2020:Mr. Planalp was joined by SHADAC Research Fellow Robert Hest, who explained how to access and use the data on opioid-related overdose deaths and sales of opioid painkillers through SHADAC’s State Health Compare website. Slides from the presentation, as well as a list of further SHADAC resources regarding the opioid crisis can be found at the bottom of this page.
Speakers
 Colin Planalp, MPA
Colin Planalp, MPA
SHADAC Senior Research Fellow
 Robert Hest, MPP
Robert Hest, MPP
SHADAC Research Fellow
Event Resources
The Opioid Epidemic (SHADAC Resource Page)
Overdose Crisis in Transition: Changing National and State Trends in a Widening Drug Death Epidemic (Briefs)
50-State Analysis of Drug Overdose Trends: The Evolving Opioid Crisis Across the States (Infographics)
After drop in 2018, newer data indicate a resurgence in drug overdose deaths
Blog & News
October 21st Webinar - Rising Suicide Rates: Examining Trends and Variations through State-level Data
October 26, 2020:Over the past two decades, the rise in suicide death rates has continued along an accelerating climb. According to new vital statistics data from the Centers for Disease Control and Prevention (CDC), the United States suicide rate reached another historic high of 14.2 per 100,000 people in 2018, up from 14.0 in the previous year.
This increase in suicide deaths has not followed a consistent trend; rather, growth has accelerated more recently. From 2000 to 2009 the suicide death rate grew by 13 percent, but from 2009 to 2018 the rate grew by 21 percent. While these trends predate the COVID-19 pandemic, early evidence has indicated this crisis is taking a significant toll on mental health, and these data therefore represent an important baseline from which the effects of the pandemic will be measured.
During the webinar, SHADAC Research Fellow Carrie Au-Yeung used national and state-level data on suicide deaths to examine this growing public health issue, highlighting concerning trends and variations in suicide deaths by geographic locations such as regions, states, and metropolitan areas, as well as by specific subpopulation groups such as age, sex, and race/ethnicity.
Ms. Au-Yeung was also joined by SHADAC Research Fellow Robert Hest, who explained how to access and use the data on suicide deaths through SHADAC’s State Health Compare website. Senior Research Fellow Colin Planalp also joined the webinar for a question and discussion session following the presentation.
 Related Resources
Related Resources
Suicide Rates on the Rise: Examining Continuing Trends and Variation across the Nation and in the States from 2000 to 2018 (Briefs)
U.S. Suicide Death Rate Reached Record High in 2018: SHADAC Briefs Examine the Numbers among Subgroups and States
State Health Compare Data Offer Baseline for Measuring Pandemic's Impact on Suicide, Drug Overdose Death Rates
National Suicide Prevention Lifeline: 1-800-273-8255
If you’re thinking about suicide, are worried about a friend or loved one, or would like emotional support, the Lifeline network is available 24/7 across the United States. For more suicide prevention resources, visit https://suicidepreventionlifeline.org/
Blog & News
Eleven Updated Measures are Now Available on State Health Compare
October 5, 2020:Estimates for a majority of measures from several categories (Access to Care, Cost of Care, Health Behaviors, and Health Outcomes) have now been updated on SHADAC’s State Health Compare web tool, from two related surveys conducted by the Centers for Disease Control and Prevention—the Youth Risk Behavior Surveillance System (YRBSS), which surveys U.S. middle and high school students (age 13-17), and the Behavior Risk Factor Surveillance System (BRFSS), which surveys U.S. adults (age 18+).
Measures that have been updated from the YRBSS include:
High School Obesity
 This measure indicates the percent of high school students (grades 9-12) in each state who were considered obese (i.e., > 95th percentile for body mass index, based on sex- and age-specific reference data from 2000 CDC growth charts).
This measure indicates the percent of high school students (grades 9-12) in each state who were considered obese (i.e., > 95th percentile for body mass index, based on sex- and age-specific reference data from 2000 CDC growth charts).
Estimates are available for all states from 2001 through 2019.
High School Smoking
Estimates for this measure denote the percent of high school students (grades 9-12) in each state who have smoked at least one cigarette in the past 30 days; data are available from 2001 through 2019.
High School Physical Activity
This measure provides estimates of the percentage of high school students (grades 9-12) who did engage in the recommended guideline of at least 60 minutes of activity each day, in the previous five days. Data are available for all states from 2011 through 2019.
Measures that have been updated from the BRFSS include:
Adults Who Forgo Needed Medical Care*
The measure indicates the percent of adults (18+) in each state who could not get needed medical care due to cost. Breakdowns by education level and race/ethnicity are available for all states from 2005 through 2010 and 2011 through 2019.
Adults With No Personal Doctor*
This measure presents the percent of adults without a personal doctor and is now available for all states from 2005 through 2010 and 2011 through 2019. Breakdowns by education level and race/ethnicity are also available.
Chronic Disease Prevalence*
Data for this measure captures the percent of adults who reported having one or more common chronic conditions such as diabetes, cardiovascular disease, heart attack, stroke, and asthma, in each state. Estimates are now available for all states from 2005 through 2010 and 2011 through 2019.
Adult Unhealthy Days
There are a multitude of options for this measure, which shows the average number of days when an adult's physical health or mental health was not good during the past 30 days. Users can view estimates solely by reported mentally unhealthy days, physically unhealthy days, or a composite of both—though the combination of both physical and mental unhealthy days is capped at a total of 30 days. Estimates for each version of this measure are available for 2011 to 2019 and possible breakdowns include age, health insurance coverage, household income categories, disability status, education levels, and race/ethnicity.
Activities Limited due to Health Difficulty*
This measure reports the average number of days (in the last 30 days) for which an adult indicated their activity were limited stemming from either mental or physical health difficulties, and data is available for all states from 2005 through 2010 and 2011 through 2019.
Adult Obesity*
The measure is an indication of the prevalence of obesity (defined for adults as a Body Mass Index [BMI] > 30) among the U.S. population 18 years of age and over. It is now available for all states from 2005 through 2010 and 2011 through 2019.
Adult Binge Drinking*
This measure indicates the percent of adults who have consumed at least four drinks (women) or five (men) or more on one occasion during the past 30 days. Now available for all states from 2005 through 2010 and 2011 through 2019, the measure includes breakdowns by education level and race/ethnicity.
Adult Smoking*
This measure indicates the percent of adults over 18 years of age who have smoked 100 or more cigarettes in their lifetime, and who currently smoke at least some days or every day. Estimates are available for all states from 2005 through 2010, and 2011 through 2019, with breakdowns by education level and race/ethnicity.
Notes
All measures marked with an “*”: This indicates a break in series due to the BRFSS implementing cell phone sampling and an advanced weighting method in 2011.
Click here to explore these updated estimates on State Health Compare!