Blog & News
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey - Update 4
March 25, 2021:Update 4: March 3 to March 15
Newly available COVID-19 vaccines promise to help protect individual Americans against infection and eventually provide population-level herd immunity. The pace of COVID-19 vaccination rollout in the United States has picked up after an unsteady rollout earlier in the year. The country has met the current administration’s goal of administering 100 million COVID-19 vaccines sooner than expected, and further increases in supply are on the horizon as newly authorized Johnson & Johnson vaccines are anticipated to be available in the coming weeks.
The initial groups prioritized for vaccination were health care workers on the front lines of the pandemic and nursing facility residents, many of whom are especially vulnerable to COVID-19 infection and severe outcomes. While these groups continue to hold priority in vaccination slots, many states have since expanded vaccine access to other (still high-priority) segments of the general population. Additionally, a growing number of states have now expanded eligibility to all adults. However, there are concerns that these prioritization decisions and the existing mechanisms of the vaccine rollout—in addition to evidence that lower-income individuals, people of color, and individuals without strong connections to the health care system are less likely to get vaccinated—are inadequate to narrow the clear disparities in the distribution of the COVID-19 vaccine and could worsen existing pandemic-related health inequities.
The available data have not assuaged these concerns, and show patterns of lower vaccination rates among people with lower incomes and levels of education, and marginalized racial and ethnic groups. The U.S. Census Bureau recently released updated data on take-up of COVID-19 vaccines from the most recent wave of its Household Pulse Survey (HPS), collected March 3 - 15, 2021.1 The HPS is an ongoing, weekly tracking survey designed to measure the impacts of the COVID-19 pandemic. These data provide an updated snapshot of COVID-19 vaccination rates and are the only data source to do so at the state level by subpopulation.
This blog presents top-level findings from these new data, focusing on rates of vaccination (one or more doses) among U.S. adults (age 18 and older) living in households and how these findings compare to results from the most recent wave of the HPS, collected February 17 - March 1, 2021.2
The current phase of the HPS is slated to continue data collection through the end of March 2021, after which time the survey may be out of the field while changes are made to questionnaire content before returning in April. Census has indicated that it plans to continue administering the survey through December 2021.
Nationally, more than one in three adults received a vaccination, but this varied by state
According to the new HPS data, 34.2% of U.S. adults had received one or more COVID-19 vaccinations by the end of the second week in March, though this varied by state from a low of 27.6% in Oregon to a high of 48.2% in Alaska. At least four in ten adults had received a vaccine in six states: Alaska, Connecticut, Hawaii, Oklahoma, and South Dakota.
Vaccination rates increased substantially across nearly all states; states with lower rates catching up
Nationally, adult vaccination rates were up from the previous wave of the HPS, increasing from 25.5% during February 17–March 1, 2021, to 34.2% during March 3–15, 2021. Every state experienced an increase in their vaccination rates, though the size of these increases varied from a 3.5 percentage point (PP) change in the District of Columbia to a 15.0 PP in New Mexico.
Percent of Adults Who Had Received a COVID-19 Vaccine
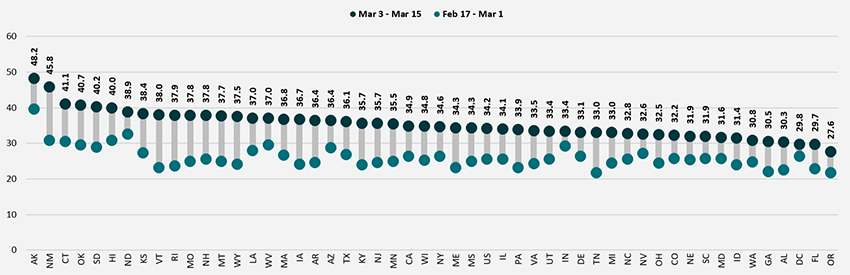
Disparities in vaccination rates improved, but slowly and unevenly
COVID-19 vaccination rates continued to vary to a great degree by demographic and socioeconomic factors. Gaps between most groups and the national average were largely unchanged from previous weeks, though some groups did see improvements. As with prior weeks, vaccination rates were lower for certain subpopulations such as Hispanic/Latino adults, Black adults, and Other/Multiracial adults, low-income adults, and for adults without a high school education. More resources and attention may be needed to close the gaps for the hardest-to-reach groups.
By race and ethnicity, Asian and White adults continued to have above-average vaccination rates at 38.3% and 37.1%, respectively. Rates among Black adults (29.7%), adults identifying with “Multiple” or “Some Other” race (28.2%), and Hispanic/Latino adults (25.4%) continued to be below the national average. However, vaccination rates among Black adults did improve somewhat relative to the national average, going from 21 percent below the national average (20.2% vs. 25.5%) in the second half of February to 13 percent below the national average (29.7% vs. 34.2%) in the first half of March.
Percent of Adults Who Had Received a COVID-19 Vaccine by Race/Ethnicity
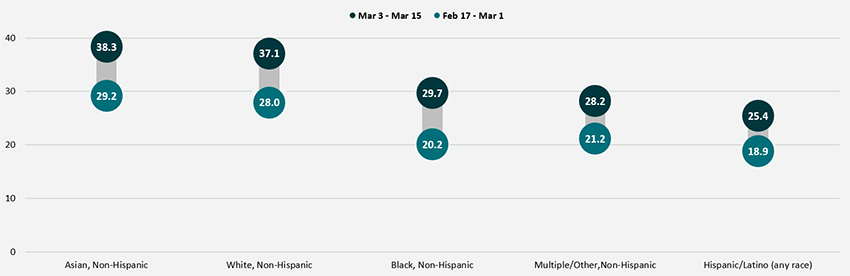
Disparities in vaccination rates by income continued to narrow, though progress was very slow and uneven across income groups. Adults with household incomes below $50,000 continued to have vaccination rates below the national average, whereas adults with household incomes above $50,000 had vaccination rates higher than the national average. However, the size of the gaps between the highest income and lowest income groups narrowed somewhat. Whereas in the second half of February adults with household incomes of $100,000 or higher had vaccination rates nearly 2.0x those of adults with incomes less than $25,000, that gap had narrowed slightly to 1.8x in the first half of March.
Percent of Adults Who Had Received a COVID-19 Vaccine by Income
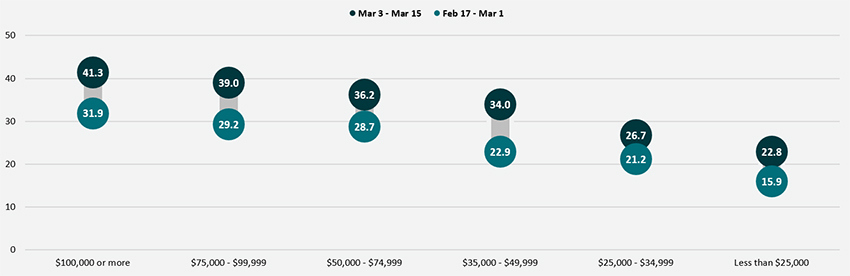
Disparities by level of education remained, with adults holding a bachelor’s degree or higher continuing to have the highest vaccination rate at 45.0%, and adults without a high school diploma having the lowest vaccination rates at 18.6%. Though adults with some college or an associate’s degree and adults with a high school degree or equivalent saw solid growth in their vaccination rates, almost no progress was made among adults without a high school diploma or equivalent. The gap between that group and the national average widened in the first half of March to 46 percent below the national average (18.6% vs. 34.2%) from 32 percent below the national average (17.2% vs. 25.5%) in the second half of February.
Percent of Adults Who Had Received a COVID-19 Vaccine by Education
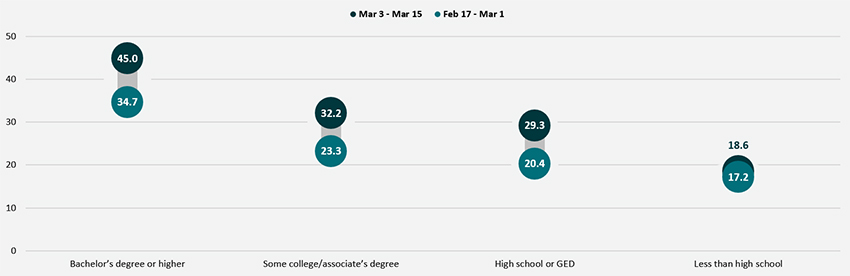
Nationally, More than two-thirds of older adults received a COVID-19 vaccine and many states continued to make considerable progress in vaccinating older adults
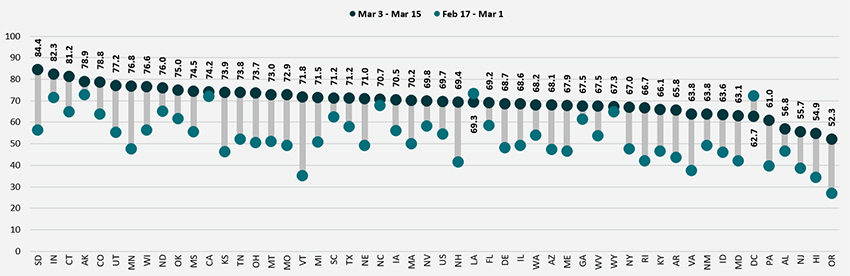
Nationally, 69.7% of older adults (age 65 and older) had received at least one dose of the COVID-19 vaccine, which was 35.5 percentage points higher than the rate among all adults (34.2%). Vaccination rates for older adults ranged from a low of 52.3% in Oregon to a high of 84.4% in South Dakota. Older adult vaccination rates were below 60% in just four states (Alabama, Hawaii, New Jersey and Oregon) and at or above 75% in ten states (Alaska, Colorado, Connecticut, Indiana, Minnesota, North Dakota, Oklahoma, South Dakota, Utah and Wisconsin).
As in the previous period, states continued to make good progress in increasing rates of vaccinations among older adults. Compared to the second half of February, 10 states increased their age 65+ vaccination rates by at least 0.5x, with Vermont more than doubling its vaccination rate for adults age 65+. Only a handful of states failed to make substantial progress in increasing vaccination rates among older adults. Though the 65+ vaccination rates in Louisiana and the District of Columbia appeared to have fallen in the first half of March, this was more than likely a statistical artifact rather than an actual decrease.
Percent of Adults Age 65+ Who Had Received a COVID-19 Vaccine
Notes about the Household Pulse Survey Data
The estimated rates presented in this post were calculated from the count estimates published by the Census Bureau. Though these counts are accompanied by standard errors, standard errors are not able to be accurately calculated for rate estimates. Therefore, we are not able to determine if the differences we found in our analysis are statistically significant or if the estimates themselves are statistically reliable. Estimates and differences for subpopulations at the state level should be assumed to have large confidence intervals around them and caution should be taken when drawing strong conclusions from this analysis. However, the fact that these early indications of COVID-19 inequities mirror patterns of other vaccinations inequities demonstrate reason for concern.
Though produced by the U.S. Census Bureau, the HPS is considered an “experimental” survey and does not necessarily meet the Census’s high standards for data quality and statistical reliability. For example, the survey has relatively low response rates (7.4% for March 3 - 15), and sampled individuals are contacted via email and text message, asking them to complete an internet-based survey. These issues in particular could be potential sources of bias but come with the tradeoffs of increased speed and flexibility in data collection as well as lower costs. A future post will investigate differences between COVID-19 vaccination rates estimated from survey data (such as the HPS) and administrative sources. The estimates presented in this post are based on responses from 78,306 adults. More information about the data and methods for the Household Pulse Survey can be found in a previous SHADAC blog post.
Previous Blogs in this Series
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey (Update 3: 2/17 - 3/1) (SHADAC Blog)
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey (Update 2: 2/3 - 2/15) (SHADAC Blog)
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey (Update: 1/10 - 2/1) (SHADAC Blog)
COVID-19 Vaccination Rates: New State-level and Subpopulation Evidence from the Household Pulse Survey (1/6 - 1/18) (SHADAC Blog)
Related Reading
State-level Flu Vaccination Rates among Key Population Subgroups (50-state profiles) (SHADAC Infographics)
50-State Infographics: A State-level Look at Flu Vaccination Rates among Key Population Subgroups (SHADAC Blog)
Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (SHADAC Brief)
New Brief Examines Flu Vaccine Patterns as a Proxy for COVID – Anticipating and Addressing Coronavirus Vaccination Campaign Challenges at the National and State Level (SHADAC Blog)
Ensuring Equity: State Strategies for Monitoring COVID-19 Vaccination Rates by Race and Other Priority Populations (Expert Perspective for State Health & Value Strategies)
SHADAC Webinar - Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (February 4th) (SHADAC Webinar)









