Blog & News
Employer-Sponsored Insurance, 2013-2017: Premiums Grow Faster, Deductibles Continue to Increase - Chartbook and State Fact Sheets
October 1, 2018:The nation’s attention has recently concentrated on health insurance coverage purchased through Affordable Care Act marketplaces, but it is important to remember that the majority of non-elderly Americans (51.6%) continue to get their health insurance coverage from an employer.[1] A new analysis from SHADAC uses data from the Medical Expenditure Panel Survey (MEPS) to highlight the experiences of private sector workers with employer-sponsored insurance (ESI) from 2013 through 2017 at the national level and within the states.
Key Findings
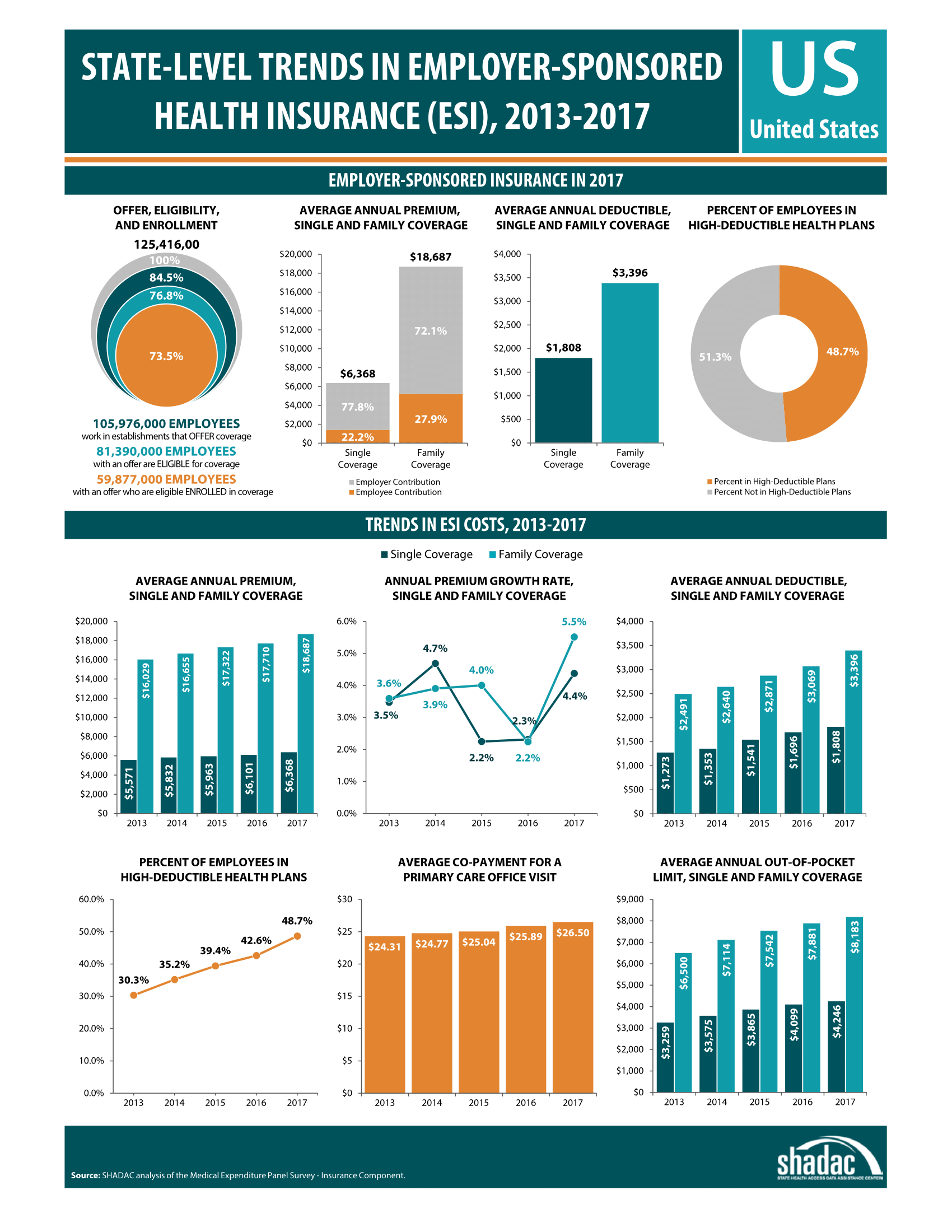 The percent of eligible U.S. employees receiving health coverage through ESI held steady in 2017, at 73.5 percent, representing nearly 60 million employees.
The percent of eligible U.S. employees receiving health coverage through ESI held steady in 2017, at 73.5 percent, representing nearly 60 million employees.- Nationwide, the percentage of employers offering health insurance coverage grew 3.5% to 46.9% from 2016 to 2017; however, there were no significant changes in the percent of employees that had an offer of coverage, the percent of employees that were eligible for coverage offered, or the percent of eligible employees that took up coverage.
- In 2017 the average annual single-coverage premium rose $267 to $6,368 nationwide. This marked a 4.4% increase from 2016--the highest annual growth rate for single-coverage premiums since 2014.
- The average annual family-coverage premium rose $977 to $18,687 in 2017. This was a 5.5% increase from 2016 and the highest annual rate of growth for family-coverage premiums in the last five years.
- The average annual single-coverage deductible nationwide rose $112 to $1,808 in 2017, a 6.6% increase from 2016.
- The average annual family-coverage deductible rose $327 to $3,396 in 2017, a 10.7% increase from 2016.
- In 2017, almost half of private-sector employees nationwide who had ESI (48.7%) were enrolled in a high-deductible health plan.[2] Enrollment in high-deductible health plans has been steadily rising and increased 14.2% between 2016 and 2017.
- The average annual out-of-pocket limit for single-coverage rose $147 to $4,246, a 3.6% increase from 2016.
- The average copayment for an office visit to a general practitioner rose $0.61 to $26.50, an increase of 2.4% from 2016; the average co-payment for a visit to a specialist rose $1.68 to $41.97, a 4.2% increase from 2016.
- State variation in access to and enrollment in ESI plans, along with variation in ESI premiums, deductibles, and cost-sharing, continued.
The Takeaway
Employer-sponsored insurance continues to be the backbone of the insurance coverage system in the United States, covering more than half the population. The level of financial protection offered by ESI has continued to decline steadily in the form of higher deductibles; however, for the first time in recent years this decrease in financial protection was accompanied by an acceleration of the growth in premiums. Given the dominant role of employer coverage in the broader coverage landscape, it is important to note that changes in the costs and value of employer coverage affect a significant number of people.
Explore the Analysis
The following products present findings from this analysis:
- Chartbook highlighting key findings on levels of, and trends in: average ESI premiums, deductibles, and employee cost sharing, as well as employee access to and take up of ESI coverage
- Two-page fact sheets on ESI for each state
- 50-state interactive map showing levels of, and changes in, average annual premiums for single-coverage in 2017, with links to state profile pages
- 50-state comparison tables
About the Data
This analysis uses data from the Medical Expenditure Panel Survey-Insurance Component (MEPS-IC).
Related Reading
New 2017 MEPS-IC Data: ESI Offer Rate Held Steady, but Premiums Continued to Rise and More Employees Enrolled in High Deductible Plans
SHADAC Blog
[1] SHADAC analysis of the 2016 American Community Survey (ACS) Public Use Microdata Sample Files.
[2] For the purposes of this analysis, high-deductible health plans are defined as plans that meet the minimum deductible amount required for Health Savings Account (HSA) eligibility ($1,300 for an individual and $2,600 for a family in 2017). This includes employees enrolled in single- and family-coverage plans.









