Publication
Room to Grow: Inequities in Children's Health Insurance Coverage
Health insurance is a linchpin in the United States’ health care system. It can insulate families from deep financial strain and medical debt, as costs for health care services have grown increasingly unaffordable in recent decades. For children, the doorway to health care offered by insurance is uniquely important—ensuring their opportunity to develop into healthy adults by providing access to regular health screenings, routine services, vaccinations, and vital treatments when health issues are identified.
 Children’s health insurance coverage rates in the United States have improved since the 1990s, largely due to policy initiatives designed to provide kids with affordable health insurance options, such as the long-running Children’s Health Insurance Program (CHIP) established twenty-five years ago.1 However, while overall uninsured rates remain low, disparities among select groups of children have persisted, with wide gaps in coverage found across the states and certain demographic categories.
Children’s health insurance coverage rates in the United States have improved since the 1990s, largely due to policy initiatives designed to provide kids with affordable health insurance options, such as the long-running Children’s Health Insurance Program (CHIP) established twenty-five years ago.1 However, while overall uninsured rates remain low, disparities among select groups of children have persisted, with wide gaps in coverage found across the states and certain demographic categories.
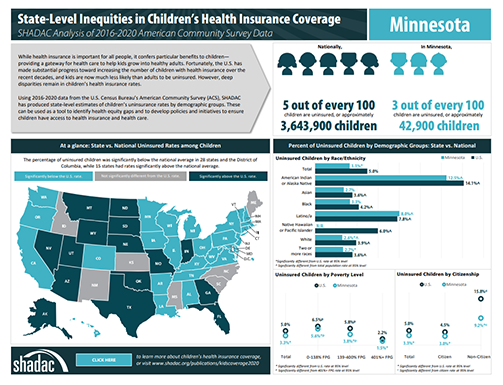
In this issue brief and accompanying 50-state profiles, SHADAC researchers explore rates of uninsurance among children in the U.S. using 2016-2020 estimates from the U.S. Census Bureau’s American Community Survey (ACS). Aiming to quantify coverage disparities in the states, this analysis looks at rates of uninsurance by race and ethnicity, income as measured by poverty level, citizenship status, age, and metropolitan status. These products can be used to identify health equity gaps and develop policies and initiatives to ensure children have needed access to health insurance and health care.
Uninsured Children by State, 2016-2020
Click on a state in the graphic below to view its kid's coverage profile. Click here to download all 50-state profiles.
1 Gates, J.A., Karpman, M., Kenney, G.M., & McMorrow, S. (2016). Uninsurance among children, 1997–2015: Long-term trends and recent patterns. Urban Institute. https://www.urban.org/sites/default/files/publication/79316/2000732-Uninsurance-among-Children-Long-Term-Trends-and-Recent-Patterns.pdf
Blog & News
2021 ACS: Estimates Show Declining Uninsurance Rates Across 28 States, Driven by Rise in Public Coverage and Fall in Private Coverage
September 15, 2022:
In a slight departure from their normal process, the U.S. Census Bureau released all 2021 estimates from the American Community Survey (ACS) today, which included state-level information about health insurance coverage by coverage type as well by certain demographic categories. The Census Bureau also released an accompanying report and blog post highlighting many of the changes seen from 2019 to 2021.*
Overall, the data showed a decrease in the number of people who were uninsured at the time of the survey: 8.6% in 2021, down 0.5 percentage points (PP) from 9.2% of the population in 2019. This echoes the drops in uninsurance shown by the recently released Current Population Survey (CPS) estimates (8.3% in 2021 from 8.6% in 2020), as well as the NHIS (9.2% in 2021 from 9.7% in 2020, though this change was not statistically significant).
This blog post highlights some of the national and state-level changes in the broadest categories of insurance (uninsurance, public coverage, and private coverage), and takes a look at the changes in rates by two age groups, nonelderly adults (age 19-64) and children (age 0-18), across the states.
Key Findings from the 2021 ACS: Uninsurance, Public Coverage, and Private Coverage
Alongside the national decline in uninsurance, 28 states also experienced significant decreases in their rates of uninsured. Maine saw the largest decrease, falling 2.3 PP from 8.0% in 2019 to 5.7% in 2021. North Dakota was the only state to experience an increase in its uninsured rate, which rose by 1.0 PP from 6.9% in 2019 to 7.9% in 2021. Uninsured rates ranged from a low of 2.5% in Massachusetts to a high of 18.0% in Texas. Though we are unable to compare to estimates in 2020, these states continued a trend of having the lowest and highest rates of uninsurance from 2018 and 2019.
When looking at public coverage, rates increased to 36.8% in 2021 from 35.4% in 2019—a 1.4 PP increase. This trend was echoed by rising rates of public coverage across 36 states, and no states saw decreases in public coverage in 2021 as compared to 2019. Rates of public coverage ranged from a low of 22.3% in Utah to a high of 50.9% in New Mexico. Idaho saw the largest increase in public coverage from 2019 to 2021, rising 4.3 PP to 36.8% last year.
Conversely, rates of private coverage declined across the nation and among 18 states in 2021. The percentage of individuals with private coverage decreased 0.4 PP from 67.4% in 2019 to 67.0% last year. Private coverage rates ranged from a low of 53.3% in New Mexico to a high of 77.8% in Utah. Rhode Island experienced the largest drop in private coverage, falling 4.2 PP to 69.2% in 2021 from 73.3% in 2019. Florida was the only state to see an increase in private coverage, rising 0.7 PP to 63.1% in 2021 from 62.5% in 2019.
State-Level Uninsurance by Age
Uninsurance fell among nonelderly adults in 2021, declining by 0.7 PP to 12.2% from 12.9% in 2019. 26 states also saw decreases in their uninsured rates for nonelderly adults, and only North Dakota saw an increase, rising 1.9 PP to 10.1%. The largest decrease in uninsurance was seen in Idaho, whose rate of uninsured nonelderly adults dropped precipitously by 4.4 PP to 12.1% in 2021 from 16.5% in 2019.
Children also saw an overall decrease in uninsurance last year, falling 0.3 PP to just 5.4% in 2021. This was echoed by falling uninsured rates in ten states, with increases seen in just two—Idaho and Maryland. Oklahoma had the largest decrease in the rate of uninsured children, falling 1.2 PP from 8.6% in 2019 to 7.4% in 2021.
Changes in State-Level Uninsurance Rates by Age, 2019 vs. 2021
State-Level Public Coverage by Age
Examining rates of public coverage for nonelderly adults showed an overall increase of 1.4 PP from 2019 to 2021, rising from 17.7% to 19.1%. 35 states also saw public coverage increase among nonelderly adults, with no states reporting decreases. Once again, Idaho was the state to report the largest increase in public coverage for nonelderly adults, rising 7.1 PP to 19.4% in 2021.
Similarly, rates of public coverage rose by 1.4 PP for children from 2019 to 2021—an increase reflected across 23 states. Just one state, Montana, saw a decrease in public coverage among children from 2019 to 2021 (42.0% to 37.7%, a difference of 4.3 PP). Rhode Island saw the largest increase from 2019 to 2021, rising 7.1 PP to 40.3% of children covered by public insurance in the state.
Changes in State-Level Public Coverage by Age, 2019 vs. 2021
State-Level Private Coverage by Age
Overall, rates of private coverage remained unchanged for nonelderly adults in 2021, likely due to a mix of states reporting rate changes (7 increased and 11 decreased) in this type of coverage. Nonelderly adults in Maine saw the largest increase in public coverage, rising 1.9 PP to 75.9% in 2021. Rhode Island reported the largest decrease, dropping 3.3 PP to 74.4% in 2021.
Children also saw fewer changes in private coverage rates, both at the national level (rate of 60.5% coverage was statistically unchanged from 2019 to 2021) and across the states, with 5 reporting increases and 3 reporting significant decreases. Pennsylvania and Tennessee both reported the largest increase in private coverage for children, rising 1.9 PP to 65.4% and 60.6%, respectively. Rhode Island’s rate of private coverage among children saw a large drop from 2019 to 2021, falling 8.4 PP to 64.6%.
Changes in State-Level Private Coverage by Age, 2019 vs. 2021
Future Data Releases and Products
Supplemental tables for the 2021 ACS 1-Year Estimates will be released from the U.S. Census Bureau on October 20, 2021, and 2017-2021 ACS 5-Year Estimates will be available on December 8, 2021.
Stay tuned for more granular details about insurance coverage changes in the states from 2019 to 2021 via customized SHADAC tables examining coverage at the state and county level.
As this blog noted, changing rates of public and private coverage in 2021 drove overall declines in uninsured rates. Further analysis shows that these changes were, in turn, driven by shifts in Medicaid, employer-sponsored insurance (ESI), and direct-purchase coverage. A SHADAC blog post taking a deep dive into these trends will be published next week. In the meantime, to learn more about our latest research on ESI trends, check out our recent narrative report and 50-state comparison tables.
Related Materials
Recent Blog: CPS ASEC: 2021 National Health Insurance Coverage Estimates Show Falling Uninsured and Private Coverage Rates Across Population Demographics (Infographic)
Upcoming Webinar: SHADAC Hosting An Annual Conversation with the U.S. Census Bureau to talk Health Insurance Coverage Estimates from the 2021 ACS and CPS
On Thursday, September 29th at 1:00 PM Central Time (2:00 PM Eastern), SHADAC will host a webinar to examine the new 2021 coverage estimates from the ACS as well as from the Current Population Survey (CPS), with technical insight provided by researchers from SHADAC and special guests Sharon Stern and Laryssa Mykyta from the U.S. Census Bureau, which administers both surveys.
Speakers will discuss the new national and state-level estimates, and attendees will learn when to use which estimates from which survey, how to access the estimates via the data.census.gov site and the new ACS table formats, and there will be an opportunity to ask questions after the speaker presentations.
Register for the webinar here!
*Comparisons with 2020 ACS Data
As has been extensively documented by both SHADAC and the Census Bureau, disruptions to data collection and dissemination efforts—as well as the presence of significant nonresponse bias—due to the COVID-19 pandemic heavily impacted estimates for 2020. As such, the Census Bureau released 2020 ACS 1-year data in an “experimental-only” format and cautioned against their use. Similarly, the Census Bureau recommends that data users do not compare 2020 ACS 1-year experimental estimates with any other data.
Notes
All changes described in this document are significant at the 90% level. Private coverage includes individually purchased and employer-sponsored coverage.
Overarching estimates of uninsurance and public and private coverage are for all ages, except where noted for children (age 0-18) and nonelderly adults (19-64).
Blog & News
CPS ASEC: 2021 National Health Insurance Coverage Estimates Show Falling Uninsured and Private Coverage Rates Across Population Demographics (Infographic)
September 13, 2022:The U.S. Census Bureau has released an initial report detailing the state of health insurance coverage in the United States for 2021. Drawing on data from the Current Population Survey Annual Social and Economic Supplement (CPS ASEC), the report highlights good news overall as the percentage of the population without health insurance coverage at any point in 2021 fell to 8.3% from 8.6% in 2020—a decrease of 0.4 percentage points (PP) or approximately 1.1 million people (27.2 million in 2021 vs. 28.3 million in 2020).
While this year marks a return to a more standard release of health insurance coverage estimates after COVID-related factors impacted the release of 2020 from the CPS and, to a larger degree, the American Community Survey (ACS), the report did not include any state-level estimates from the ACS, as have been provided in past years. Instead, the Census Bureau plans to release all data relating to the ACS on Thursday, September 15, 2022.
The CPS ASEC does provide important breakdowns of available health insurance coverage estimates at the national level, including by age, race and ethnicity, immigration status, marital status, geographic region, employment, poverty status, and Medicaid expansion status.
The following blog and infographic explore changes in coverage rates by demographic for nonelderly adults (age 19-64) and for children (age 0-18), who experienced a greater number of changes in insurance coverage both overall and across categories than their adult counterparts.
Changes in Uninsurance by Age and Characteristics
Among nonelderly adults (age 19-64), the overall rate of uninsurance remained statistically unchanged from the previous year, reported at 11.6% in 2021 compared to 11.9% in 2020.
Comparatively, children (age 0-18) had an uninsured rate of 5.0% in 2021, a decrease from 5.6% the previous year.
Race and ethnicity
While uninsurance rates also remained unchanged across a number of racial and ethnic groups in 2021—7.5% for White adults, 7.7% for Asian adults, and 25.1% for Hispanic adults—the rate of uninsurance fell significantly among Black nonelderly adults, decreasing to 12.7% in 2021 from 14.2% in 2020.
Similarly, while uninsurance rates remained stable for children of several racial and ethnic groups in 2021—3.4% for White children and 8.6% for Hispanic children—the rate of uninsurance dropped significantly among Black children, falling to 4.3% in 2021 from 5.9% in 2020. Asian children, however, saw an increase in rates of uninsurance, rising to 4.6% in 2021 from 2.8% in 2020.
Immigration status
The rate of uninsurance among native-born nonelderly adults fell to 9.1% in 2021 from 9.6% in 2020, while the uninsurance rate among foreign-born adults remained statistically unchanged at 22.8% in 2021 compared to 22.9% in 2020.
Rates of uninsurance also fell among native-born children, decreasing to 4.5% in 2021 from 5.2% in 2020, while again, the uninsurance rate for foreign-born children was statistically unchanged at 18.6% in 2021.
Poverty level
When examining coverage by poverty level, rates of uninsurance among nonelderly adults were broadly unchanged for each measurable category: 24.0% among those with incomes below 100% poverty, 16.7% for those between 100%-399% poverty, and 4.5% for those living at or above 400% poverty.
In 2021, rates of uninsurance were unchanged for children in the two lower poverty level categories—8.3% for those in families with incomes below 100% poverty and 6.4% for those living in families with incomes between 100%-399% poverty. However, uninsured rates fell to 1.7% among children in families with incomes at or above 400% of poverty, a decrease of 0.4 PP from 2020.
Medicaid expansion status
As of January 1, 2021, 36 states and the District of Columbia have chosen to act on the option provided by the Affordable Care Act (ACA) and expand Medicaid eligibility requirements. Comparing rates of uninsurance by expansion and nonexpansion states revealed parallel trends for both nonelderly adults and children.
In 2021, the overall uninsured rate remained statistically unchanged from 2020 (9.0% in both years) for adults living in expansion states. However, uninsurance dropped from 17.7% in 2020 to 16.7% in 2021 for adults living in nonexpansion states.
Similarly, children in expansion states saw no change in uninsured rates for 2021 compared to 2020 (4.0% in both years). And again, uninsurance fell in nonexpansion states, falling to 7.1% in 2021 from 8.6% in 2020.
Other Notable Coverage Changes
Public and private coverage
Other notable overarching trends included a higher percentage of the population with public coverage, increasing 1.2 PP to 35.7% in 2021 from 34.5% in 2020, and a consequent decrease in the percentage of the population with private coverage, measuring at 66.0% in 2021, a decrease of 0.6 PP from 2020 (66.5%). The largest drivers of public and private coverage changes were a 0.9 PP increase in Medicaid coverage (18.9% in 2021, up from 17.9% in 2020) and a 0.2 PP drop in employment-based coverage (54.3% in 2021, down from 54.6% in 2020).
Poverty level
Of particular note in the report was a consistent correlation between poverty level for both adults and children and changes in rates of public and private insurance coverage between 2020 and 2021.
Rates of public coverage rose among adults in all poverty categories, increasing 2.4 PP to 51.8% among those with incomes below 100% of poverty, 0.8 PP to 25.4% for those between 100%-399% of poverty, and 0.5 PP to 5.7% among those living at or above 400% of poverty.
Rates of public coverage also increased by 2.0 PP to 44.2% among children in families with incomes between 100%-399% and by 1.2 PP to 7.2% for children in families at or above 400% of poverty. Rates of public coverage were unchanged among children below 100% of poverty (79.7%).
Looking at private coverage changes, uninsurance rates remained unchanged among adults in all poverty categories at 27.1%, 61.8%, and 91.8% for those with incomes below 100% of poverty, between 100%-399% of poverty, and at or above 400% of poverty, respectively.
Similarly, rates of private coverage were largely unchanged among children in families with incomes below 100% of poverty and those in families at or above 400% of poverty at 15.5% and 93.2%, respectively. Rates of private coverage did decrease in one category: children in families with incomes between 100%-399% of poverty, dropping by 1.5 PP to 53.4% in 2021.
Employment
Overall, rates of uninsurance fell amongst workers, decreasing to 10.7% in 2021 from 11.2% in 2020, driven by a decrease in adults who worked less than full-time year-round (15.1% in 2021 vs. 16.4% in 2020). Among those who worked full-time year-round, uninsurance did increase to 9.1% in 2021 from 8.4% in 2020, and among those who did not work in 2021, the rate of uninsurance remained unchanged at 14.8%.
Related Releases and Products
As previously mentioned, the Census Bureau will be releasing the full roster of 2021 estimates from the American Community Survey (ACS) on Thursday, September 15. SHADAC will be monitoring this release and providing updates, along with several blog posts analyzing the estimates, as soon as they are available.
In a follow-up to several blogs and reports released in 2021 that detailed the effects of COVID-19 on the 2020 CPS and ACS health insurance coverage data estimates, a new blog from the Census Bureau looks at the continuing impact of the pandemic on survey data collection and release processes and nonresponse bias.
Though data collection operations were mostly able to resume as normal, lower-than-usual response rates persisted into 2022, measuring at 72% compared to 76% in 2021. Prior to the pandemic (2018 and earlier), the CPS enjoyed some of the highest response rates across a number of federal surveys, consistently recording percentages in the high 80s and low 90s.
Additionally, the blog notes the continued presence of measurable nonresponse bias, particularly in categories of income statistics and poverty rates. While the CPS standard weighting methodology (described fully in the ASEC technical documentation) was able to account for differences in survey estimates and administrative data prior to 2019, figures in the blog show that both standard and even alternative weights employed by the Census Bureau have not been able to fully adjust for differences between respondents and nonrespondents since 2020, highlighting the fact that certain pandemic-era challenges still persist.
Notes
All changes are statistically significant at the 90 percent confidence level.
All estimates come from the 2021 and 2022 Current Population Survey Annual Social and Economic Supplement, which provide data for years 2020 and 2021, respectively.
Both the 2020 and 2021 estimates use 2020 Census-based population controls, meaning that estimates for 2020 listed in the current report may not always match those listed in the report published in September 2021, which used 2010 Census-based population controls.
Uninsured estimates represent individuals with no health insurance coverage for the entire calendar year.
Estimates of health insurance coverage type represent individuals with that type of coverage at any point during the calendar year. Types of health insurance coverage are not mutually exclusive.
Publication
State-Level Trends in Employer-Sponsored Health Insurance, 2019-2021
The COVID-19 pandemic has altered long-standing patterns of life and work in the United States and internationally. The pandemic, along with the associated policy response, led to (at least temporary) changes in Americans’ primary source of health insurance coverage, with more Americans enrolled in public coverage and fewer in private. Despite these shifts, employer-sponsored health insurance (ESI) remains the largest single source of coverage for most Americans, with 62.2 million private-sector workers enrolled in ESI in 2021. This report considers how trends in ESI coverage and cost have evolved over the past three years, since the pre-pandemic baseline (2019), since the first year of the pandemic (2020), and in 2021, as the country emerges from pandemic-related restrictions and economic dislocation. These analyses use estimates from the Medical Expenditure Panel Survey-Insurance Component (MEPS-IC), recently produced by the Agency for Healthcare Research and Quality (AHRQ).
This narrative also provides an overview of the 2021 MEPS-IC private-sector ESI estimates, covering changes in market composition, ESI access, and cost. Because changes in the labor market caused by COVID-19 likely had a large influence on measures of ESI access in 2020, the analysis of ESI access will compare 2021 estimates against a pre-pandemic baseline of 2019. However, the pandemic likely had a smaller impact on long-running cost trends, so the analysis of ESI costs will compare 2021 estimates against 2020.
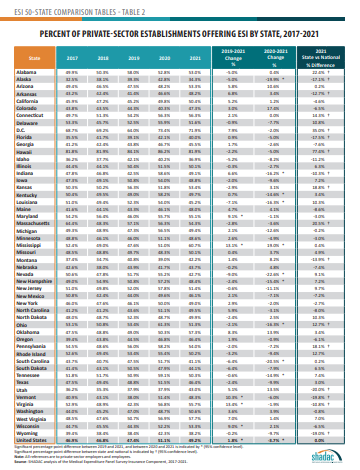
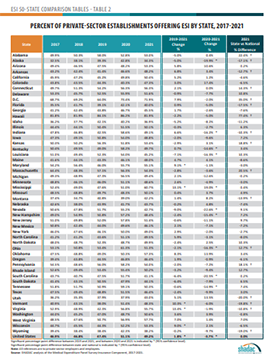
Accompanying this narrative are detailed 50-state comparison tables that allow for easy cross-state analysis of ESI trends from 2017 to 2021, significant changes in ESI rates from 2019 to 2021 and 2020 to 2021, and state vs national average comparisons for 2021 estimates.
For more detailed information on ESI findings from SHADAC, see the following products:
- Printable version of this ESI Report Narrative
- Companion Blog and Infographic highlighting key findings in ESI coverage at the national level
- 50-State Comparison Tables including 2017-2021 ESI estimates
- 2020 ESI Blog covering pandemic-era trends
Blog & News
Employer-Sponsored Insurance (2019-2021): A National-Level Look at Cost and Coverage Rates (Infographic)
August 30, 2022:Throughout the United States, a majority of Americans and their families receive health insurance coverage through their employer. In 2021, the number of individuals enrolled in this type of coverage–known as employer-sponsored insurance or ESI–exceeded 62.2 million. In this blog, infographic, and companion documents, SHADAC researchers use data from the Medical Expenditure Panel Survey-Insurance Component (MEPS-IC) to analyze the private-sector ESI landscape in 2021 on a national level and within the states. As discussed in SHADAC’s 2020 ESI coverage blog, the COVID-19 pandemic complicated the collection and analysis of data throughout recent years, leading our researchers to compare 2021 ESI access data against pre-pandemic (2019) estimates and 2021 ESI cost data against 2020 estimates.
Key Findings
Employee Access to Coverage (2019 vs. 2021)
Establishment
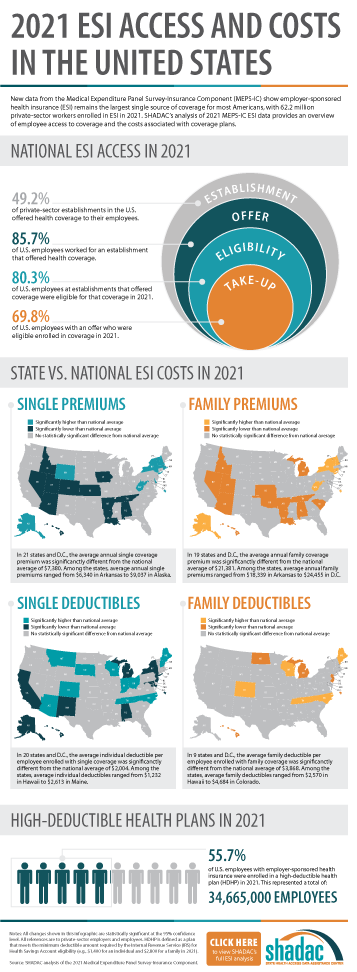
Not all private sector establishments offer their employees health insurance coverage. In fact, slightly less than half of establishments in the U.S. offered coverage in 2021 (49.2%). This was a significant increase from 47.4% in 2019.
Offer
The offer of employer-sponsored insurance coverage was extended to the majority of private-sector employees. In 2021, 85.7% of employees in the U.S. worked in establishments that offered health insurance coverage, a rate that remained statistically unchanged from 2019 (85.3%).
Eligibility
Among employees working at establishments that offered coverage, the percent eligible for coverage was 80.3% in 2021; an increase from 77.7% in 2019.
Take-Up
The take-up rate of ESI-eligible employees has varied over the years, and in 2021, 69.8% of eligible employees enrolled in coverage. This represented a 2.1 percentage-point decrease from 2019 (71.9%).
Employee Coverage Costs (2020 vs. 2021)
Premiums and contributions
- The average annual premium for single coverage rose to $7,380 in 2021, a $231 or 3.2% increase from 2020.
- For those enrolled in family coverage, average annual premiums also rose. In this case, premiums climbed to $21,381 in 2021, a $623 or 3.0% increase from 2020.
Deductibles
- For single coverage, the 2021 average individual deductible was $2,004. This represented a significant increase of 3.0% from 2020 ($1,945).
- Among those enrolled in family coverage, the average deductible per employee enrolled was $3,868 in 2021. This was also a significant increase of 3.9% from 2020 ($3,722).
High-Deductible Health Plans
- In 2021, the share of employees enrolled in high-deductible health plans (HDHPs) increased substantially in 2021 to 55.7% – an increase of 5.3 percentage points from 2020.
Key Takeaways
With so many Americans relying on their employers for health insurance coverage, ESI findings remain an important indicator of the financial and health burdens many individuals and families face. In 2021, the U.S. experienced several continuing ESI trends, including rising costs across employee premiums, premium contributions, and deductibles. Additionally, the share of private sector employees enrolled in high-deductible plans increased substantially. In regards to coverage, more employers offered ESI to their employees in 2021 when compared to pre-pandemic levels. Meanwhile, the rate of ESI-eligible employees enrolling in offered coverage was down overall from pre-pandemic, though unchanged from 2020.
For more detailed information on ESI findings from SHADAC, see the following products:

 Report Narrative
Report Narrative
The report narrative provides an in-depth look at 2019-2021 ESI estimates including state-level changes and trends.
50-State Comparison Tables
The 50-state tables include 2017-2021 ESI estimates and allow for easy cross-state and state vs. national analysis.
Other related resources
• 2021 ESI Blog (2019-2020 data)
• 2020 ESI Report, Blog, and Infographic (2015-2019 data)
• 2019 ESI Report, Blog, and Infographic (2014-2018 data)