Blog & News
COVID-19 Vaccination Rates: State-level and Subpopulation Evidence from the Household Pulse Survey (Update 2: Feb 3 to Feb 15)
February 25, 2021:Newly available COVID-19 vaccines promise to help protect individual Americans against infection and eventually provide population-level herd immunity. The pace of the COVID-19 vaccination rollout in the United States has been somewhat erratic—with reports of slow early going before picking up somewhat in following weeks, only to be hampered by recent storms across the southern region. However, signs of vaccination progress are appearing on the horizon once again, with manufacturers ramping up production, shipping getting back on track after the recent roadblocks, and early positive news from the FDA regarding Johnson & Johnson’s single-shot vaccine. The initial groups prioritized for vaccination were health care workers on the front lines of the pandemic and nursing facility residents, many of whom are especially vulnerable to COVID-19 infection and severe outcomes.
While these groups continue to hold priority in vaccination slots, many states have expanded vaccine access to other (still high-priority) segments of the general population such as older adults, K-12 and child care workers, essential workers, and those with high-risk medical conditions. However, there are concerns that these prioritization decisions and the existing mechanisms of the vaccine rollout—in addition to evidence that lower-income individuals, people of color, and individuals without strong connections to the health care system are less likely to get vaccinated—are inadequate to narrow the clear disparities in the vaccine rollout so far and could worsen existing pandemic-related health inequities.
The available data have not assuaged these concerns, and show patterns of lower vaccination rates among people with lower incomes and levels of education, and marginalized racial and ethnic groups. The U.S. Census Bureau recently released updated data on take-up of COVID-19 vaccines from the most recent wave of its Household Pulse Survey (HPS), collected February 3-15, 2021.1 The HPS is an ongoing, weekly tracking survey designed to measure impacts of the COVID-19 pandemic. These data provide an updated snapshot of COVID-19 vaccination rates and are the only data source to do so at the state level by subpopulation. This blog post presents top-level findings from these new data, focusing on rates of vaccination (one or more doses) among U.S. adults (age 18 and older) living in households and comparing to results from the most recent wave of the HPS, collected January 20-February 1, 2021.2
Nearly one in five adults had received a vaccination, but this varied by state
According to the new HPS data, 19.9% of U.S. adults had received one or more COVID-19 vaccinations during this two-week period in the first half of February, though this varied by state from a low of 16.3% in the District of Columbia (D.C.) to a high of 31.9% in Alaska. More than one in four adults had received a vaccine in three states: Alaska, Hawaii, and New Mexico.
Vaccination rates increased substantially across nearly all states; states with lower rates catching up
Nationally, adult vaccination rates were up from the previous wave of the HPS, increasing from 13.2% during January 20-February 1, 2021, to 19.9% during February 3-15, 2021. Most states also experienced increases in their vaccination rates, though again the size of these increases varied across the states, from an increase of 1.5 percentage points (PP) in Vermont to an increase of 10.9 PP in Wisconsin.
Percent of Adults Who Had Received a COVID-19 Vaccine

States that had previously had below-average vaccination rates caught up somewhat to the higher-performing states. The states that were below the national average in late January, such as California and Wisconsin, saw larger increases in their vaccination rates compared with the states that were above the national average in late January, so that by the middle of February, vaccination rates were somewhat more even across the states, with most states hovering just above or below 20% of their adult populations vaccinated.
Disparities in vaccination rates remain largely unchanged
COVID vaccination rates continued to vary to a great degree by demographic and socioeconomic factors, though disparities narrowed slightly from previous weeks. This narrowing could be due to the expansion of priority groups to include a broader share of the population over this period; however, progress has remained limited in getting vaccines to certain groups such as low-income, Hispanic, and Black adults, for instance, and new vaccination strategies may be needed to reach the hardest-to-reach groups such as these.
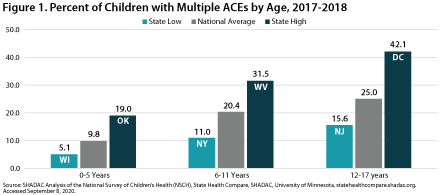
By race and ethnicity, non-Hispanic Asian and non-Hispanic White adults continued to have above-average vaccination rates at 25.3% and 21.5%, respectively. Vaccination rates among non-Hispanic adults identifying with “Multiple” races or “Some other” race, which had previously increased relative to the average, fell behind pace and rose to just 16.3%, below the national average of 19.9%. Rates among non-Hispanic Black adults (16.2%) and Hispanic/Latino adults of any race (15.0%) remained below the national average.
Percent of Adults Who Had Received a COVID-19 Vaccine by Race/Ethnicity
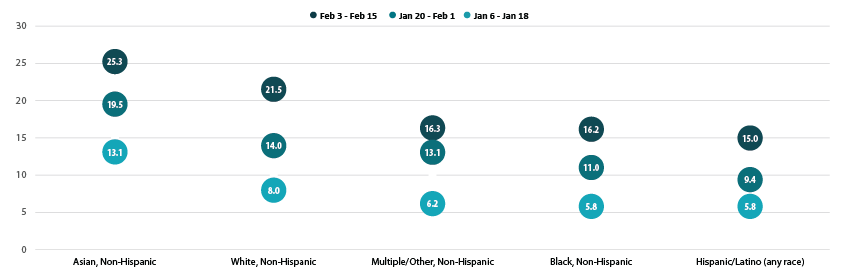
Disparities in vaccination rates by income continued to narrow, though rates among those with the lowest incomes remained far below the average. Adults with household incomes of less than $25,000 were nearly half as likely to have received a vaccine compared with all adults (10.7% vs. 19.9%). This gap was largely unchanged from previous weeks, even as the gap between other lower-income groups and the average steadily narrowed from early January.
Percent of Adults Who Had Received a COVID-19 Vaccine by Income
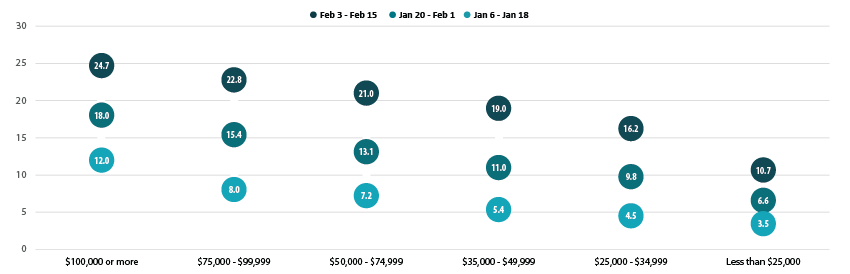
Disparities by level of education remained, with adults holding a bachelor’s degree or higher continued to have the highest vaccination rate at 28.2%, and adults without a high school diploma having the lowest vaccination rates at 12.2%. However, disparities by education did narrow somewhat, and vaccination rates among both adults with a high school diploma or equivalent and adults with less than a high school education increased faster than the overall adult rate.
Percent of Adults Who Had Received a COVID-19 Vaccine by Education
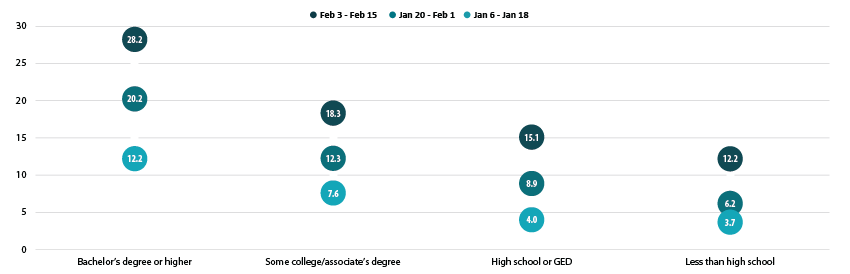
Nearly 2 in 5 older adults received a COVID vaccine as the U.S., and many states, continued to make large progress in vaccinating older adults
Nationally, 38.5% of older adults (age 65 and older) had received at least one dose of the COVID-19 vaccine, which was 18.6 percentage points higher than the rate among all adults (19.9%). Vaccination rates for older adults ranged from 17.6% in Rhode Island to 60.5% in Alaska. Older adult vaccination rates were below 25% in four states (New Hampshire, Oregon, Rhode Island, and Vermont) and at or above 50% in five states (Alaska, Georgia, Indiana, Mississippi, and Oklahoma) and in D.C.
Percent of Adults Age 65+ Who Had Received a COVID-19 Vaccine
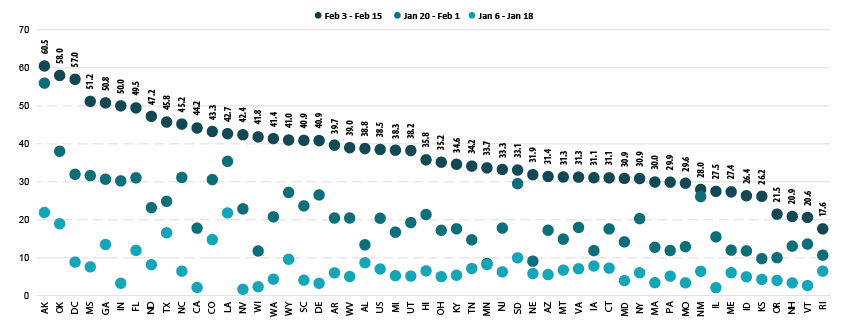
As in the previous period, states continued to make large progress in rates of vaccination among older adults. Compared to the end of January, 19 states more than doubled their 65+ vaccination rates, and three states (Minnesota, Wisconsin, and Nebraska) more than tripled their 65+ vaccination rates, with Minnesota nearly quadrupling its rate (from 8.5% to 33.7%). Only a handful of states failed to make substantial progress in increasing vaccination rates among older adults.
Notes about the Household Pulse Survey Data
The estimated rates presented in this post were calculated from the count estimates published by the Census Bureau. Though these counts are accompanied by standard errors, standard errors are not able to be accurately calculated for rate estimates. Therefore, we are not able to determine if the differences we found in our analysis are statistically significant or if the estimates themselves are statistically reliable. Estimates and differences for subpopulations at the state level should be assumed to have large confidence intervals around them and caution should be taken when drawing strong conclusions from this analysis. However, the fact that patterns of inequities in other vaccination rates are mirrored by these early indications of COVID-19 vaccination inequities demonstrates reason for concern.
Though produced by the U.S. Census Bureau, the HPS is considered an “experimental” survey and does not necessarily meet the Census’s high standards for data quality and statistical reliability. For example, the survey has relatively low response rates (7.3% for February 3-15), and sampled individuals are contacted via email and text message, asking them to complete an internet-based survey. These issues in particular could be potential sources of bias, but come with the tradeoffs of increased speed and flexibility in data collection as well as lower costs. A future post will investigate differences between COVID vaccination rates estimated from survey data (such as the HPS) and administrative sources. The estimates presented this post are based on responses from 77,122 adults. More information about the data and methods for the Household Pulse Survey can be found in a previous SHADAC blog post.
Previous Blogs in the Series
COVID-19 Vaccination Rates: New State-level and Subpopulation Evidence from the Household Pulse Survey (Update: Jan 10 to Feb 1)
COVID-19 Vaccination Rates: New State-level and Subpopulation Evidence from the Household Pulse Survey (Jan 6 to Jan 18)
Related Reading
State-level Flu Vaccination Rates among Key Population Subgroups (50-state profiles) (SHADAC Infographics)
50-State Infographics: A State-level Look at Flu Vaccination Rates among Key Population Subgroups (SHADAC Blog)
Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (SHADAC Brief)
New Brief Examines Flu Vaccine Patterns as a Proxy for COVID – Anticipating and Addressing Coronavirus Vaccination Campaign Challenges at the National and State Level (SHADAC Blog)
Ensuring Equity: State Strategies for Monitoring COVID-19 Vaccination Rates by Race and Other Priority Populations (Expert Perspective for State Health & Value Strategies)
SHADAC Webinar - Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (February 4th) (SHADAC Webinar)
Blog & News
COVID-19 Vaccination Rates: New State-level and Subpopulation Evidence from the Household Pulse Survey (Jan 6 to Jan 18)
January 29, 2021:Newly available COVID-19 vaccines promise to help protect individual Americans against infection and eventually provide population-level herd immunity. However, the rollout of the COVID-19 vaccines thus far—largely delegated to the states—has been slow and inconsistent. The initial groups prioritized for vaccination were health care workers on the front lines of the pandemic and nursing facility residents, many of whom are especially vulnerable to COVID-19 infection and severe outcomes. However, there are concerns that these prioritization decisions—in addition to evidence that lower-income individuals, people of color, and individuals without strong connections to the health care system are less likely to get vaccinated—could worsen existing pandemic-related health inequities.
Preliminary data have unfortunately reinforced these concerns, showing patterns of lower vaccination rates among people with lower incomes and levels of education, and marginalized racial and ethnic groups. The U.S. Census Bureau recently released new data on take-up of COVID-19 vaccines from the most recent wave of its Household Pulse Survey (HPS), collected January 6-18, 2021. The HPS is an ongoing, weekly tracking survey designed to measure impacts of the COVID-19 pandemic. These data are the first to provide estimates of COVID-19 vaccination rates at the state level and by subpopulation. This blog post presents top-level findings from these new data, focusing on rates of vaccination (one or more doses) among U.S. adults (age 18 and older) living in a household unit.1
Roughly eight percent of adults had received a vaccination, but this varies by state
According to the new HPS data, 7.7% of U.S. adults had received one or more COVID-19 vaccinations during this two week period in January, though this varied by state from a low of 5.4% in California to a high of 13.7% in Hawaii. More than one in ten adults had received a vaccine in nine states: Alaska, Hawaii, Montana, New Mexico, North Dakota, Oklahoma, South Dakota, Texas, and Vermont.
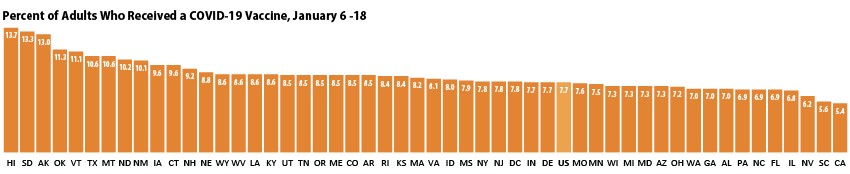
Disparities in vaccination rates reflect concerns about harder-to-reach groups and groups prioritized for initial round of vaccinations
Vaccination rates also varied substantially by a number of demographic and socioeconomic factors. These could be partly a result of decisions to prioritize health care workers, who tend to be less racially and ethnically diverse than the overall population, and who often have higher incomes and levels of education.
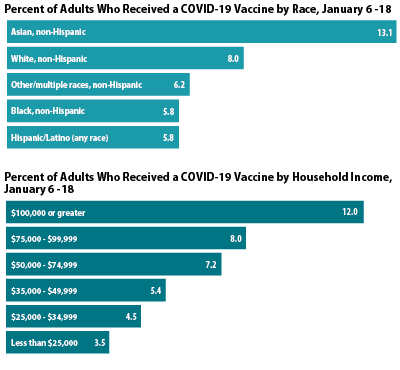 By race and ethnicity, non-Hispanic Asian adults had the highest vaccination rates at 13.1%, followed by non-Hispanic White adults at 8.0%. Hispanic/Latino adults (any race), non-Hispanic Black adults, and non-Hispanic adults identifying with multiple races or some other race had lower vaccination rates (5.8%, 5.8%, and 6.2%, respectively). A similar pattern was seen across many states, with Asian and White adults often more likely to have received a vaccine than Black and Hispanic adults.
By race and ethnicity, non-Hispanic Asian adults had the highest vaccination rates at 13.1%, followed by non-Hispanic White adults at 8.0%. Hispanic/Latino adults (any race), non-Hispanic Black adults, and non-Hispanic adults identifying with multiple races or some other race had lower vaccination rates (5.8%, 5.8%, and 6.2%, respectively). A similar pattern was seen across many states, with Asian and White adults often more likely to have received a vaccine than Black and Hispanic adults.
Large disparities in vaccination rates by income were also apparent, with the highest income groups reporting higher rates of vaccination compared to those with lower incomes, and rates increasing steadily in correlation with income. Of adults with household incomes of $100,000 or higher, 12.0% had received a COVID-19 vaccine, which was nearly 2.5x higher than the rate among those with incomes below $25,000.
Nearly half of all adults who had received a COVID-19 vaccine have incomes of at least $100,000, despite making up only three in ten adults in the overall population.
Similar patterns by income were seen across the states. For example, in 17 states, adults in the highest income category were at least 5x more likely to have been vaccinated than those in the lowest income category.
Patterns of vaccination by education were similar to those by income, with adults with less education being less likely to have received a vaccine compared to adults with more education. Nationally, 12.2% of adults with a bachelor’s degree or higher have received a vaccine compared with 3.7% of adults with less than a high school education.
More progress is needed in vaccinating the older adult population most vulnerable to severe COVID-19 morbidity and mortality
Nationally, older adults (age 65 older) were no more likely to have received a COVID-19 vaccine than the overall adult population. During the period of January 6 through January 18, 7.1% of older adults had received a vaccine compared with 7.7% of all adults. This may be of concern because older adults are more likely to develop severe COVID-19 cases or die from the disease compared to the general population. Consequently, many states have given precedence to vaccinations for older adults, but these early data don’t show that prioritization is resulting in higher vaccination rates.
Vaccination rates for older adults ranged from 1.7% in Nevada to 21.9% in Alaska. Vaccination rates were below five percent in 15 states and were above ten percent in seven states. Older adults were more likely to have received a vaccine than the overall population in just 11 states
Notes about the Household Pulse Survey Data
Many of the estimates published by the Census Bureau and presented here were not accompanied by standard errors. Therefore, we are not able to determine if the differences we found in our analysis are statistically significant or if the estimates themselves are statistically reliable. Estimates and differences should be assumed to have large confidence intervals around them—especially for subpopulations at the state level—and caution should be taken when drawing strong conclusions from this analysis. However, the fact that patterns of inequities in other vaccination rates are mirrored by these early indications of COVID-19 vaccination inequities demonstrates reason for concern.
Though produced by the U.S. Census Bureau, the HPS is considered an “experimental” survey and does not necessarily meet the Census’s high standards for data quality and statistical reliability. For example, the survey has relatively low response rates (6.5% for January 6–18) and sampled individuals are contacted via email and text message, asking them to complete an internet-based survey. These issues in particular could be potential sources of bias, but come with the tradeoffs of increased speed and flexibility in data collection as well as lower costs. The estimates presented this post are based on responses from 68,348 adults. More information about the data and methods for the Household Pulse Survey can be found in a previous SHADAC blog post.
Related Reading
Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (SHADAC Brief)
New Brief Examines Flu Vaccine Patterns as a Proxy for COVID – Anticipating and Addressing Coronavirus Vaccination Campaign Challenges at the National and State Level (SHADAC Blog)
Ensuring Equity: State Strategies for Monitoring COVID-19 Vaccination Rates by Race and Other Priority Populations (Expert Perspective for State Health & Value Strategies)
Upcoming SHADAC Webinar - Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (February 4th) (SHADAC Webinar)
1 It is important to mention that the HPS does not collect data for institutionalized adults, such as those living in nursing facilities. These individuals were commonly prioritized for the first rounds of COVID-19 vaccines, so the estimates of vaccination rates presented here are likely an undercount of population-wide vaccination rates. This undercount could be more pronounced among the total 65-and-older population, as they are disproportionately likely to reside in institutions. Further, these data do not represent adults in correctional facilities such as prisons or jails—another group of adults who are also at increased risk of contracting COVID-19.
Blog & News
SHADAC Webinar - Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (February 4)
August 01, 2024:Date: Thursday, February 4, 2021
Time: 1:00 PM Central Time / 2:00 PM Eastern Time
Across the country, states have begun the first stages of their campaigns to vaccinate people against the novel coronavirus (COVID-19). However, early troubles have highlighted the challenges to such a massive endeavor, as pointed out in recent articles from the New York Times and the Washington Post.
Once the first tiers of recipients have been vaccinated, states will need to begin subsequent efforts to inoculate their broader resident populations—efforts that may be hampered by another, more-familiar set of hurdles, including vaccine skepticism and a U.S. health care system that typically leaves large segments of the population underserved.
Looking to the nation’s experiences with other vaccine campaigns such as influenza, can provide insights to the challenges faced by states in attaining their targets for coronavirus immunization.
In a recent SHADAC webinar, Senior Research Fellow Colin Planalp, MPA, presented data published in a recent brief, funded by the California Health Care Foundation (CHCF). The analysis uses flu vaccination rates for U.S. adults across the 50 states and the District of Columbia as a proxy to identify population subgroups that may be harder to reach with a COVID-19 vaccine. An analysis of several demographic categories, such as age, race/ethnicity, chronic health conditions, and health insurance coverage status was also included in the webinar discussion.
Mr. Planalp was joined by SHADAC Research Fellow Robert Hest, MPP, for a question and answer session following the webinar presentation.
Related Resources
State-level Flu Vaccination Rates Among Key Population Subgroups (SHADAC 50-state Infographics)
50-State Infographics: A State-level Look at Flu Vaccination Rates among Key Population Subgroups (SHADAC Blog)
COVID-19 Vaccine Challenges: Illustrating Hurdles to Population Immunity and Equity Using Flu Vaccination Data (SHADAC Webinar Slides)
Anticipating COVID-19 Vaccination Challenges through Flu Vaccination Patterns (SHADAC Brief)
Ensuring Equity: State Strategies for Monitoring COVID-19 Vaccination Rates by Race and Other Priority Populations (SHVS Expert Perspective)
State-Specific Surveys Encompassing Residents’ COVID-19 Experiences (SHADAC Survey Resource)
Blog & News
State Health Compare Adds New Social Determinants Measure: Percent of Children with Adverse Childhood Experiences
September 14, 2020:A new State Health Compare measure examines the prevalence and degree of adverse childhood experiences (ACEs) among different demographic groups, with estimates available across the states and over time.
What are ACEs?
The Centers for Disease Control and Prevention (CDC) defines ACEs as “potentially traumatic events that occur in childhood (0-17 years)” including experiencing violence, abuse, or neglect; witnessing violence in the home or community; or having a family member attempt or die by suicide. ACEs also include “aspects of the child’s environment that can undermine their sense
of safety, stability, and bonding,” such growing up in a household with substance misuse, mental health problems, and instability due to parental separation or household members being in jail or prison.i
Why are ACEs Important?
A landmark study conducted in the 1990s found a significant relationship between the number of ACEs an individual experienced and a variety of negative outcomes in adulthood, including poor physical and mental health, substance abuse, and risky behaviors (e.g., smoking, having a history of sexually transmitted disease/infection, etc.). The more ACEs an individual experienced, the greater the risk of these outcomes.ii Because ACEs are common, with about 61% of adults reporting at least one type of ACE and nearly one in six reporting four or more types of ACEs, preventing ACEs
could reduce a large number of negative physical and behavioral health outcomes.iii
How Can We Prevent ACEs?
Creating and sustaining safe, stable, nurturing relationships and environments for children and families can prevent ACEs.iv Data on the prevalence and severity of ACEs among different groups can help policymakers and public health professionals target prevention efforts effectively so that resources are efficiently leveraged to support these relationships and environments where they are most needed.
What Can We Learn from the State Health Compare Estimates?
The ACEs estimates presented in State Health Compare indicate the percent of children with no ACEs, the percent of children with one ACE, and the percent of children with multiple ACEs. Breakdowns are available by age, insurance coverage type, education, poverty level, and race/ethnicity. Available time periods are the two-year pooled periods of 2016-2017 and 2017-2018
Children with ACEs: Data Highlights
Nationwide, an estimated 18.6% of all children (age 0-17) had multiple ACEs in 2017-2018, 23.3% had one ACE, and 58.2% had zero ACEs. The following section takes a quick dive into the percentages of children with multiple ACEs to highlight some of the subgroup analyses that are available using State Health Compare.
Percent of Children with Multiple ACEs: By Age Group
Figure 1 shows the national rates of children with multiple ACEs and state high and low rates for different age groups of children, with rates tending to be higher among older children and lower among younger children. Overall, the lowest percentage of children with multiple ACEs by age was 5.1% among 0-5 year-olds in Wisconsin, and the highest percentage was 42.1% among 12-17 year-olds in the District of Columbia (DC).
Percent of Children with Multiple ACEs: By Race/Ethnicity
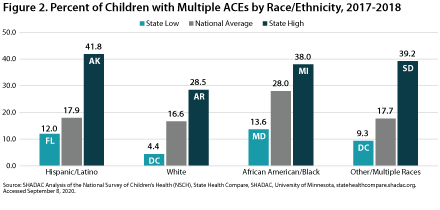 Figure 2 shows the national rates and state high and low rates for children with multiple ACEs by race/ethnicity in 2017-2018. When examining the national rate of children with multiple ACEs by race/ethnicity, as well as state-level highs and lows for this measure, White children consistently ranked at the bottom, with the lowest percentage being 4.4% among White children living in DC. The highest nation- wide percentage of children with multiple ACEs by race/ethnicity was among African American/Black children, of whom 28% had more than one ACE. The highest state-level percentage was 41.8% among Hispanic/Latino children living in Alaska.
Figure 2 shows the national rates and state high and low rates for children with multiple ACEs by race/ethnicity in 2017-2018. When examining the national rate of children with multiple ACEs by race/ethnicity, as well as state-level highs and lows for this measure, White children consistently ranked at the bottom, with the lowest percentage being 4.4% among White children living in DC. The highest nation- wide percentage of children with multiple ACEs by race/ethnicity was among African American/Black children, of whom 28% had more than one ACE. The highest state-level percentage was 41.8% among Hispanic/Latino children living in Alaska.
Percent of Children with Multiple ACEs: By Insurance Coverage Type
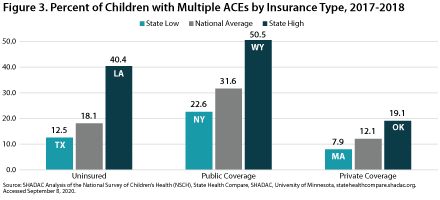 Figure 3 shows the percentage of children with two or more ACEs according to insurance status in 2017-2018. Nationwide, the highest proportion of children reporting multiple ACEs was among those with public coverage, at 31.6 percent. This is more than 2.5 times the nationwide low of 12.1 percent among children with private coverage. At the state level, a low of 7.9 percent of privately insured children in Massachusetts reported multiple ACEs, versus a high of 50.5 percent of publicly insured children in Wyoming.
Figure 3 shows the percentage of children with two or more ACEs according to insurance status in 2017-2018. Nationwide, the highest proportion of children reporting multiple ACEs was among those with public coverage, at 31.6 percent. This is more than 2.5 times the nationwide low of 12.1 percent among children with private coverage. At the state level, a low of 7.9 percent of privately insured children in Massachusetts reported multiple ACEs, versus a high of 50.5 percent of publicly insured children in Wyoming.
Percent of Children with Multiple ACEs: By Poverty Level
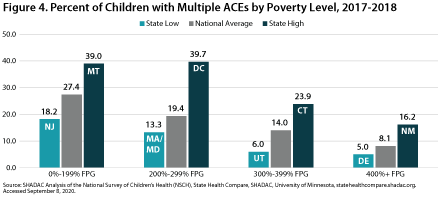 Figure 4 shows the prevalence of multiple ACEs by poverty level in 2017-2018. The national percentage of children who had multiple ACEs by poverty level was highest among children at 0 to 199 FPG at 27.4 percent. This proportion was lowest among children in household with incomes at or above 400 percent of the Federal Poverty Guideline (FPG) at 8.1 percent—a 19.3 percentage-point difference from the rate for high-income children. At the state level, the highest percentages of children with multiple ACES by poverty level were 39.7 percent among children at 200 to 299 percent FPG living in DC and 39.0 percent among children at 0 to 199 percent FPG living in Montana. The state low for multiple
Figure 4 shows the prevalence of multiple ACEs by poverty level in 2017-2018. The national percentage of children who had multiple ACEs by poverty level was highest among children at 0 to 199 FPG at 27.4 percent. This proportion was lowest among children in household with incomes at or above 400 percent of the Federal Poverty Guideline (FPG) at 8.1 percent—a 19.3 percentage-point difference from the rate for high-income children. At the state level, the highest percentages of children with multiple ACES by poverty level were 39.7 percent among children at 200 to 299 percent FPG living in DC and 39.0 percent among children at 0 to 199 percent FPG living in Montana. The state low for multiple
ACEs by poverty level was 5.0 percent among children at
or above 400 percent FPG living in Delaware.
Learn More
To explore State Health Compare’s ACEs estimates further, visit State Health Compare at statehealthcompare.shadac.org and click on “Explore Data.”
Other social and economic factors that can be explored through State Health Compare include:
i Centers for Disease Control and Prevention (CDC). (April 2020). “Preventing Adverse Childhood Experiences.” Available at https://www.cdc.gov/violenceprevention/acestudy/fastfact.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fviolenceprevention%2Fchildabuseandneglect%2Faces%2Ffastfact.html
ii Felitti, V.J., Anda, R.F., Nordenberg, D., Edwards, B.A., Koss, M.P., Marks, J.S. (May 1998). “Relationship of Childhood Abuse and Household Dysfunction to Many of the Leading Causes of Death in Adults.” American Journal of Preventive Medicine 14(4): 245-258. DOI: 10.1016/S0749-3797(98)00017-8.
iii Centers for Disease Control and Prevention (CDC). (April 2020). “Preventing Adverse Childhood Experiences.” Available at https://www.cdc.gov/violenceprevention/acestudy/fastfact.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fviolenceprevention%2Fchildabuseandneglect%2Faces%2Ffastfact.html
iv Ibid.
Blog & News
After drop in 2018, newer data indicate a resurgence in drug overdose deaths
August 26, 2020:While new SHADAC research found small but statistically significant declines in opioid and drug overdose death rates during 2018, newer data indicate those reductions may have been short-lived. Overall, in 2018, drug overdose death rates declined 4.6 percent as compared to the prior year, but our analysis also found variation in amounts and direction of changes in individual types of drugs. For instance, overdose death rates from prescription opioids dropped 14.7 percent and those from heroin dropped 3.8 percent, but overdose death rates from synthetic opioids (e.g., fentanyl) increased 9.6 percent and those from psychostimulants (e.g., methamphetamine) grew 22.1 percent.
Provisional data published by the U.S. Centers for Disease Control and Prevention show evidence of an increase in overall drug overdose deaths in 2019, as well as for certain individual types of drugs. During a rolling 12-month period ending in December 2019, drug overdose deaths reached a record high of 70,980—a 4.6 percent increase over the 12-month period ending in December 2018.1 And among the states, 36 of 50 saw increases in their reported drug overdose deaths. In that same amount of time, overdose deaths from synthetic opioids increased 15.8 percent and overdose deaths from psychostimulants increased 26.8 percent.
The state of Minnesota also recently published its own preliminary data on drug overdose deaths in 2019, finding similar patterns to the U.S. After experiencing a decline in drug overdose deaths in 2018, Minnesota reported that preliminary data showed a 20 percent increase in overall drug overdoses in 2019—in addition to synthetic opioid overdose deaths that increased by 48 percent, and psychostimulant overdose deaths that grew by 37 percent.2
Some reports also indicate that drug overdose deaths may have spiked in early 2020, coinciding with the beginning of the coronavirus pandemic and various associated stressors. For example, a White House analysis found an 11.4 percent increase in overdose deaths in the first four months of 2020 as compared to the prior year.3 In the midst of the COVID-19 emergency, experts such as those from the National Academy of Medicine have raised concerns that “the nation is experiencing an unprecedented convergence of epidemics, and there is great concern that the opioid crisis…may only worsen in the absence of a concerted response.”4
As new data on drug overdoses become available in the coming months and years, it will be vital to monitor the continually shifting dynamics of the opioid crisis, to identify early the emerging patterns—such as the rise of synthetic opioids and psychostimulants—and to continue to guide policy efforts to address the persistent public health emergencies of substance use and drug overdose deaths.
Explore SHADAC's most recent analysis of the Widening Drug Overdose Crisis in the United States or visit our Opioid Epidemic Resources page to access all opioid-related analysis done by SHADAC researchers over the last several years.
1 Ahmad, F.B., Rossen L.M., & Sutton, P. (2020). Provisional drug overdose death counts [National Center for Health Statistics report]. Available from https://www.cdc.gov/nchs/nvss/vsrr/drug-overdose-data.htm
2 DeLaquil, M., Giesel, S., & Wright, N. (n.d.). Preliminary 2019 drug overdose deaths: A return to the states’ overall trend [PDF file]. Retrieved from https://www.health.state.mn.us/communities/opioids/documents/2019prelimdeathreport.pdf
3 Ehley, B. (2020, July 2). Pandemic unleashes a spike in overdose deaths. Politico. Retrieved from https://www.politico.com/news/2020/06/29/pandemic-unleashes-a-spike-in-overdose-deaths-345183
4 National Academy of Medicine. (2020). Mapping our impacts. Available from https://nam.edu/programs/action-collaborative-on-countering-the-u-s-opioid-epidemic/mapping-our-impact/