Publication
Perceptions and Opinions Relating to Cannabis in Minnesota
Using data from the National Survey on Drug Use and Health (NSDUH), this brief explores people’s perceptions and opinions related to cannabis and cannabis use prior to its 2023 legalization in Minnesota. The brief begins with an overview of the context of cannabis policy and use in the United States before moving into analysis of perceptions on cannabis prior to legalization. Specifically, researchers analyzed respondents’ opinions on:
- How easy or hard it would be to obtain cannabis
- Perceived risk associated with smoking cannabis
- Disapproval (or lack thereof) of cannabis use by adults (age 18+) and youth (age 12-17)
 Researchers from the University of Minnesota School of Public Health’s State Health Access Data Assistance Center (SHADAC) and Cannabis Research Center (CRC) present data on these three topics for Minnesota specifically and for the U.S. as a whole.
Researchers from the University of Minnesota School of Public Health’s State Health Access Data Assistance Center (SHADAC) and Cannabis Research Center (CRC) present data on these three topics for Minnesota specifically and for the U.S. as a whole.
Examining data prior to legalization helps both researchers and the public understand Minnesota’s perceptions and attitudes surrounding cannabis before policy changes – then, as we move forward, we can compare this to post-policy data to understand what has changed, what hasn’t changed, and, hopefully, begin to answer common questions regarding cannabis use and legalization.
Will cannabis use increase with legalization? Will increased consumption lead to greater public health harms? Will rates of use increase for youth? Will perceived risk of use decrease with legalization?
“The answer [to these questions] may depend, in part, on whether the changing legal status of cannabis also changes social norms and people’s perceptions about cannabis, such as reducing social stigma associated with cannabis use,” says SHADAC and CRC Researcher Colin Planalp.
The data in this brief are intended to provide information to Minnesota policymakers as they set up the state’s regulatory framework surrounding cannabis. It also aims to give Minnesotans helpful information as they navigate the new choices that come with the lifting of decades of cannabis prohibition.
Continued research and monitoring of these and other issues will be crucial as cannabis policy, attitudes, and social norms evolve. Examining and understanding these opinions and perceptions can potentially reveal hints at how the cannabis landscape may change as a result of legalization.
Read the brief in full here. Additionally, SHADAC and the CRC authored a companion brief using the same survey data to examine the potential public health implications of cannabis policy in Minnesota. You can find that brief here.
Interested in learning more about cannabis policy in Minnesota, substance use, and related topics? Check out the following resources:
- SHADAC blog accompanying this brief - “Measuring Perceptions and Opinions on Cannabis Use in Minnesota”
- Brief on the United States Opioid Crisis – “Opioid Crisis in the Pandemic Era”
- Cannabis Research Center Website
- Explore data on the topic of substance use, alcohol-involved deaths, and more on State Health Compare
Blog & News
Measuring Perceptions and Opinions on Cannabis Use and Access in Minnesota
April 18, 2024:Even before legalization, most Minnesotans reported that cannabis was easy to obtain; only one-third disapproved of use by adults
During the past decade, the United States’ cannabis policy landscape has changed dramatically. By the end of 2023, 24 states had legalized cannabis for non-medical use by adults — meaning the majority of the U.S. population lives in a state with legalized recreational cannabis.
These changes in the landscape of U.S. cannabis policy have coincided with evolving public opinion and perceptions about cannabis and cannabis legalization. Researchers have documented changing public attitudes about cannabis policy. For example, according to the polling firm Gallup, the share of people in the U.S. who support legalization of marijuana has grown from 50% in 2012 to 70% in 2023, just over a decade later1. But the complexities of cannabis and the attitudes surrounding it are much more nuanced than simply whether people support or oppose cannabis legalization.
In 2023, Minnesota became the 23rd state to legalize cannabis for non-medical use by adults. To help policymakers and Minnesotans understand the potential public health implications of that policy change, researchers from the University of Minnesota School of Public Health’s State Health Access Data Assistance Center (SHADAC) and the newly formed Cannabis Research Center (CRC) have analyzed data on people’s perceptions and opinions relating to cannabis, both for Minnesota and the U.S. as a whole.
SHADAC and the CRC used data from the federal government’s National Survey on Drug Use and Health (NSDUH). This research so far has included a focus on pre-legalization data, to better understand the people’s perspectives, opinions, and experiences with cannabis before Minnesota’s policy shift. Using the NSDUH, we report pre-legalization baseline data on several issues and commonly cited concerns associated with cannabis legalization:
- Ease or difficulty of obtaining cannabis under a policy of prohibition
- Perceived risk of smoking cannabis on a weekly basis
- Disapproval, or lack of disapproval, of cannabis use by adults (age 18 and older) and youth (age 12-17)
These particular measures are important because they may offer hints about the potential public health effects of cannabis legalization. Much of the concern about legalization hinges on the assumption that it will increase cannabis use, in turn resulting in possible consequences such as increases in prevalence of cannabis use disorder. But is it not clear whether legalization will increase cannabis use in the Minnesota context, or whether increased cannabis use will result in subsequent harms.
Data on Minnesotans’ perceptions and opinions of cannabis can offer us clues as to how legalization might affect the state. In our analysis, we found that most Minnesotans age 12 and older reported that cannabis was very or fairly easy to obtain, even before it was legalized. That could mean that increased availability of cannabis through legalization might not have a substantial impact on use, as people already reported easy availability when cannabis was prohibited.
We also found that roughly half of Minnesotans believed that smoking cannabis once or twice a week carried no risk or only slight risk of harm. And, while our analysis found that only one in three Minnesota adults (age 18 and older) reported disapproving of adults using cannabis, four in five Minnesota youth (age 12 to 17) said they disapproved of peers using cannabis. That suggests that adults may be less inhibited to try cannabis than youth under legalization — though those attitudes could change.
Our plan is to continue monitoring the cannabis landscape in Minnesota, measuring the impacts of legalization and the consequences — positive or negative — for public health. The findings of this study offer us early hints, but it will be crucial to continue to research these issues once commercial sales of cannabis begin and as new data become available.
Find more details and data analysis in the full version of this brief by clicking on the image to the right, or at the link here.
Interested in Minnesota cannabis policy and research? Check out the following resources to learn more about this growing field:
Publication
Sexual Orientation and Gender Identity Data: New and Updated Information on Federal Guidance and Medicaid Data Collection Practices (SHVS Brief)

In the United States, over 13 million people identify as lesbian, gay, bisexual, or transgender (LGBT).1 Further, approximately 1.2 million LGBT adults (ages 18 - 64) are covered by Medicaid, and, of those, it is estimated that 152,000 (12.7%) identify as transgender.2
- a summary of the current landscape of SOGI data collection in Medicaid through an examination of all 50 states’ and Washington, D.C.’s paper Medicaid applications along with 44 states’ online Medicaid applications
- a spotlight on Oregon’s efforts to develop SOGI data standards
- a discussion of considerations for states wanting to implement these new SOGI questions into their Medicaid application(s)
Read the brief in full here.
About the SHVS:
[1] The Williams Institute at UCLA School of Law. (2019, December 16). LGBT FAQs - Williams Institute. Williams Institute. https://williamsinstitute.law.ucla.edu/quick-facts/lgbt-faqs/
[2] Medicaid and CHIP Payment Access Commission (MACPAC). (June 2022). Access in Brief: Experiences of Lesbian, Gay, Bisexual, and Transgender Medicaid Beneficiaries with Accessing Medical and Behavioral Health Care. https://www.macpac.gov/wp-content/uploads/2022/06/Access-in-Brief-Experiences-in-Lesbian-Gay-Bisexual-and-Transgender-Medicaid-Beneficiaries-with-Accessing-Medical-and-Behavioral-Health-Care.pdf
[3] Bosworth, A., Turrini, G., Pyda, S., Strickland, K., Chappel, A., De Lew, N., Sommers, B.D.. (June 2021). Health Insurance Coverage and Access to Care for LGBTQ+ Individuals: Current Trends and Key Challenges. https://aspe.hhs.gov/sites/default/files/2021-07/lgbt-health-ib.pdf
[4] U.S. Government. Executive Office of the President. “Advancing Equality for Lesbian, Gay, Bisexual, Transgender, Queer, and Intersex Individuals”. 87 Fed Reg 37,189-37,195. (June 22, 2022). https://www.govinfo.gov/app/details/FR-2022-06-21/2022-13391
[5] Centers for Medicare & Medicaid Services (2023). New Sexual Orientation and Gender Identity (SOGI) Questions on the Marketplace Application. https://www.cms.gov/files/document/sogi-questions-marketplace-application.pdf
[6] Center for Medicaid and CHIP Services (November 9, 2023). Guidance on Adding Sexual Orientation and Gender Identity Questions to State Medicaid and CHIP Applications for Health Coverage. https://www.medicaid.gov/sites/default/files/2023-11/cib11092023.pdfBlog & News
2023 NHIS Early Release: Estimates from Quarter 3 (July to September) Hold Steady
April 01, 2024:The National Center for Health Statistics (NCHS) has released quarterly estimates of health insurance coverage beginning in July 2022 through September 2023 from the National Health Interview Survey (NHIS) as part of the NHIS Early Release Program. Each quarter covers a three-month span, and this blog specifically looks at survey data from the most recent quarter (Q3 - July to September 2023) and notes any differences compared to the same time period in 2022.
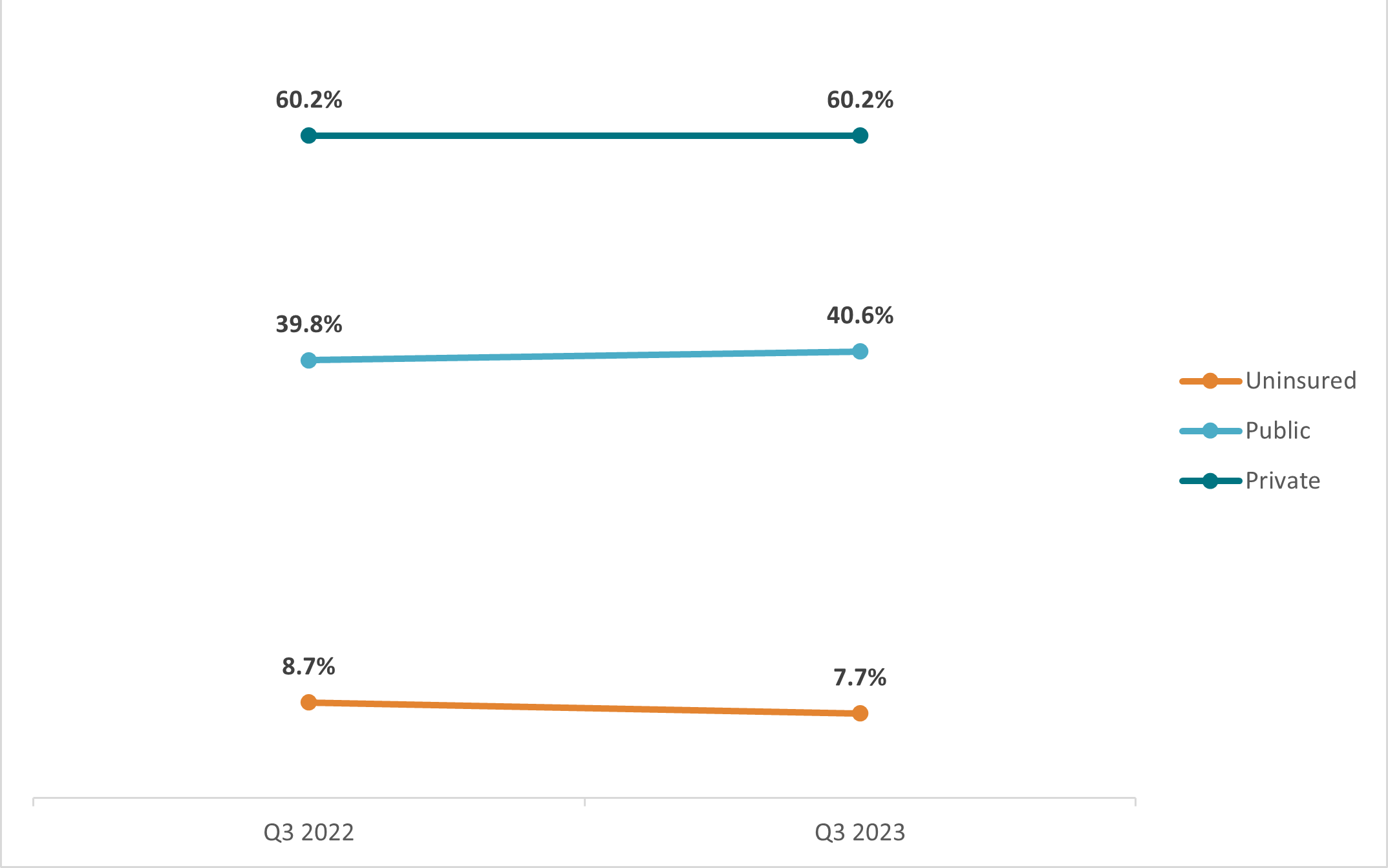
Between Q3 of 2022 and Q3 of 2023, rates of uninsurance, public coverage, and private coverage for adults (age 18-64) remained mostly unchanged. There was a small increase in the rate of public coverage for all ages and a small decrease in the rate of uninsurance overall, but these changes were not statistically significant.
Figure 1: Health Insurance Coverage Rates by Type (Adults Age 18-64), Q3 2022 vs. Q3 2023
[1] Centers for Medicare & Medicaid Services (CMS). (2023, December 18). Medicaid and CHIP Enrollment: Child and Youth Data Snapshot. https://www.medicaid.gov/sites/default/files/2023-12/medicaid-unwinding-child-data-snapshot.pdf
Blog & News
Minnesota Community and Uninsured Profile Updated to Include 2022 American Community Survey Estimates
March 04, 2024:|
|
 |
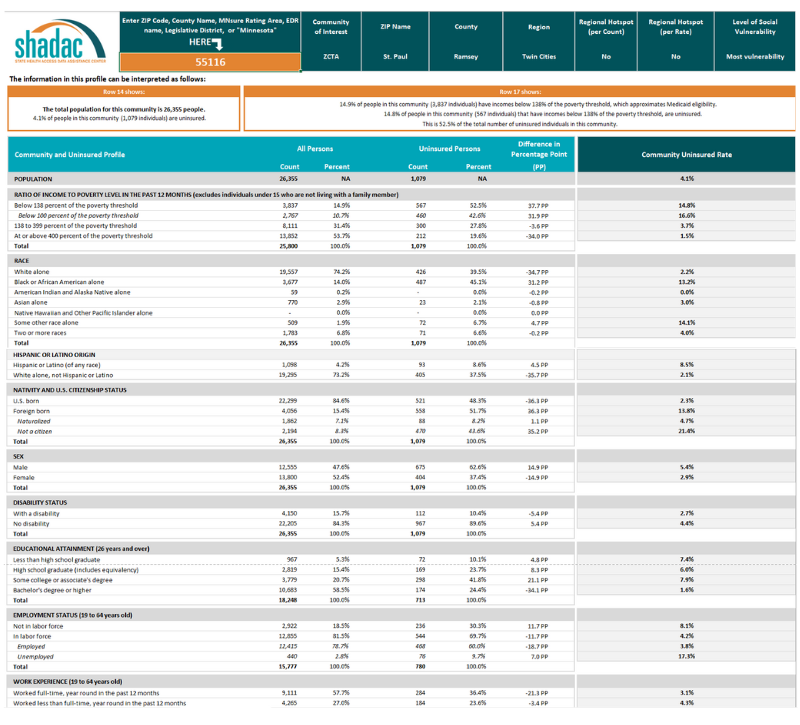 |
- Provide information on Minnesota uninsured people and populations
- Assist policymakers in developing & evaluating enrollment and outreach strategies
- Understand uninsured community and population characteristics in Minnesota
- Create a tool that can be used to understand and evaluate equity work, inform strategic planning, assess community needs, and support grant writing for related and relevant programs
- How to Use - an overview on using the uninsured profile to both identify and gather information communities of interest
- Community and Uninsured Profile - the profile itself with breakdowns at the county, MNsure rating area, ZIP code, economic development region, and state levels
- ZIP Code Uninsured Rates - includes all reported Census-defined ZIP Codes, regions, and counties in Minnesota along with both the number and percent of uninsured within those communities