Blog & News
Unemployment Rate Trends of the Past 5 Years: Pre-, Mid-, and Post-Pandemic
April 01, 2024:In early 2020, the COVID-19 pandemic ended the United States’ decade-long era of economic expansion. Many businesses across industries halted or closed operations, resulting in record-high temporary and permanent job losses – events that have been reflected in unemployment rate trends.
Primarily, unemployment affects people’s economic stability and well-being, but it goes beyond that. Unemployment affects individuals’ access to stable housing, food security, and health insurance coverage and care. Unemployment has also been linked to negative health consequences, with unemployed individuals often reporting feelings of depression and anxiety, and suffering from stress-related illness such as high blood pressure, stroke, heart attack, heart disease, and arthritis more often compared to employed counterparts
Knowing that unemployment affects health and health care access, we wanted to understand how such a seismic event as the pandemic affected unemployment rates. We also wanted to determine what progress has been made in recovery post-pandemic. To do this, SHADAC used our State Health Compare tool’s unemployment measure, looking at data pre- (2018-2019), mid- (2020), and post-pandemic (2021-2022). Keep reading to learn more about our process and key findings.
Unemployment Rate Trends: Overall Rate Rose Sharply During Pandemic
Before the pandemic began, the United States was experiencing what the Bureau of Labor Statistics (BLS) called, “the second longest [period of] economic expansion on record,” with the unemployment rate reaching a 49-year low. Overall, the pre-pandemic national unemployment rates in 2018 and 2019 were 3.9% and 3.7%, respectively. In 2020, what we have termed as during / mid-pandemic, the unemployment rate rose sharply to 8.1%. As time went on, though, unemployment rates began to noticeably decrease, measuring at 5.3% in 2021 and dipping below 2019’s low to 3.6% in 2022.
It is no surprise that national unemployment was at its highest mid-pandemic in 2020 as a result of business closures (both temporary and permanent). However, some heartening news comes from the 2022 data showing a national unemployment rate sitting the lowest it had been in the past five years, and several other key labor market measures also returning to their pre-pandemic levels.
While encouraging, when looking at unemployment rates pre-, mid-, and post-pandemic, it is worthwhile to go beyond the seemingly straightforward, positive picture at the national level in order to understand how different geographic and demographic populations varied in unemployment rates. For our analysis, we looked at unemployment rate by state and by race/ethnicity.
Examining Unemployment Rate Trends by State
The following tables show the five states with the lowest and the highest unemployment rates each year from 2018 to 2022.
| Lowest | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| 2018 | 2019 | 2020 | 2021 | 2022 | |||||
| Hawaii | 2.4% | North Dakota | 2.4% | Nebraska | 4.2% | Nebraska | 2.5% | North Dakota | 2.1% |
| Iowa | 2.5% | Vermont | 2.4% | South Dakota | 4.6% | Utah | 2.7% | South Dakota | 2.1% |
| New Hampshire | 2.5% | New Hampshire | 2.5% | Utah | 4.7% | South Dakota | 3.1% | Nebraska | 2.3% |
| North Dakota | 2.6% | Utah | 2.6% | North Dakota | 5.1% | Kansas | 3.2% | Utah | 2.3% |
| Vermont | 2.7% | Hawaii | 2.7% | Iowa | 5.3% | Alabama | 3.4% | Missouri | 2.5% |
| Highest | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| 2018 | 2019 | 2020 | 2021 | 2022 | |||||
| Louisiana | 4.9% | New Mexico | 4.9% | Michigan | 9.9% | Dist. of Columbia | 6.6% | Pennsylvania | 4.4% |
| New Mexico | 4.9% | West Virginia | 4.9% | New York | 10.0% | New Mexico | 6.8% | Delaware | 4.5% |
| West Virginia | 5.3% | Mississippi | 5.4% | California | 10.1% | New York | 6.9% | Illinois | 4.6% |
| Dist. of Columbia | 5.6% | Dist. of Columbia | 5.5% | Hawaii | 11.6% | Nevada | 7.2% | Dist. of Columbia | 4.7% |
| Alaska | 6.6% | Alaska | 6.1% | Nevada | 12.8% | California | 7.3% | Nevada | 5.4% |
Certain unemployment rate trends have remained consistent in the last two years of the post-pandemic period, which could shed light on individual states’ economic recovery post-pandemic. For example, Nebraska and South Dakota have been among the five states with the lowest unemployment rates mid- & post-pandemic, suggesting less economic fallout from the pandemic. On the other hand, Nevada has ranked in the five states with the highest unemployment rates post-pandemic (2021 and 2022), suggesting perhaps a slower economic recovery due to COVID-19.
Case Study of Nevada: Misleading Overall Data
While a state’s overall unemployment rate may tell one story, a further breakdown into individual racial/ethnic subgroups may tell another, as we can see with Nevada.
Nevada’s total unemployment rate for 2021 was 7.2%, which was among the five states with the highest rate of unemployment for that year. However, the 2021 unemployment rate for White individuals in Nevada measured at 6.6% – lower than the overall state-level rate. In stark contrast, the 2021 unemployment rate for African American/Black individuals in Nevada measured at 15.3% – more than double the rates of White individuals in Nevada and the state’s overall unemployment rate.
Examining Unemployment Rate Trends by Race/Ethnicity
As observed in Nevada, a breakdown of unemployment rates by race/ethnicity gives insight to the disparities experienced by certain racial/ethnic subgroups. African American/Black, Hispanic, and Native American* individuals were more likely to suffer job loss compared to White workers during the pandemic. Adverse health outcomes and difficulty accessing healthcare are associated with longer periods of unemployment, which Black, Hispanic, and Native American workers endured more than White workers. Thus, it is important to consider the breakdown of race/ethnicity in relation to unemployment, especially when analyzing mid- and post-pandemic data.
While population-level unemployment rates may seem relatively low post-pandemic, a breakdown by race/ethnicity can reveal inequities and more detailed information regarding unemployment in the United States. The following chart shows the year-by-year total breakdown of unemployment by race/ethnicity, as well as the national rate for reference.
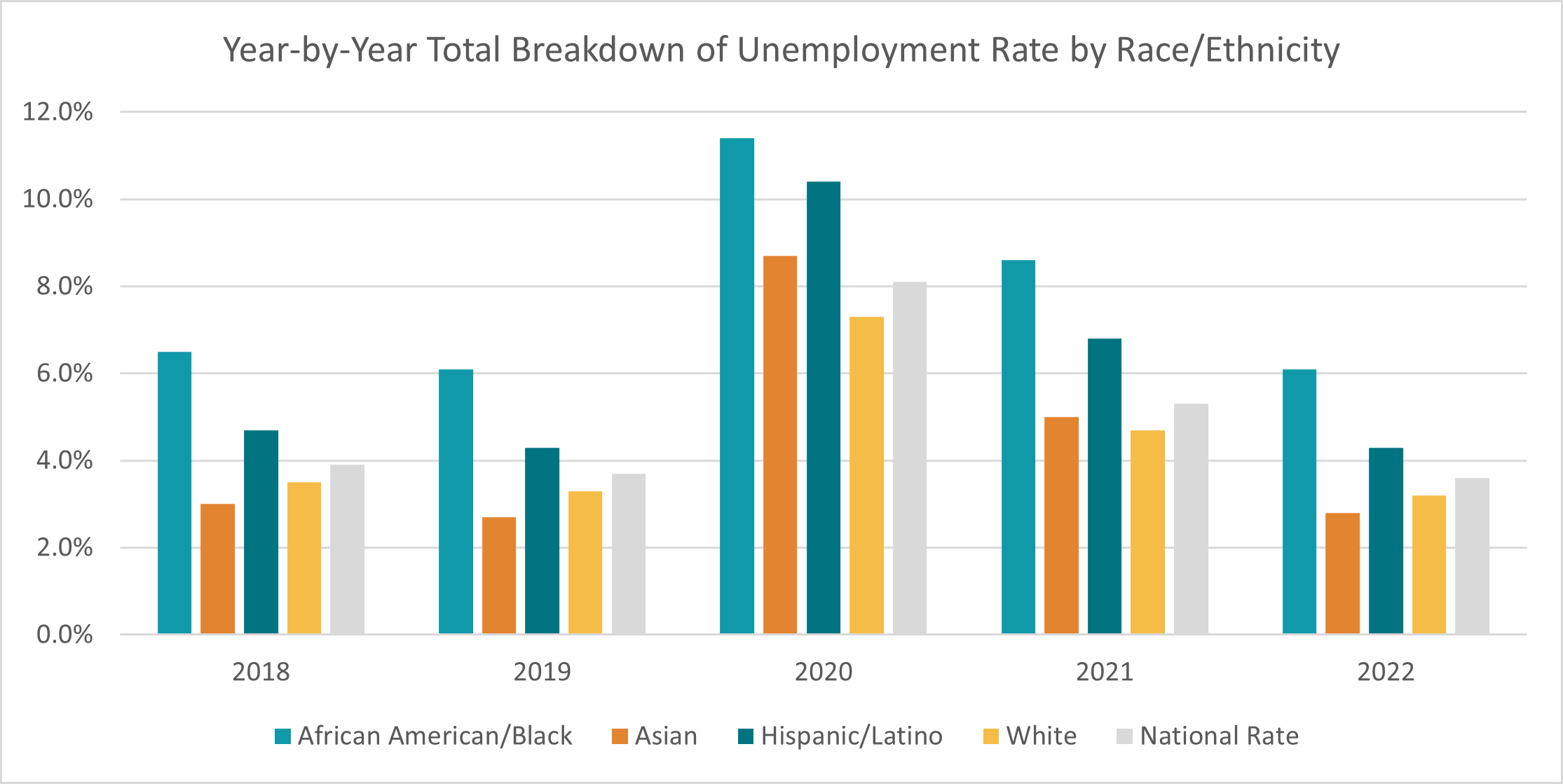
All four racial/ethnic groups follow the nationally observed unemployment trend: mid-pandemic (2020) rates are the highest, and, by 2022, unemployment had returned to pre-pandemic (2018 and 2019) levels.
However, deeper analyses of these five-year trends reveal disparities for certain racial/ethnic subgroups. For example, White individuals are the only racial/ethnic group to have their lowest national unemployment rate in the last five years be post-pandemic (3.2% in 2022). Compare that to African American/Black adults and Hispanic/Latino adults who, in the same year of 2022, have had higher unemployment rates (6.1% and 4.3%, respectively) than the national U.S. rate (3.6%). White and Asian adults have had lower unemployment than the U.S. rate for the last five years, except in 2020 where the unemployment rate for Asian adults was 8.7% compared to the U.S. rate of 8.1%.
Conclusion
Due to the implications that unemployment has on health and health care, it is important to consider the disparities in rates among different racial/ethnic groups. Even in states where unemployment may seem to be trending down, this rate could be misleading when not accounting for race/ethnicity.
Overall, national unemployment has returned to pre-pandemic rates, and the same trend has been observed across racial/ethnic groups. However, unemployment rates for African American/Black and Hispanic/Latino individuals are still consistently higher than the U.S. rate, revealing the need for targeted attention toward addressing unemployment rates for these populations.
To learn more about this and other related subjects, check out the following products on our site:
- Six Measures on SHADAC’s State Health Compare Now Updated to Include Pandemic-era Data for Health Behaviors and Outcomes
- Revised Childhood Vaccinations Measure on State Health Compare Shows Vaccination Rates Vary by State, Race/Ethnicity, and Insurance Coverage
- The Opioid Crisis in the Pandemic Era
You can also explore these and many other data measures with our State Health Compare tool here.
*State Health Compare does not currently have available data for Native American individuals, due to low response rate. However, SHADAC is hopeful this data gap will be addressed in the future in order to conduct equitable analyses.
Blog & News
2020 Public Use Microdata Area (PUMA) Updates in the 2022 American Community Survey
March 26, 2024:A Public Use Microdata Area (PUMA) is a type of geographic unit created for statistical purposes. PUMAs represent geographic areas with a population size of 100,000–200,000 within a state (PUMAs cannot cross state lines). PUMAs are the smallest level of geography available in American Community Survey (ACS) microdata. They are designed to protect respondent confidentiality while simultaneously allowing analysts to produce estimates for small geographic areas.
Every ten years, the decennial census results are used to redefine ACS PUMA boundaries to account for shifts in population and continue to maintain respondent confidentiality. This process is intended to yield geographic definitions that are meaningful to many stakeholders.
Most recently, new PUMAs were created based on the 2020 Census; these 2020 PUMAs were implemented in the ACS starting in the 2022 data year. Although Public Use Microdata Area components remain consistent to the extent possible, they are updated based on census results and revised criteria. Therefore, they are not directly comparable with PUMAs from any previous ACS data years. For example, the 2020 PUMAs used in the 2022 data year are distinct from the 2010 PUMAs, which were used in the 2012–2021 ACS data years.
The 2020 PUMAs were created based on definitions that include two substantive changes relative to the 2010 PUMAs:
1) An increase in the minimum population threshold for the minimum size of partial counties from 2,400 to 10,000. Increasing the population minimum for a PUMA-county part aims to further protect the confidentiality of respondents. However, exceptions are allowed on a case-by-case basis in order to maintain the stability of PUMA definitions (that were based on the previous minimum of 2,400) and due to unique geography.
2) Allowing noncontiguous geographic areas. Allowing PUMAs to include noncontiguous geographic areas aims to avoid unnecessarily splitting up demographic groups in order to provide more meaningful data. This change is not intended to create highly fragmented PUMAs.
Other than the two changes listed above, PUMA criteria remained consistent, such as treating 100,000 as a strict minimum population size for PUMAs. The maximum population size for PUMAs can exceed a population of 200,000 in certain instances due to expected population declines or geographic constraints.
Generally, counties and census tracts are the building block geographies for PUMAs. This maximizes the stability of PUMA boundaries and therefore reduces disclosure risks. Counties may be combined or split as needed, depending on population size. Additionally, PUMAs are designed to avoid unnecessarily splitting metropolitan areas, minor civil divisions (MCDs) with a functional government, and areas of American Indian/Alaska Native (AIAN) and Native Hawaiian people. Carlton County in Minnesota, for example, illustrates that splitting a county was necessary to avoid splitting Fond du Lac reservation into multiple PUMAs (U.S. Census Bureau, 2022).
Figure 1: Minnesota PUMA 00400 Includes Fond du Lac Reservation in Its Entirety
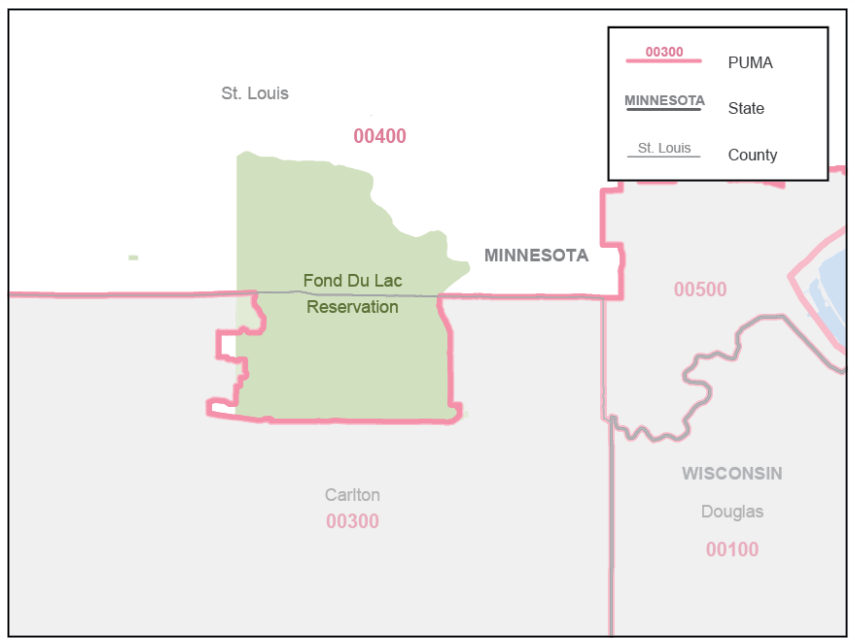
Note: Minnesota PUMA 00400 featuring Fond Du Lac Reservation in its entirety. Reprinted from Final Criteria for Public Use Microdata Areas for the 2020 Census and the American Community Survey from https://www2.census.gov/geo/pdfs/reference/puma2020/2020PUMA_FinalCriteria.pdf.
Due to periodic changes in Public Use Microdata Area boundaries, states as a whole are the most granular geographic variable in the ACS microdata that can be compared consistently across all years. However, IPUMS USA offers harmonized geographic variables that greatly expand the options for analyzing ACS data across both time and geography. These variables are less granular than PUMAs, but more granular than states. For example, CONSPUMA and CPUMA0010 combine ACS PUMAs to create consistent geographies that can be compared across multiple decades of PUMA definitions; these have not yet been updated to include the new 2020 PUMAs. Currently, CITY, COUNTYFIP, and MET2013 allows users to compare cities, counties, and metropolitan areas, respectively, over years 2005-2022.
IPUMS USA also provides in-depth geographic resources for ACS data users, including interactive maps of the 2010 and 2020 PUMAs. For example, below is a map of the Twin Cities metropolitan area, Minnesota, showing 2020 PUMAs in blue and 2010 PUMAs in orange (IPUMS USA, 2020). This map illustrates that the updated PUMA criteria resulted in changes to PUMA boundaries in urban areas and some aggregation of PUMAs in more rural areas.
Figure 2: IPUMS USA Map of Twin Cities Metropolitan Area, Minnesota 2010 and 2020 PUMAs
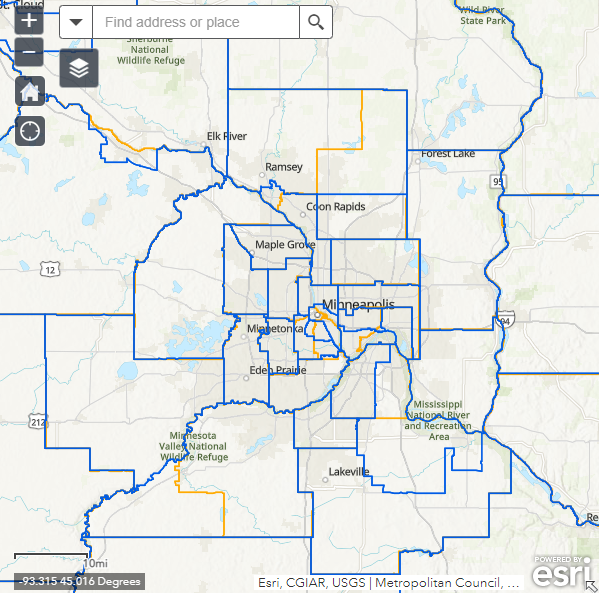
Note: IPUMS USA Map of Twin Cities Metropolitan Area, Minnesota 2010 and 2020 PUMAs. Reprinted from 2020 PUMA DEFINITIONS: WEB MAP OF 2010 AND 2020 PUMAS from IPUMS USA, https://usa.ipums.org/usa/volii/pumas20.shtml.
Looking for other data and information from the American Community Survey? Learn more with the following SHADAC products:
2022 ACS Tables: State and County Uninsured Rates
American Indian/Alaska Native (AIAN) and Native Hawaiian and Other Pacific Islander (NHPI) data added to State Health Compare ACS estimates
Explore the Data on State Health Compare
Sources:
U.S. Census Bureau. (2022, July 25). Final Criteria for Public Use Microdata Areas for the 2020 Census and the American Community Survey. https://www2.census.gov/geo/pdfs/reference/puma2020/2020PUMA_FinalCriteria.pdf
IPUMS USA (2020). 2020 PUMA Definitions: Web Map of 2010 and 2020 PUMAs. https://usa.ipums.org/usa/volii/pumas20.shtml.
Blog & News
Now Available on State Health Compare: New 2022 Estimates from the ACS and CPS
March 04, 2024:
2022 estimates from the American Community Survey (ACS) and Current Population Survey (CPS) are now available for eight measures on SHADAC’s State Health Compare.
Updated measures using new ACS data include:
![]() Coverage Type
Coverage Type
Health insurance coverage by type of coverage (private, public, employer-sponsored, Medicare, Medicaid/CHIP, individual, and uninsured) available by a variety of breakdowns, including by income, disability status, race/ethnicity, and more.
![]()
Broadband Internet Access
This measure allows the user to view state-level percentages of people who have access to high-speed internet, which is an increasingly important tool for individuals to access health care (via telehealth), find employment, and connect with a range of other services. The measure has multiple layers of breakdowns by income, disability status, and metropolitan status, among others.
Child Poverty
Children who experience poverty can be more prone to many different negative health outcomes, often lacking in access to health care, education, shelter, sanitation, and more compared to children not considered to be in poverty. This is a vulnerable population that needs to be monitored continuously. This measure provides state-level data on children <100% Federal Poverty Guideline for both the total population and by race and ethnicity.
![]() Income Inequality
Income Inequality
Lower incomes are correlated to effects like housing instability, food insecurity, and more that can lead to negative health outcomes. This measure presents state-level data on income inequality as measured by the Gini coefficient.
![]()
Unaffordable Rents
Stable housing is a key component of health and wellbeing. Unaffordable Rents on State Health Compare measures the share of renters who may be struggling to afford their rents, thus contributing to unstable housing. This measure is available by a number of policy-relevant breakdowns, including race/ethnicity, Medicaid enrollment, and household income.
Updated measures using new CPS data include:
Percent of People with High Medical Cost Burden
Out-of-pocket spending on health care can make up a large share of income, creating burdens for those with large health care expenses. This measure can help us understand trends and disparities in healthcare affordability. These data are available both by insurance coverage type and by race/ethnicity.
![]() Median Medical Out-of-Pocket (OOP) Spending
Median Medical Out-of-Pocket (OOP) Spending
This measure shows the amount that the typical individual spends using their own money on health care costs, including health insurance coverage premiums, forms of insurance cost sharing (e.g., co-pays, deductibles), and services not covered by health insurance and/or paid by uninsured individuals. The 2022 estimates are available to be viewed by total and specifically by those with employer-sponsored insurance.
![]()
Health Status
Stable housing is a key component of health and wellbeing. Unaffordable Rents on State Health Compare measures the share of renters who may be struggling to afford their rents, thus contributing to unstable housing. This measure is available by a number of policy-relevant breakdowns, including race/ethnicity, Medicaid enrollment, and household income.
Be sure to check out a recent analysis of new data where we add context to the Health Insurance Coverage by Race/Ethnicity measure.
Other Related Reading:
Blog & News
New Data on Health Insurance Coverage by Race/Ethnicity Added to State Health Compare
February 13, 2024:State Health Access Data Assistance Center (SHADAC) has added two new racial/ethnic population groups to our measures of health insurance coverage available on State Health Compare.
Using micro-data from the American Community Survey (ACS), we were able to add health insurance coverage measures for American Indian/Alaska Native (AIAN) and Native Hawaiian Pacific Islander (NHPI) populations. Specifically, SHADAC has added insurance coverage data for AIAN and NHPI populations at both the national and state level (when sample size permits) from the years 2008-2022. Estimates for these groups are also available by age and poverty status.
This update now allows users to download estimates of insurance coverage for all of the minimum race categories for data collection outlined by the Office of Management and Budget (OMB), which are: American Indian or Alaska Native (AIAN), Asian, Black or African American, Native Hawaiian or Other Pacific Islander (NHPI), and White.
| Uninsured adults (19-64) in the US, 2021-2022 | ||||||
|---|---|---|---|---|---|---|
| Race/ethnicity | Age | 2021 | 2022 | Difference | * | |
| AIAN | 19-64 | 24.5% | 22.2% | -2.4 | * | |
| African-American / Black | 19-64 | 13.4% | 12.1% | -1.3 | * | |
| Asian | 19-64 | 7.2% | 6.7% | -0.5 | * | |
| Hispanic / Latino | 19-64 | 24.4% | 22.8% | -1.5 | * | |
| NHPI | 19-64 | 12.1% | 13.6% | 1.5 | ||
| Other / Multiple Races | 19-64 | 11.2% | 10.5% | -0.7 | * | |
| White | 19-64 | 8.2% | 7.4% | -0.7 | * | |
| All | 19-64 | 12.0% | 11.2% | -0.9 | * | |
| * Significant difference between years. Source: SHADAC analysis of the 2021-2022 American Community Survey. |
||||||
In this analysis, we used this newly available data from State Health Compare to examine differences in uninsurance from 2021 to 2022 by race/ethnicity for adults ages 19-64. Over this period, the overall uninsured rate for non-elderly adults dropped nearly a percentage point, reaching 11.2%. The largest drop in uninsurance was seen among AIAN adults, lowering by 2.4 percentage points. Hispanic and Black adults also saw improvements in coverage of greater than one percentage point (1.5 and 1.3 percentage points, respectively). More modest gains in coverage were reported by adults who were White, Asian, and Other/Multiple races.
Significant decreases were seen consistently across populations by race/ethnicity except for the NHPI adult population, which did not see this same decrease in uninsurance. While estimates were limited by sample size and changes were not significant, uninsurance rates for this group increased from 12.1% to 13.6%. These concerning rates of uninsured NHPI adults contrasted with the overall trend of decreased uninsurance rates and thus warrant further observation.
While encouraging to see a trend of decreasing uninsurance amongst non-elderly adults, disparities in insurance coverage between racial/ethnic groups are persistent. For example, in 2022, more than one in five adults were uninsured among both the Hispanic/Latino and AIAN populations. Uninsurance was also high for NHPI and Black adults, at 13.6% and 12.1%, respectively. The substantial differences in coverage between racial/ethnic populations illustrate the ongoing priority of improving health equity, including health care access. We plan to continue monitoring insurance coverage in light of ongoing post-pandemic policy changes. Providing more granular estimates by race/ethnicity will support efforts to understand and reduce disparities in health care access.
Publication
SHADAC’s Primary Source of Coverage Hierarchy for American Community Survey (ACS) Estimates on State Health Compare
 This updated brief from SHADAC defines a “primary source of coverage hierarchy,” and how and when researchers can use this tool to determine which payer is primary when an individual reports multiple sources of health insurance coverage on the American Community Survey (ACS).
This updated brief from SHADAC defines a “primary source of coverage hierarchy,” and how and when researchers can use this tool to determine which payer is primary when an individual reports multiple sources of health insurance coverage on the American Community Survey (ACS).
Using a hierarchy provides multiple benefits for researchers, including the ability to ensure that individuals who report having multiple types of coverage are only counted once, reducing the rate of over-reporting for a specific type of coverage, and making coverage estimates more comparable across different surveys. However, SHADAC researchers caution that there is not one specific, singular hierarchy that should always be imposed; rather, there are a multiplicity of possible hierarchies with orders of coverage varying based on the research focus and requirements of each individual analysis (e.g., if a researcher would like to look at a range of coverage over time, or examine coverage for a singular year or specific subpopulations).
When performing national, state, and sub-state analysis of ACS coverage data, SHADAC imposes a particular coverage hierarchy that places respondents into two categories, age 0-18 and age 19 and older, and then ranks possible coverage options—Medicare, Medicaid/CHIP, Employer/Military (TRICARE, VA), Direct purchase, and Uninsured —in descending order for which respondents in each age group will be sorted.
The reason for this separation by age is that for all adults age 19 and older, Medicare is considered the primary source as it is the primary payer for covered medical services. Children age 0-18 are not eligible for Medicare (except in one rare and specific instance) and therefore Employer/Military is considered primary, as many dependents draw this source of coverage from an adult parent or caregiver.
In addition to exploring the different hierarchy possibilities, the brief also walks the user through an example application of SHADAC’s coverage hierarchy on data from the 2022 American Community Survey, and how this affects the rates of reported coverage for each insurance source for the two age groups, both separately and together.
For more on the data produced using SHADAC’s primary source of coverage hierarchy, visit our State Health Compare web tool and explore the “Health Insurance Coverage Type” measure.
Download a PDF of SHADAC’s Coverage Hierarchy for American Community Survey (ACS) Estimates on State Health Compare brief.













